What toxic stress means in biological terms — and why it's not just "severe stress"
When we talk about stress in everyday life, we usually mean a subjective feeling of tension, anxiety, or overload. But in scientific literature, stress is the activation of specific biological systems, primarily the hypothalamic-pituitary-adrenal axis (HPA axis), which triggers the release of cortisol (S001, S005).
Intuitively we understand that stress is bad, but the scientific community still hasn't reached a unified definition of what exactly constitutes stress, which forms are adaptive, and which are destructive. More details in the Climate and Geology section.
🧬 Physiological stress: what happens in your body when you're "nervous"
Physiological stress is the activation of the HPA axis and the sympathetic nervous system. When the brain perceives a threat (real or imagined), the hypothalamus releases corticotropin-releasing hormone (CRH), which stimulates the pituitary gland to release adrenocorticotropic hormone (ACTH).
ACTH causes the adrenal glands to produce cortisol — the primary stress hormone. Cortisol mobilizes energy resources, raises blood glucose levels, suppresses non-priority functions (digestion, immunity, reproduction), and prepares the body for a "fight or flight" response. Normally, this mechanism is adaptive: it helps you survive dangerous situations.
The problem begins when activation becomes chronic.
⚠️ Toxic stress: when a protective mechanism turns into poison
Toxic stress isn't just "really severe stress." It's a specific pattern: excessive or prolonged activation of stress systems in the brain and body, occurring without buffering supportive relationships (S005).
- Key difference from ordinary stress
- not intensity, but chronic activation without recovery periods
- Result
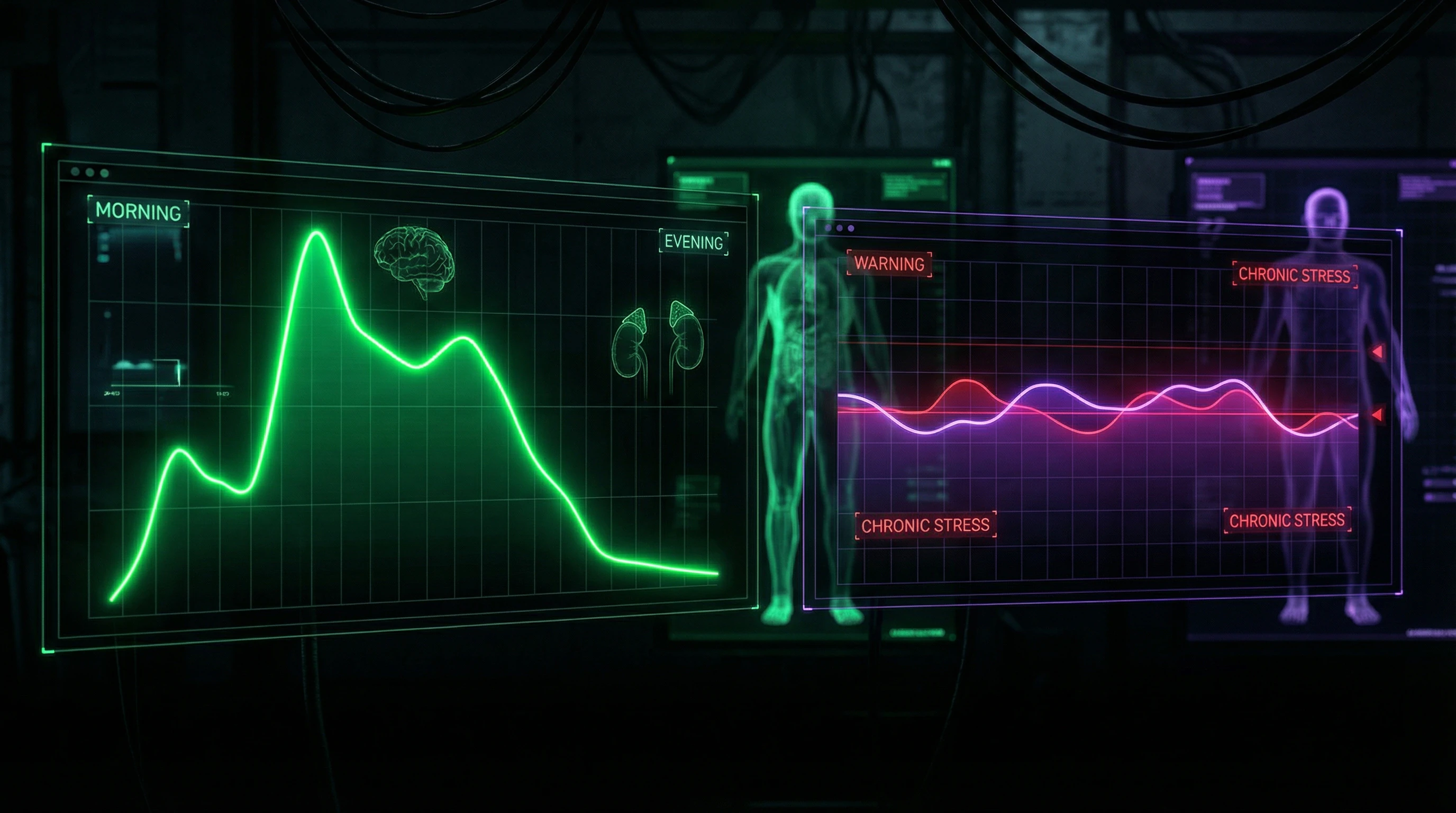
- dysregulation of cortisol patterns: instead of a healthy circadian rhythm (peak in morning, decline toward evening), flattened curves, blunted peaks, and flat slopes are observed
- Consequence
- associated with increased morbidity (S008)
🔬 Cortisol as a biomarker: what scientists measure when they talk about stress
Cortisol is the gold standard stress biomarker in research. It can be measured in saliva, blood, urine, or hair, with salivary cortisol being particularly convenient for non-invasive monitoring.
| Parameter | Healthy profile | Sign of chronic stress |
|---|---|---|
| Morning peak | Pronounced (30–45 min after waking) | Blunted or absent |
| Diurnal slope | Gradual decline throughout the day | Flattened; elevated evening levels |
| Disease association | Low morbidity | Depression, CVD, increased mortality (S008) |
It's important to understand: cortisol itself isn't a "bad" hormone. The problem is dysregulation of its rhythm. The connection between attachment styles and hormonal regulation shows that the quality of early relationships programs this capacity for recovery for life.
Seven Arguments That Relationships Actually Affect Your Hormonal Profile
The idea that a partner can "infect" you with their stress at a biological level sounds counterintuitive. Here are the strongest arguments supporting this hypothesis. More details in the Cellular Biology section.
🔬 Argument 1: Direct measurements show correlation between partner stress and your cortisol
A study by Shrout and colleagues (2020) directly measured cortisol levels in married couples throughout the day and found: perceived partner stress predicts an individual's cortisol slopes independently of their own stress level (S011, S012). This isn't a correlation between two subjective assessments, but a link between one person's subjective stress and another's objective biomarker.
The effect persisted even after controlling for multiple variables, including relationship conflict and individual characteristics.
🧠 Argument 2: Emotional contagion is a documented phenomenon with a neurobiological basis
People automatically "read" the emotional state of those close to them through facial microexpressions, tone of voice, and body posture. This is subconscious synchronization of physiological states, not just empathy at the conscious level.
Observing another person's stress can activate the observer's own stress response, including cortisol release (S014). In the context of close relationships, where contact is daily and prolonged, this effect intensifies.
📊 Argument 3: Attachment style modulates stress response to relationships
People with insecure attachment styles (anxious or avoidant) demonstrate higher cortisol release in response to relationship stressors compared to those with secure attachment (S014).
- Not everyone is equally vulnerable to "stress contagion" from a partner
- Individual differences in the attachment system create varying degrees of permeability to others' stress
- Anxiously attached individuals are particularly sensitive to threat signals in relationships
🧬 Argument 4: Emotion suppression in relationships is linked to cardiovascular disease
Emotion suppression in the context of relationships is associated with increased risk of cardiovascular disease (S004). When you systematically hide your feelings from a partner, it creates chronic physiological burden.
You activate stress systems without the possibility of discharge through social support—a classic pathway to toxic stress.
⚙️ Argument 5: Chronic relationship conflict predicts cortisol dysregulation
Couples with high levels of conflict demonstrate flatter cortisol slopes and blunted morning peaks (S011, S012). The conflict pattern in a couple creates a shared stressful environment that affects both partners.
This isn't about occasional arguments, but about a chronic pattern of negative interaction that becomes a background stressor.
🔁 Argument 6: Social hierarchy stability modulates the link between status and stress
A study by Knight and colleagues (2017) showed that social hierarchy stability modulates the impact of status on stress and performance (S007). In unstable hierarchies, even high status doesn't protect against stress.
- Applied to relationships:
- If power dynamics in a couple constantly shift, if roles are unclear or contested, this creates additional stress. Toxic relationships are often characterized by precisely this instability—you never know what rules apply, what to expect.
🧪 Argument 7: "Shift-and-persist" strategies show that social context can buffer stress
Research on low-status groups shows that "shift-and-persist" strategies (reappraising the stressor + maintaining optimism and meaning) can buffer the negative effects of chronic stress (S007).
It's not stress itself that determines the outcome, but the presence or absence of protective factors. A supportive partner can be such a buffer; a toxic one, conversely, strips you of this protection and becomes a source of stress themselves.
Evidence Base: What We Know for Certain and Where Questions Remain
Moving to a detailed examination of the evidence. Each claim is supported by a source; we'll indicate where the data are strong and where gaps remain. More details in the Space and Earth section.
📊 Shrout et al. (2020) Study: Partner Stress Predicts Your Cortisol
A key study in Psychoneuroendocrinology examined 191 heterosexual couples over several days (S011, S012). Participants collected saliva samples to measure cortisol at four time points (waking, +30 minutes, midday, evening) and completed questionnaires about perceived stress.
Results: partner's perceived stress significantly predicted an individual's cortisol slopes independent of their own stress. The effect was stronger in couples with high conflict levels—direct evidence that partner stress affects your physiology.
🧬 Emotional Contagion Mechanism: From Mirror Neurons to Cortisol
Emotional contagion is an automatic process whereby one person's emotional state induces a similar state in another (S014). The neurobiological basis: mirror neurons and empathy systems activate when observing others' emotions.
But this isn't just subjective experience. Observing another's stress can activate the observer's own HPA axis and trigger cortisol release. In close relationships, the effect is amplified by three factors:
- Frequency and duration of contact
- Emotional significance of the partner
- Shared environment with common stressors
🧠 Attachment Style as a Modulator of Stress Vulnerability
Attachment theory predicts: individuals with insecure styles (anxious or avoidant) are more reactive to relationship stressors (S014). Empirical data confirm—individuals with insecure attachment demonstrate higher cortisol release in response to conflict or relationship threats.
Anxious attachment is associated with hyperactivation of the attachment system and constant monitoring for threats to closeness; avoidant attachment involves suppression of closeness needs, creating internal conflict. Both patterns lead to chronic activation of stress systems in relationship contexts.
More on the neurobiology of attachment in a separate article.
⚠️ Emotional Suppression: The Hidden Cost of "Saving Face"
Emotional suppression is a strategy where a person conceals outward expression without changing internal experience (S004). Chronic suppression in relationships is associated with increased cardiovascular disease risk.
| Mechanism | Consequence |
|---|---|
| Suppression requires constant effort | Activates sympathetic nervous system, raises blood pressure |
| Partner doesn't see your discomfort | Cannot provide support |
| Absence of support | Stress accumulates, creating a vicious cycle |
🔁 Relationship Conflict and Cortisol Dysregulation: Cause or Effect?
The link between conflict and cortisol dysregulation is well documented (S011, S012), but the direction of causality isn't always clear. Three scenarios are possible:
- Scenario 1: Conflict → cortisol dysregulation
- Stress causes hormonal shifts.
- Scenario 2: Cortisol dysregulation → conflict
- Disrupted cortisol impairs emotion regulation and cognitive control, making conflicts more likely.
- Scenario 3: Bidirectional relationship (vicious cycle)
- Chronic conflict activates stress systems; dysregulated cortisol increases conflict proneness. This is a classic example of systemic dynamics where it's impossible to isolate a "root cause."
The third option is most likely. Data point to positive feedback where each element amplifies the other.

Mechanisms: How Exactly Your Partner's Stress "Gets Under Your Skin"
Real causal relationships differ from correlation through specific transmission pathways. Here are four mechanisms through which one person's stress restructures another's physiology. More details in the Epistemology Basics section.
🧬 Pathway 1: Emotional Contagion Through Mirror Neurons
When your partner is tense, your mirror neurons automatically simulate their state—this is a subcortical reaction within milliseconds, requiring no conscious participation. Mirror neuron activation triggers a cascade: amygdala (fear center) → hypothalamus → CRH release → pituitary → ACTH → adrenal glands → cortisol (S005).
The entire pathway activates from observing someone else's stress, without any direct stressor affecting you.
⚙️ Pathway 2: Shared Environment and Joint Stressors
Partners share financial problems, housing conditions, child-rearing, conflicts with relatives. If one experiences stress, the other is exposed to the same factors, even if they perceive them less acutely.
One person's stress reformats the shared environment: irritability, emotional unavailability, failure to fulfill responsibilities—this creates new stressors for the other partner.
🔁 Pathway 3: Destruction of Buffering Mechanisms
The primary protective factor against toxic stress is supportive relationships (S005). A healthy partner regulates your emotions, provides practical help, creates a sense of safety.
But a stressed partner cannot perform this function. They demand support you cannot provide; create conflicts; ignore your needs. The relationship transforms from a source of protection into a source of stress.
| Healthy Relationships | Toxic Relationships |
|---|---|
| Partner helps "turn off" stress response | Partner is the source of activation |
| Physical contact, emotional support | Hypervigilance, monitoring threat signals |
| Recovery periods at home | Chronic activation without shutdown |
🧷 Pathway 4: Chronic Activation Without Recovery
Toxic stress differs from ordinary stress by the absence of recovery periods (S008). You cannot relax at home because you don't know what mood your partner will be in; you're constantly in hypervigilance mode.
This leads to flattening of cortisol rhythms—your stress system stops "turning off" even at night. The body remains in combat-ready mode 24/7.
Relationships are not just an emotional context. They are a physiological regulator that either buffers stress or amplifies it at the level of hormones and neurotransmitters.
These four pathways often operate simultaneously, creating a synergistic effect. One mechanism amplifies another, and the cumulative impact on cortisol, inflammation, and cognitive function becomes significant.
Cognitive Anatomy of the Myth: Why We Underestimate Our Partner's Impact on Our Health
Despite growing evidence, many people continue to underestimate the impact of relationships on physical health. Why? Let's examine the cognitive biases and cultural narratives that prevent us from seeing this connection. Learn more in the Scientific Method section.
⚠️ Myth 1: "Stress is purely psychological"
Mind-body dualism is deeply rooted in Western culture. We tend to think of stress as a "mental" problem unrelated to physical health.
Stress is an integrated psychophysiological response with measurable biological markers (S001, S005). It's not "just nerves"—it's real changes in brain structure and function, the endocrine system, and the immune system.
Chronic stress is linked to cardiovascular disease, diabetes, obesity, immune disorders, and neurodegenerative diseases. The mechanism works through cortisol, adrenaline, and inflammatory cytokines—this isn't metaphor, it's biochemistry.
🧩 Myth 2: "I control my stress, so my partner can't affect me"
This is an illusion of control. Yes, individual differences in stress resilience exist. But your partner's stress affects your cortisol regardless of your own stress level (S008).
Even if you subjectively feel calm, your physiology may be responding to your partner's stress. The mechanism—emotional contagion and shared environment—operates at a subconscious level, beyond your voluntary control.
- You can't "just not react" to the stress of someone you live with
- Cortisol synchronization occurs through olfactory signals, microexpressions, and tone of voice
- Your nervous system literally "mirrors" your partner's state through mirror neurons
🕳️ Myth 3: "Toxic relationships are only about obvious violence or conflict"
Toxicity is a spectrum, not a binary category. Chronic stress can result not only from arguments, but also from emotional distance, unpredictability, neglect, and microaggressions.
| Type of relationship stress | Visible conflict | Impact on cortisol |
|---|---|---|
| Overt violence, yelling | Yes | Acute spike + chronic elevation |
| Silence, distance, neglect | No | Chronic elevation (often higher) |
| Partner unpredictability | May be hidden | Maximum tension (uncertainty) |
| Microaggressions, criticism | Seems "normal" | Constant low-level elevation |
The most dangerous relationships are those where stress is invisible but constant. The brain cannot adapt to chronic uncertainty; it remains in a state of hypervigilance.
🔍 Why We Don't See It: Three Cognitive Traps
The first trap is normalization. If you grew up in an environment of chronic stress, your nervous system is calibrated to that level as "normal." You don't notice you're living in a state of constant alert.
The second trap is attribution. When you feel fatigue, irritability, insomnia, you attribute it to work, genetics, age—anything except the relationship. Because acknowledging your partner's influence means admitting you don't control your life.
- The third trap is cultural narrative
- Western culture celebrates "independence" and "self-sufficiency." Acknowledging that your partner affects your health means admitting dependence, which is perceived as weakness. So we prefer to believe in the myth of complete control.
The result: people stay in stressful relationships longer than necessary because they don't see the connection between their partner and their physical symptoms. They treat symptoms (insomnia, anxiety, pain) but don't eliminate the source.
🔗 Connection to the Broader System
This cognitive blindness isn't accidental. It's built into a medical system that separates mental and physical health. It's embedded in a culture that romanticizes suffering in relationships as "proof of love."
Understanding the neurobiology of attachment styles helps reveal how childhood experiences program us for certain stress patterns in relationships. But this isn't a life sentence—it's information for action.
