What is faith healing in legal and medical context: defining a phenomenon that kills
Faith healing (spiritual healing, healing by faith) is the practice of treating diseases exclusively or predominantly through religious rituals: prayer, laying on of hands, anointing with oil, casting out demons, appeals to saints or deities. The critical distinction from complementary medicine: faith healing positions itself not as a supplement to conventional treatment, but as its complete replacement, based on the belief that illness results from lack of faith, sin, or demonic influence (S012).
⚠️ Spectrum of practices: from harmless amulets to deadly insulin refusal
Wearing religious symbols, reciting prayers alongside medication, visiting holy sites — these practices may have placebo psychological effects without direct harm. The problem arises when faith healing becomes the exclusive method for conditions requiring urgent medical intervention (S012).
| Condition | Required treatment | Risk if refused |
|---|---|---|
| Infections (pneumonia, meningitis) | Antibiotics | Death within days |
| Type 1 diabetes | Insulin | Diabetic ketoacidosis, death |
| Appendicitis | Surgical intervention | Peritonitis, sepsis, death |
| Early-stage cancer | Surgery, chemotherapy, radiation therapy | Progression, metastasis |
🧾 Legal framework: where religious freedom ends and negligence begins
In most jurisdictions, freedom of religion is not absolute when it concerns the life and health of third parties, especially children. Parents do not have the right to deny children life-saving medical care based on religious beliefs — this is the position of the U.S. Supreme Court, the European Court of Human Rights, and most national judicial systems (S001).
However, some U.S. states have so-called "religious exemptions" — legislative exceptions that shield parents from criminal prosecution for medical neglect if they acted according to religious beliefs (S001).
The paradox: the law simultaneously recognizes a child's right to life and creates a loophole allowing parents to take that life if done in the name of faith.
🔎 Scale of the problem: statistics on preventable deaths
Precise statistics are difficult due to insufficient reporting and the closed nature of religious communities. A study published in 2015 analyzed child deaths in families practicing exclusively faith healing (S004).
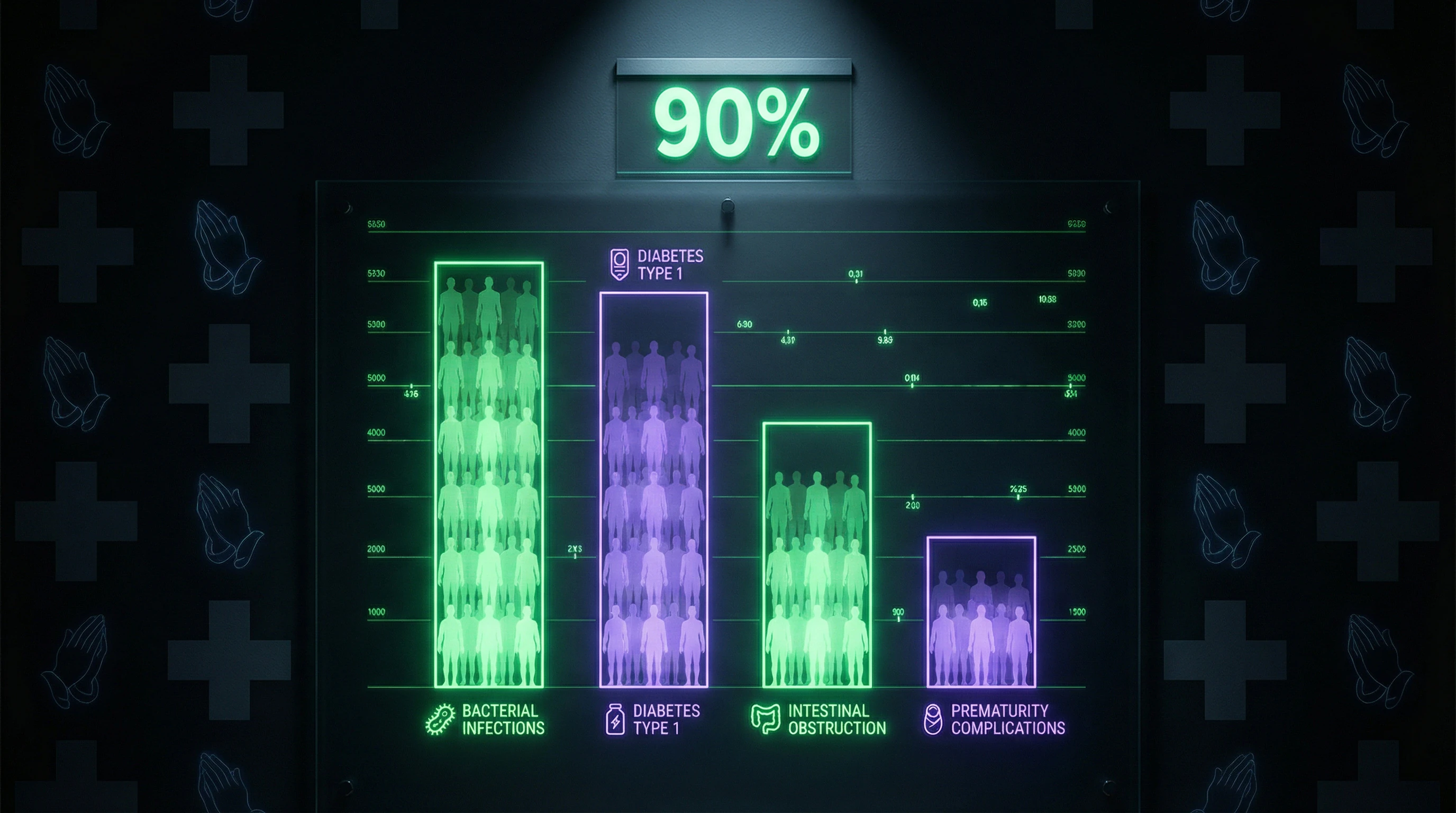
- Key finding
- 90% of documented child mortality cases involved conditions with high survival probability under standard medical treatment: bacterial infections (pneumonia, meningitis), type 1 diabetes, intestinal obstruction, prematurity with complications.
- Why this matters
- Deaths are neither random nor inevitable — they result from active choice to refuse available treatment, not from absence of medical capabilities.
Steel Version of the Argument: Seven Strongest Arguments from Faith Healing Defenders
To honestly analyze the problem, it's necessary to present the most convincing arguments of spiritual healing proponents in their strongest form — not caricatured versions, but logically consistent positions that are actually used in legal proceedings and ethical debates. More details in the section Fasting as a Panacea.
⚠️ First Argument: Constitutional Protection of Religious Freedom as a Fundamental Right
Freedom of religion is not a privilege, but a fundamental human right enshrined in international conventions and constitutions of democratic states. If the government can compel parents to accept medical interventions against their religious beliefs, this creates a dangerous precedent for other forms of state interference in family autonomy and religious practice.
Where is the line drawn? Can the state prohibit circumcision? Refusal of blood transfusions among Jehovah's Witnesses? Vegetarian diets for children in Hindu families?
🧩 Second Argument: Parental Autonomy and the Right to Raise Children According to One's Values
Parents, not the state, bear primary responsibility for their children's well-being and have the right to make decisions about upbringing, education, and medical care in accordance with their deepest convictions. State intervention should be a last resort, applied only in cases of clear and immediate harm.
Many medical decisions contain elements of uncertainty and risk — why should religiously motivated decisions be subject to stricter scrutiny than other parental choices?
⚠️ Third Argument: Documented Cases of Spontaneous Remission and "Miraculous Healings"
Medical literature contains documented cases of spontaneous remission of serious diseases, including late-stage cancer, that cannot be fully explained by modern science. If there exists even a small probability of healing through faith, and if this faith is central to the family's religious identity, shouldn't parents have the right to choose this path?
Absence of scientific explanation does not mean absence of real effect.
🧩 Fourth Argument: Psychoneuroimmunology and Scientific Foundations for the Faith-Health Connection
A growing body of research in psychoneuroimmunology demonstrates real physiological effects of psychological states on the immune system and healing processes. Faith, hope, and spiritual practice can activate endogenous healing mechanisms through stress reduction, improved immune function, and activation of the parasympathetic nervous system.
This is not mysticism, but a recognized field of scientific research.
⚠️ Fifth Argument: Iatrogenic Harm and Risks of Conventional Medicine
Medical errors are the third leading cause of death in the United States. Medication side effects, hospital-acquired infections, surgical complications, misdiagnoses — conventional medicine carries its own significant risks.
Some families make a rational choice to avoid these risks, especially for conditions with uncertain prognosis or aggressive treatments with severe side effects (such as chemotherapy in children).
- Medical errors as the third leading cause of mortality
- Side effects of pharmacotherapy and hospital-acquired infections
- Surgical complications and misdiagnoses
- Aggressive treatments with severe side effects
🧩 Sixth Argument: Cultural Imperialism and Imposing the Western Biomedical Model
Insisting on the exclusivity of scientific medicine reflects cultural imperialism and disregard for non-Western systems of knowledge and healing. Many cultures have millennia-old traditions of spiritual healing that are an integral part of their identity.
Criminalization of faith healing disproportionately affects religious minorities and marginalized communities, reinforcing systemic inequality.
⚠️ Seventh Argument: Slippery Slope to a Totalitarian Medical State
If the state can forcibly treat children against parental wishes in faith healing cases, this opens the door to other forms of compulsory medical intervention: mandatory vaccination without exceptions, forced psychiatric treatment, eugenic programs.
History shows that medical paternalism can be used for horrifying abuses — from forced sterilization to Nazi medical experiments.
Evidence Base for Faith Healing Effectiveness: What Systematic Reviews and Meta-Analyses Show
Scientific data on the effectiveness of spiritual healing requires clear separation: psychological effects (improved well-being, reduced anxiety) and objective clinical outcomes (survival, remission, physiological indicators) are different phenomena. More details in the section Anti-Vaccination Movement.
📊 Intercessory Prayer: What Systematic Reviews Say
Methodologically rigorous studies of intercessory prayer (distant prayer for others) have found no specific therapeutic effect (S012). This does not exclude psychological benefits for the person praying or for patients aware of the prayers (placebo effect), but no direct physiological impact on biological disease processes has been identified.
The absence of evidence for a specific effect of prayer on physiology does not mean absence of psychological benefits of faith.
🧪 Two Cardiac Studies: Results and Limitations
Two American studies in cardiac intensive care units showed statistically significant better outcomes in prayer groups (S012). However, both had serious methodological problems: inability to fully blind, insufficient adjustment for confounders, lack of replication in subsequent large studies.
| Characteristic | Faith Healing Studies | Evidence-Based Medicine Standard |
|---|---|---|
| Sample Size | Often small | Adequate for statistical power |
| Control Groups | Often absent | Mandatory |
| Blinding | Impossible or incomplete | Double-blind |
| Outcomes | Often subjective | Objective, measurable |
| Funding | Often religious organizations | Independent |
🔬 Quality of Evidence Base: Systematic Errors
The overwhelming majority of studies claiming positive effects of faith healing are characterized by weak methodological quality: absence of control groups, retrospective design, subjective outcomes, publication bias (S012). Studies funded by religious organizations report positive results significantly more often than independent ones—a classic sign of conflict of interest.
📊 Cure vs. Healing: Conceptual Distinction
Two terms often confused in faith healing debates. Cure—elimination of pathological process: destroying bacteria, removing tumors, normalizing glucose. Healing—restoration of wholeness, meaning, and well-being: psychological, social, spiritual (S012).
- Faith healing can contribute to healing in the broad sense
- Helps cope with illness, find meaning in suffering, feel community support.
- But this is not equivalent to cure
- Physical elimination of disease requires impact on biological mechanisms of illness, not just psychological state.
🧾 Psychological Benefits: Real, But Not Replacing Medicine
Psychological benefits of faith and spiritual practices are well documented (S012). Religious involvement is associated with lower levels of depression and anxiety, better stress coping mechanisms, stronger social support, greater sense of meaning.
These factors can indirectly influence health through psychoneuroimmunological mechanisms and placebo effect. However, this does not justify refusing effective medical treatment for serious illnesses—psychological well-being and physical recovery require different interventions.
Mechanisms and Causality: Why Correlation Between Faith and Health Doesn't Mean Prayer Cures Cancer
Observed correlations between religiosity and certain health indicators are often interpreted as evidence of faith healing effectiveness. However, correlation does not imply causation, and there are numerous alternative explanations for these associations that don't require assuming supernatural intervention. More details in the Alternative Oncology section.
🧬 Confounders: Social Support, Healthy Lifestyle, and Selection
Religious communities often provide strong social support, which is itself a powerful predictor of health and longevity. Many religious traditions promote healthy lifestyles: abstinence from alcohol and tobacco, dietary moderation, regular social interactions.
There's a selection effect: people with more severe illnesses may be less able to participate in religious practices, creating the illusion that religiosity protects against disease, when in reality health enables religious participation.
Healthy people go to church. That doesn't mean the church healed them—they were simply healthy enough to attend.
🔁 Placebo and Nocebo Effects: Real Physiological Effects of Expectations
The placebo effect is a real physiological phenomenon in which patient expectations can influence biological processes through neuroendocrine and immune mechanisms. Belief in treatment effectiveness (including faith healing) can activate endogenous opioid systems, reduce stress responses, and modulate inflammatory processes (S012).
However, the placebo effect has limitations: it's most effective for subjective symptoms (pain, nausea, fatigue) and significantly weaker for objective pathological processes (infections, tumors, metabolic disorders). Placebo cannot replace insulin for type 1 diabetes or antibiotics for bacterial meningitis.
| Symptom Type | Placebo Susceptibility | Mechanism |
|---|---|---|
| Pain, nausea, fatigue | High (20–40%) | Neuroendocrine modulation |
| Inflammation, immune response | Moderate (10–20%) | Psychoneuroimmune pathways |
| Infection, tumor, metabolism | Minimal (<5%) | Requires specific treatment |
🧠 Psychoneuroimmunology: Real Science, But Not Magic
Psychoneuroimmunology studies interactions between psychological processes, the nervous system, and immune function. Chronic stress suppresses immune function, while positive emotional states and social support can enhance it (S012).
This explains why psychological interventions (including spiritual practices) can have measurable effects on some aspects of health. However, these effects are modest and cannot replace specific medical treatment for serious illnesses. Meditation may improve immune function by 10–20%, but that won't help if you need emergency appendectomy.
- Stress → suppression of T-cells and NK-cells → reduced anti-tumor immunity
- Positive emotions → activation of parasympathetic nervous system → enhancement of regulatory T-cells
- Social support → reduction of cortisol → restoration of immune balance
- Spiritual practices → modulation of inflammation, but NOT elimination of pathogen or tumor
🧷 Regression to the Mean and Natural Disease Course
Many diseases have a fluctuating course with periods of exacerbation and remission. Patients most often turn to faith healing during exacerbations, when symptoms are most severe.
Subsequent improvement may result from natural regression to the mean or spontaneous remission, rather than the effect of spiritual intervention. Without a control group, it's impossible to distinguish treatment effect from natural disease course.
The patient prays during the worst moment of illness. The disease follows its course and improves. Prayer gets credit for what would have happened anyway.
Conflicts in the Evidence Base: Where Sources Diverge and Why It Matters
The scientific literature on faith healing is not monolithic. Significant disagreements exist between researchers, particularly between those working in religious institutions and independent researchers at secular universities. More details in the Mental Bugs section.
🧩 Methodological Divide: Rigorous RCTs vs. Observational Studies
Randomized controlled trials (RCTs) with adequate blinding and control for confounders consistently fail to find specific effects of faith healing on objective clinical outcomes (S001). In contrast, observational studies and studies with weaker designs more frequently report positive associations.
This is a classic pattern: when methodology becomes more rigorous, the effect disappears. Observed associations are driven by methodological artifacts, not actual therapeutic impact.
🔎 Conflicts of Interest and Funding Sources
Studies funded by religious organizations or conducted at religiously affiliated medical facilities are significantly more likely to report positive faith healing outcomes than studies funded by government scientific agencies (S002).
This doesn't necessarily indicate fraud, but it does point to systematic bias in study design, data interpretation, and publication of results.
- Choice of metrics: religious institutions often use subjective measures (well-being, spiritual growth) rather than objective ones (survival, tumor size).
- Participant selection: exclusion of patients with severe disease forms who might lower success rates.
- Interpretation: identical data are read as "evidence of efficacy" in religious journals and as "absence of effect" in secular ones.
📊 Publication Bias: Vanishing Negative Results
Studies that find no effects of faith healing are less likely to be published in journals, especially in journals focused on integrative or complementary medicine (S004). This creates a distorted picture in the literature.
| Result Type | Publication Probability | Where Published |
|---|---|---|
| Positive (faith healing works) | High | Religious journals, integrative medicine |
| Null (no effect) | Low | Rarely; if published—in niche journals |
| Negative (harm) | Very low | Legal documents, medical expert reports |
The phenomenon known as the "file drawer problem" means that negative results remain in researchers' drawers and never enter scientific circulation. Positive results are overestimated, negative results underestimated.
This bias can be verified through scientific databases by comparing published studies with clinical trial registries (ClinicalTrials.gov). The gap between planned and published studies often reaches 30–50%.
Cognitive Anatomy of Belief in Miraculous Healing: Which Psychological Mechanisms Are Exploited
Understanding why people believe in the effectiveness of faith healing despite evidence requires analysis of cognitive biases and psychological mechanisms that make this belief resistant to refutation. More details in the section Thinking Tools.
⚠️ Confirmation Bias: Seeing Only What Confirms Belief
People notice and remember cases that confirm their beliefs and ignore those that contradict them. If they believe in prayer, they remember recoveries and rationalize deaths as lack of faith or God's will.
This creates a subjective sense of effectiveness that doesn't correspond to objective statistics (S001).
🧠 Illusion of Control and Need for Meaning
Illness generates helplessness and chaos. Faith healing restores control: illness has a spiritual cause, healing is possible through correct actions (prayer, repentance).
A false sense of control is psychologically more comfortable than acknowledging the randomness of biological processes (S002).
⚠️ Survivorship Bias and Selective Memory
We hear stories of miraculous healings from survivors. We don't hear from the dead who relied on faith healing. Religious communities actively spread successes and suppress failures.
This creates systematic distortion of available information (S004).
🧩 Authority and Social Proof
When religious leaders assert the effectiveness of faith healing and the community shares this belief, individual critical thinking is suppressed. Social proof and authority outweigh rational evaluation of evidence (S006).
⚠️ Cognitive Dissonance and Sunk Cost Protection
A person who denied treatment to a child for the sake of faith healing faces unbearable dissonance: "I harmed someone I love." Instead of admitting error, the brain activates defenses: "It was God's will," "Faith was insufficient," "Doctors wouldn't have saved them."
The higher the cost of the decision (death of a loved one), the stronger the psychological defense and the more resistant the belief becomes to refutation (S001).
| Mechanism | How It Works | Result |
|---|---|---|
| Confirmation bias | Remember successes, forget failures | Illusion of effectiveness |
| Illusion of control | Illness = meaning + action, not randomness | Psychological comfort instead of treatment |
| Survivorship bias | Hear only success stories | Systematic data distortion |
| Social proof | Community believes → I believe | Suppression of critical thinking |
| Cognitive dissonance | Death of loved one = defense of belief | Belief becomes irrefutable |
🔗 Social Structure as Amplifier
Faith healing doesn't exist in a vacuum. It's embedded in a social system: religious community, authority of leaders, shared narratives about the meaning of suffering. Each element of the system reinforces the others.
A person doubting faith healing risks social isolation, loss of identity, rupture with family. The psychological cost of defection is often higher than the cost of belief, even if belief leads to death (S003).
⚠️ Why Facts Don't Work
Providing mortality statistics or scientific evidence often strengthens belief rather than weakening it. This is called the "backfire effect": when facts contradict deep conviction, the brain perceives them as a threat and reinforces the original position.
Changing belief requires not more facts, but reframing of meaning, restoration of control through other mechanisms (medicine, psychological support), and safe exit from the social system (S007).
🧩 Mechanism of Exploitation
Religious organizations and faith healers often consciously use these mechanisms. They create narratives that activate the need for meaning and control, use authority and social pressure, hide failures and spread successes.
This isn't always conscious deception—often it's the result of self-deception and group dynamics. But the result is the same: people die because psychological mechanisms that evolved for survival under uncertainty are exploited by a system that causes harm (S002).
