The Myth of Universal Parasitic Infection: Science vs. Fearλ
The popular claim that everyone has parasites is not supported by scientific evidence and is used to sell questionable products.
Overview
The claim "everyone has parasites" is a marketing tool, not a medical fact. In developed countries with quality sanitation, parasite prevalence is in the single-digit percentages 🧬: diagnosis requires laboratory confirmation, not universal "cleanses." The myth is exploited by the wellness industry and alternative medicine, replacing evidence-based diagnosis with fear and self-treatment.
🛡️
Laplace Protocol: Parasitic infections are a real medical problem requiring professional diagnosis. The claim of universal infection is an exaggeration used for commercial purposes and does not correspond to scientific data on parasite prevalence in various populations.
Reference Protocol
Scientific Foundation
Evidence-based framework for critical analysis
Protocol: Evaluation
Test Yourself
Quizzes on this topic coming soon
Fact Checks
View All Claims →Claims & Analysis
⚡
Deep Dive
What Are Parasites and How They Spread in Human Populations
Parasites are organisms that live on the surface or inside a host's body and feed on its resources. Three main groups parasitize humans: helminths (worms), ectoparasites (mites, lice, bedbugs), and protozoa (single-celled organisms).
Each group has specific transmission routes and requires different approaches to diagnosis and treatment. Universal "anti-parasitic programs" ignore this biological reality.
Types of Human Parasites and Their Biological Characteristics
Helminths are multicellular worms with complex life cycles, often requiring multiple hosts. Tapeworms (cestodes) inhabit the intestines and can reach several meters in length. Roundworms (nematodes) include ascarids and pinworms. Flukes (trematodes) affect the liver and other organs.
- Ectoparasites
- Live on the skin. Mites transmit infections through saliva, lice feed on blood and cause pediculosis, bedbugs leave characteristic bites.
- Protozoa
- Microscopic single-celled organisms (giardia, toxoplasma). Cause serious diseases in immunocompromised individuals.
Each parasite species requires specific diagnostics and targeted treatment. This makes universal "anti-parasitic programs" scientifically unfounded.
Transmission Routes and Infection Risk Factors
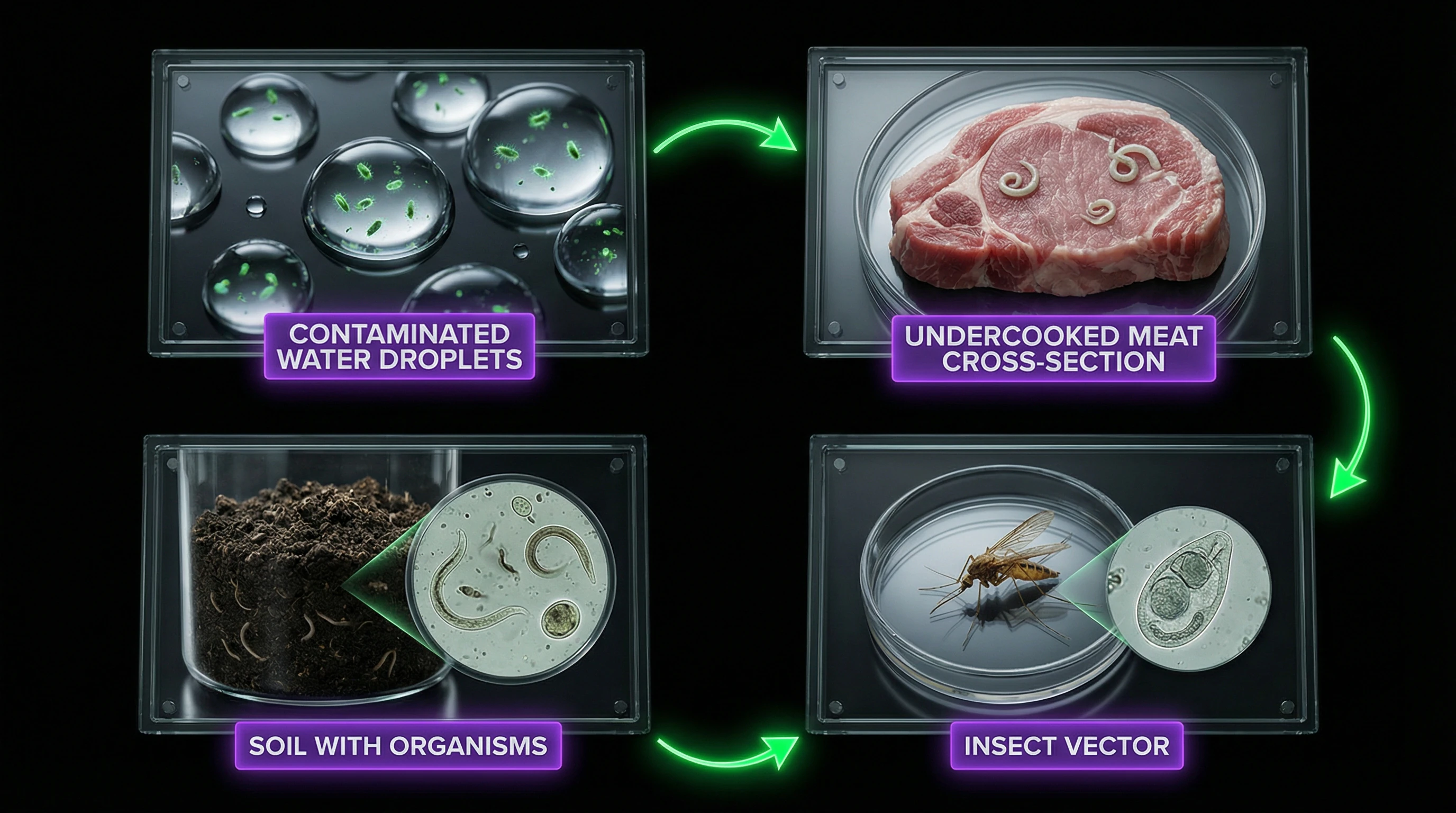
Infection occurs through specific mechanisms, not spontaneously. The fecal-oral route is realized through consumption of contaminated water, unwashed vegetables and fruits—especially in regions with underdeveloped sanitation.
| Transmission Route | Mechanism | Examples |
|---|---|---|
| Vector-borne | Insect and tick bites | Malaria, Lyme disease |
| Contact | Direct contact with infected person or shared objects | Ectoparasites, scabies |
| Foodborne | Raw or undercooked food | Liver fluke, tapeworm |
Risk factors: travel to endemic regions, raw food (especially fish and meat), contact with infected animals, work in agriculture or veterinary medicine, living in poor sanitary conditions.
Documented case: liver fluke infection after consuming unwashed greens led to severe anemia and elevated alkaline phosphatase, requiring prolonged treatment. This illustrates the connection between infection and specific hygiene violations, not its inevitability for all people.
Scientific Data on Parasite Prevalence in the Modern World
Epidemiological studies show that the prevalence of parasitic infections varies significantly depending on geographic region, level of economic development, and sanitary-hygienic conditions. The claim that "everyone has parasites" contradicts scientific evidence.
Actual statistics demonstrate a clear correlation between infrastructure development level and parasite infection rates.
Statistics by Region and Endemic Zones
In developing countries of Africa, Southeast Asia, and Latin America, the prevalence of intestinal helminthiases can reach 50–70% of the population in certain regions, especially in rural areas with limited access to clean water.
Malaria, transmitted by mosquito vectors carrying Plasmodium protozoa, remains endemic to tropical and subtropical zones, where hundreds of millions of cases are registered annually. Schistosomiasis affects more than 200 million people in countries with freshwater bodies infected with intermediate hosts—snails.
- Intestinal helminthiases — 50–70% in endemic regions
- Malaria — hundreds of millions of cases annually in the tropics
- Schistosomiasis — over 200 million people in risk zones
- Tick-borne infections — regional threat in forested areas
In temperate climates and developed countries, the situation is dramatically different: most parasitic infections are imported cases related to international travel. Autochthonous (local) cases are limited primarily to enterobiasis (pinworms) in preschool-age children and ectoparasites (lice, mites).
Differences Between Developed and Developing Countries
The key factor determining parasite prevalence is the quality of water supply and sanitation. In countries with centralized water treatment and modern sewage systems, the frequency of intestinal parasitic infections drops to single-digit percentages of the population.
Access to medical care and regular preventive examinations enable detection and treatment of infections at early stages, preventing mass spread. Educational programs on hygiene and food safety establish behavioral patterns that minimize infection risk.
In developing countries, the absence of basic sanitary infrastructure creates conditions for fecal-oral transmission of parasites. The use of untreated human excrement as fertilizer, consumption of water from open sources, and low levels of hygiene literacy maintain high circulation of pathogens.
Insufficient thermal processing of food, especially fish and meat, leads to infection with tissue helminths. These differences explain why parasitic infections remain a global health problem in some regions but are practically eliminated in others.
Where the Myth of Universal Parasitic Infection Came From
The idea that "everyone has parasites" has no scientific basis, but is actively spread in certain online communities and commercial niches. This narrative emerged at the intersection of alternative medicine, the wellness industry, and conspiracy theories, where simplified explanations of complex medical problems find fertile ground.
The Role of Social Media and the Wellness Industry
Social platforms—Reddit, Facebook, Instagram, Twitter—have become primary channels for spreading misinformation about parasites. Discussions in wellness communities contain anecdotal testimonials without medical confirmation, where users attribute a wide range of nonspecific symptoms to parasites: fatigue, digestive issues, skin rashes.
Social media algorithms amplify the spread of such content, creating "echo chambers" where unverified claims are repeatedly reinforced and perceived as truth.
| Manipulation Mechanism | How It Works | Result |
|---|---|---|
| Pseudoscientific terminology | Use of medical terms without precise meaning | Illusion of authority and competence |
| References to "studies" | Misinterpretation or fabricated sources | Appearance of evidence-based claims |
| Monetization of fear | Selling supplements and detox programs without proven efficacy | Profit from medical illiteracy |
The wellness industry exploits consumer anxiety by promoting "antiparasitic programs" and dietary supplements. The lack of regulation in the supplement sector allows products with unproven efficacy to be marketed under the guise of preventing "universal infection."
Conspiracy Theories and Distrust of Medicine
The myth of universal infection often intertwines with conspiracy narratives, especially in anti-vaccine communities. Posts link vaccines to parasites, claiming without evidence that vaccinations contain parasitic organisms or facilitate their spread.
The psychological mechanism behind the appeal of such theories: simple explanations for complex health problems and a sense of "secret knowledge" unavailable to most. Attributing diverse symptoms to a single cause creates an illusion of control.
However, this approach is dangerous: focusing on a nonexistent problem distracts from real diseases requiring professional diagnosis. This can lead to progression of serious pathologies when symptoms are ignored.
Real Cases of Parasitic Infections: When Diagnosis is Confirmed
Risk Factors and Population Groups with Increased Infection Probability
Parasitic infections are not evenly distributed — infection probability increases sharply under specific conditions. Travel to endemic regions, consumption of contaminated water or inadequately processed food, contact with infected animals, and occupational hazards create real transmission pathways.
In developed countries with quality water treatment and high food safety standards, helminth prevalence is significantly lower. Documented case: liver fluke infection after consuming unwashed greens led to severe anemia and elevated alkaline phosphatase — diagnosis established only after laboratory testing.
| Risk Group | Specific Conditions | Transmission Mechanism |
|---|---|---|
| Preschool children | Insufficient hygiene skills | Contact with contaminated soil, objects |
| Agricultural and veterinary workers | Regular contact with soil and animals | Direct contact with infected material |
| Immunocompromised individuals | Reduced body defense | Increased susceptibility to invasion |
| Ectoparasites (ticks, bedbugs) | Color preferences when choosing shelters | Transmission through saliva, bites |
Even in risk groups, infection is not inevitable — specific transmission conditions are required, unique to each parasite species.
Symptoms Requiring Medical Attention and Laboratory Diagnosis
Genuine parasitic infections manifest with specific symptoms, distinct from the vague complaints of alternative medicine. Persistent gastrointestinal disorders with unexplained weight loss, visible parasites in stool, specific skin manifestations in ectoparasitoses, unexplained anemia and eosinophilia in blood tests — signs requiring professional evaluation.
Many conditions — irritable bowel syndrome, food intolerances, endocrine disorders, psychosomatic conditions — have similar nonspecific symptoms but require entirely different treatment approaches. This is the trap: symptom similarity does not mean cause similarity.
Diagnosis of parasitic infections is based on objective laboratory methods: microscopic stool examination (often requires multiple samples), serological tests for specific antibodies, PCR diagnostics to detect parasite DNA, imaging methods when tissue forms are suspected.
Self-diagnosis based on internet symptoms or "tests" of dubious origin has no medical value. Medical consultation platforms show: patients often present with parasite suspicions for nonspecific symptoms, but confirmed diagnoses are established only after comprehensive examination by a qualified specialist.

The Danger of Self-Diagnosis and Uncontrolled "Antiparasitic Cleanses"
Why Professional Laboratory Diagnosis is Necessary Before Treatment
Antiparasitic medications are specific drugs with clearly defined indications, mechanisms of action, and side effects. Choosing a treatment regimen requires precise identification of the pathogen.
Different types of parasites are sensitive to different medications: treatments for nematodes won't work on cestodes, medications for intestinal forms are ineffective against tissue parasites. Without an accurate diagnosis, treatment becomes meaningless and potentially dangerous consumption of toxic substances.
| Parasite Type | Drug of Choice | Without Diagnosis |
|---|---|---|
| Nematodes (roundworms) | Mebendazole, pyrantel | Ineffective |
| Cestodes (tapeworms) | Niclosamide, praziquantel | Ineffective |
| Tissue parasites | Specific regimens | Dangerous |
Self-diagnosis based on nonspecific symptoms leads to ignoring real diseases. Chronic fatigue can be a sign of anemia, hypothyroidism, depression, or dozens of other conditions.
Digestive disorders may indicate inflammatory bowel disease, celiac disease, dysbiosis, or functional disorders. Focusing on a nonexistent infection distracts from finding the true cause and delays proper treatment—especially dangerous with serious diseases requiring early diagnosis.
Risks of Uncontrolled Use of Antiparasitic Drugs and Supplements
Antiparasitic medications have toxicity: hepatotoxicity, neurotoxicity, hematological disorders, allergic reactions. Uncontrolled use without medical indications exposes the body to unnecessary risks.
"Antiparasitic cleanses" are often based on herbal mixtures and supplements with unproven efficacy. Plant components can interact with medications, cause allergies, and have toxic effects on the liver and kidneys. The lack of quality control for supplements means the composition may not match what's claimed, and concentrations of active substances can be unpredictable.
Marketing of "antiparasitic programs" exploits fears and lack of medical knowledge, offering expensive courses to people who don't need them. Social media and forums are flooded with advertisements for such products with pseudoscientific explanations and fake testimonials.
The real danger is not only financial losses and side effects, but also a false sense of security: a person who has undergone a "cleanse" may ignore serious symptoms, believing they've solved the problem. The medical community does not recommend preventive deworming for populations in developed countries without specific risk factors and confirmed diagnosis.
Evidence-Based Prevention of Parasitic Infections in Daily Life
Hygiene and Food Safety as the Foundation of Infection Prevention
Effective prevention of parasitic infections is based on simple but consistently followed hygienic measures that break the transmission pathways of pathogens. Thorough handwashing with soap after using the toilet, contact with soil, animals, and before food preparation is a basic measure that prevents fecal-oral transmission of parasites.
Consuming only properly filtered or boiled water in regions with questionable water quality, thoroughly washing vegetables, fruits, and greens under running water, and adequate heat treatment of meat and fish (especially freshwater) eliminate most risks of foodborne infection. The case of liver fluke infection from unwashed greens clearly demonstrates the importance of this simple precaution.
| Risk Source | Preventive Measure |
|---|---|
| Household pets | Regular deworming as recommended by veterinarian, hygiene when cleaning litter boxes |
| Soil and vegetation | Gloves when working with soil, thorough handwashing after contact |
| Ticks in endemic regions | Repellents, protective clothing, body inspection after outdoor activities |
| Stray animals | Avoiding contact, maintaining hygiene |
These measures don't require special medications or expensive procedures, but when applied systematically, they provide reliable protection.
When You Actually Need to See a Doctor for Testing
Medical consultation is necessary when specific indications are present, not due to vague concerns or after reading alarming articles on the internet. Seeing a doctor is justified for persistent gastrointestinal symptoms (diarrhea, abdominal pain, nausea) lasting more than two weeks, unexplained weight loss, discovery of unusual material in stool, or appearance of specific skin manifestations after bites or contact with potential carriers.
Anemia of unknown origin, eosinophilia in complete blood count, fever after returning from tropical countries — these are signals for comprehensive examination including parasitological tests, not a reason for self-treatment.
Preventive parasite screening is recommended for at-risk groups: children attending childcare facilities, food industry and food service workers (per sanitary requirements), people who have returned from endemic regions with symptoms, and individuals with occupational risks.
For the rest of the population in developed countries, routine parasite screening is not part of standard medical care due to low infection prevalence and lack of economic justification. The correct approach is seeing a doctor when specific symptoms appear, undergoing prescribed tests, and following specialist recommendations, rather than self-prescribing "preventive" medication courses based on questionable internet information.

Knowledge Access Protocol
FAQ
Frequently Asked Questions
No, this is a scientifically unfounded claim. The prevalence of parasitic infections depends on region of residence, hygiene conditions, and lifestyle—in developed countries, infection rates are significantly lower due to quality water and sanitation. Universal infection is a myth actively spread in wellness communities to sell dubious 'cleanses.'
Humans can be affected by three main groups of parasites: helminths (worms—roundworms, pinworms, tapeworms), protozoa (giardia, toxoplasma), and ectoparasites (ticks, lice, bedbugs). Each type has specific transmission routes and requires different diagnostic and treatment methods.
Main transmission routes include consuming contaminated water and poorly processed food, contact with infected animals, and poor hand hygiene. Risk factors include travel to endemic regions, consuming raw meat or fish, and working with soil without gloves.
The myth is actively spread through social media, wellness bloggers, and supplement sellers who use fear to promote 'antiparasitic programs.' On Reddit and Facebook, this claim is even linked to conspiracy theories about vaccines, though there is no scientific confirmation.
In developing countries with poor sanitation, infection rates can reach 30-50%; in developed countries—less than 5% of the population. The WHO notes that most cases are concentrated in regions with limited access to clean water and medical care.
Warning signs include: persistent digestive disorders, unexplained weight loss, anal itching, visible parasites in stool, prolonged weakness after tropical travel. It's important to understand that these symptoms are nonspecific and may indicate many other conditions—laboratory diagnosis is necessary.
No, self-diagnosis is impossible and dangerous. Detecting parasites requires specific tests: stool examination, blood tests for antibodies, sometimes endoscopy or ultrasound. Attributing fatigue or bloating to parasites without examination can lead to missing serious diseases.
Uncontrolled medication intake is toxic to the liver and kidneys, can cause allergic reactions, and disrupt intestinal microflora. Without a confirmed diagnosis, you're treating a nonexistent problem while ignoring the real cause of symptoms. Antiparasitic drugs are serious medications requiring prescription and medical supervision.
In developed countries, preventive intake is not recommended in the absence of risk factors. The WHO advises mass deworming only in endemic regions with high infection rates. For residents of the US and Europe, proper hygiene and thermal food processing are sufficient.
Standard set: three-time stool analysis for helminth eggs, pinworm scraping, blood test for antibodies to major parasites (giardia, toxocara, opisthorchis). The specific list is determined by an infectious disease specialist or parasitologist based on symptoms and medical history.
Absolutely not — this is a conspiracy theory with no scientific basis. Vaccines undergo rigorous quality control and contain only antigens or weakened viruses/bacteria, never parasites. Such claims are spread in anti-vaccine communities to manipulate public opinion.
Parasitic infections can cause weakness, but this is a rare cause of chronic fatigue in developed countries. Fatigue is more commonly linked to vitamin deficiencies, anemia, endocrine disorders, depression, or sleep deprivation. Attributing all symptoms to parasites is a typical error of pseudomedical practices.
The foundation of prevention is thorough handwashing, consuming boiled or filtered water, and cooking meat and fish until fully done. It's important to wash fruits and vegetables, avoid swimming in contaminated water bodies, and regularly deworm household pets.
Seek medical attention for persistent gastrointestinal issues lasting more than 2 weeks, unexplained weight loss, diarrhea after traveling to tropical countries, or if you discover worms in stool. Consultation is also needed after contact with infected individuals or if you work in high-risk groups (veterinarians, wastewater treatment workers).
Yes, certain parasites are transmitted from animals: toxocariasis from dogs, toxoplasmosis from cats, echinococcosis from dogs and wild animals. Prevention includes regular deworming of pets (every 3-6 months), handwashing after contact, and cleaning up feces while wearing gloves.
Scientific evidence for the effectiveness of pumpkin seeds, garlic, or wormwood against parasites is insufficient. These remedies may have mild supportive effects but do not replace specific antiparasitic medications for confirmed infections. Relying solely on folk methods for actual infections is dangerous.
