Intestinal Parasites: Impact on Microbiome and Gut Healthλ
Evidence-based approach to understanding the connection between parasitic infections, microbiota composition, and functional digestive health
Overview
Intestinal parasites alter microbiota composition — 🧬 this is not a myth, but a measurable effect with consequences for immunity, nutrient absorption, and intestinal barrier function. Mechanism: competition for resources, toxins, mucosal inflammation. Risk group — immunosuppression (chemotherapy, HIV, transplantation), but most "parasite panics" on social media are built on substituting correlation for causation and ignoring base rates.
🛡️
Laplace Protocol: Diagnosis of parasitic infections requires laboratory confirmation. Self-diagnosis based on symptoms and preventive "cleanses" without medical indications are not recommended. Treatment should only be prescribed after diagnosis confirmation by a qualified specialist.
Reference Protocol
Scientific Foundation
Evidence-based framework for critical analysis
Navigation Matrix
Subsections
[candida-leaky-gut]
Candida and Leaky Gut
We examine the connection between fungal microflora and intestinal barrier dysfunction based on scientific evidence and clinical research
Explore
[everyone-has-parasites]
Everyone Has Parasites
The popular claim that everyone has parasites is not supported by scientific evidence and is used to sell questionable products.
Explore
Protocol: Evaluation
Test Yourself
Quizzes on this topic coming soon
⚡
Deep Dive
Types of Intestinal Parasites and Infection Mechanisms: What Lives in the Gut
Intestinal parasites are a heterogeneous group of organisms that colonize the gastrointestinal tract and feed at the host's expense. Two main categories are distinguished: helminths (multicellular worms) and protozoa (single-celled organisms), each with unique interaction mechanisms.
Understanding the biology of these parasites is critical for developing effective diagnostic and therapeutic approaches.
Helminths and Protozoa: Biological Classification
Helminths include three main classes: nematodes (roundworms), cestodes (tapeworms), and trematodes (flukes). Each class possesses specific morphological characteristics and life cycles.
Soil-transmitted helminths (STH) are widely distributed in African populations and demonstrate measurable correlations with gut microbiome composition. Protozoan parasites—giardia, amoebae—are characterized by shorter life cycles and the ability to rapidly reproduce in the intestinal environment.
- Helminth Impact Mechanism
- Mechanical damage to the mucous membrane and competition for nutrients.
- Protozoan Impact Mechanism
- Disruption of absorption processes and provocation of local inflammation.
- Size Paradox
- Microscopic protozoa can cause more pronounced symptoms than large helminths.
Chronic infection leads to the production of toxins and metabolites that systemically affect the host's immune and nervous systems.
Transmission Routes and Infection Risk Factors
Main transmission routes: fecal-oral mechanism through contaminated water and food, direct contact with infected soil, transmission through intermediate hosts.
| Risk Factor | Impact on Transmission |
|---|---|
| Geographic and Sanitary Conditions | Regions with inadequate water treatment and low hygiene levels demonstrate significantly higher disease incidence |
| Immune Status | Immunocompromised patients show increased susceptibility due to weakened defense mechanisms |
| Parasite Type | Soil-transmitted helminths require contact with contaminated soil; protozoa are transmitted through unboiled water |
| Seasonality | Infection peaks during periods of increased humidity and temperature |
| Occupational Activity | Agricultural or soil work substantially increases the likelihood of helminth infection |
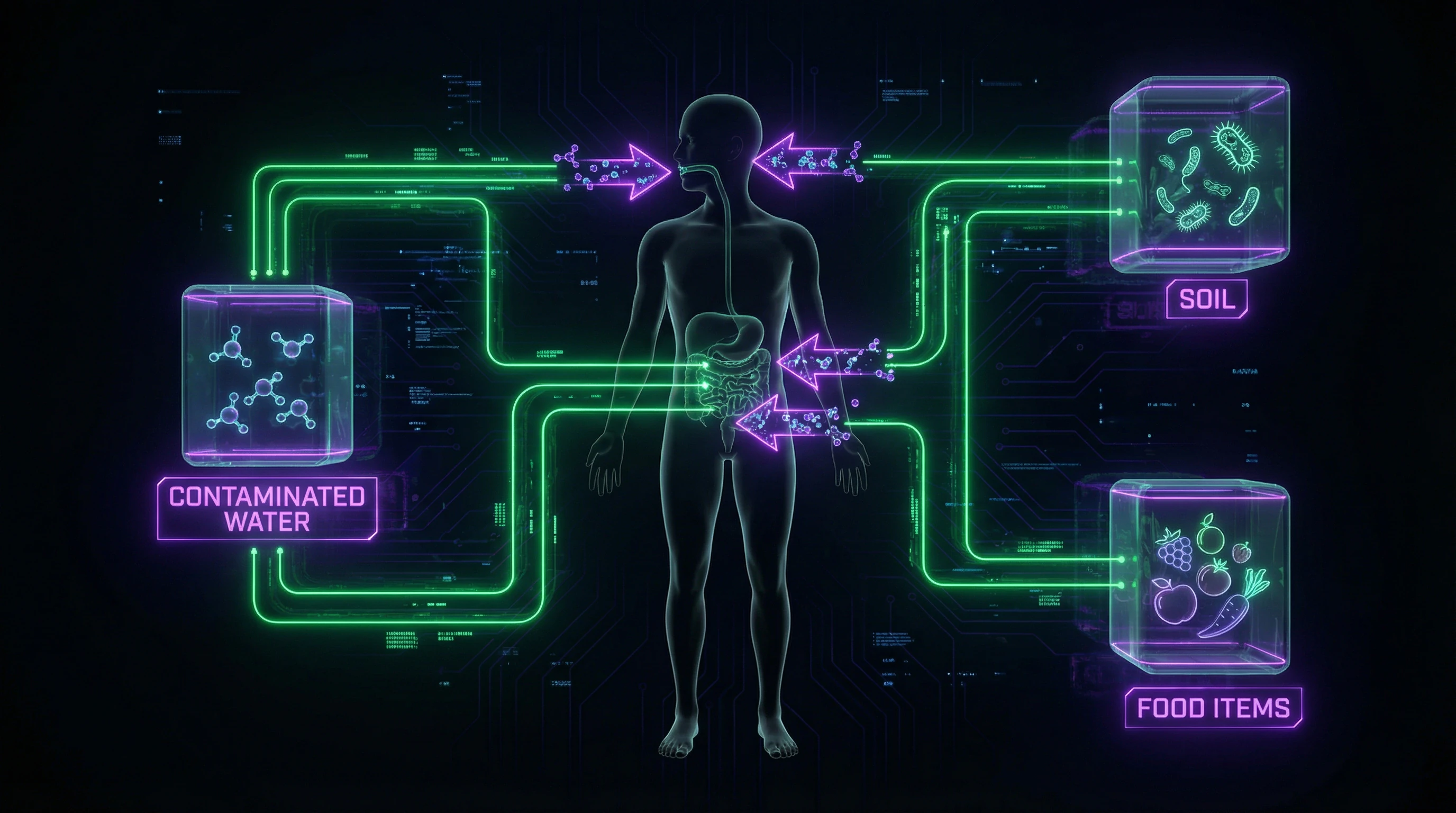
Parasite Interactions with the Gut Microbiome: Ecosystem Alteration
The presence of intestinal parasites initiates a cascade of changes in the composition and functional activity of the gut microbiome — a complex community of microorganisms playing a key role in digestion, immunity, and organismal homeostasis. Modern metagenomic studies have identified measurable correlations between parasitic infections and microbiota diversity.
These interactions are bidirectional: parasites modify the microbial environment, while the microbiome influences parasite survival and virulence.
Impact on Microbiota Diversity
Parasitic infections demonstrate statistically significant associations with changes in alpha- and beta-diversity of the gut microbiome, as confirmed by metagenomic data analysis from African populations. Soil-transmitted helminths correlate with increased overall microbial diversity, which may reflect an adaptive immune response or direct influence of parasitic metabolites on microbial ecology.
Correlation does not imply causation. Multiple factors — diet, geography, sanitation — influence the observed patterns of microbial diversity.
Reduced microbiota diversity is associated with certain types of parasitic infections, especially in chronic protozoan infestations, which can lead to dysbiosis and impaired intestinal barrier function.
- Competition for nutritional substrates between parasite and microbiota
- Production of antimicrobial substances by parasites
- Modulation of local immune response affecting microbial composition
Recovery of microbial diversity after parasite elimination occurs gradually and may require additional probiotic interventions.
Changes in Bacterial Composition During Infection
Specific taxonomic shifts in microbiome composition are observed in various parasitic infections: increased representation of pro-inflammatory bacteria from the Enterobacteriaceae family and decreased abundance of beneficial commensals such as Faecalibacterium prausnitzii.
In immunocompromised patients, distinct patterns of microbiota changes have been identified that differ from those in immunocompetent individuals, indicating the role of immune status in shaping microbe-parasite interactions. These changes may exacerbate clinical manifestations and affect treatment efficacy.
| Functional Impairment | Mechanism | Clinical Significance |
|---|---|---|
| Reduced short-chain fatty acids | Loss of butyrate-producing bacteria | Weakened intestinal barrier, inflammation |
| Disrupted bile acid metabolism | Altered microbial composition | Dysregulation of lipid metabolism |
| Decreased synthesis of vitamins B and K | Elimination of synthesizing strains | Micronutrient deficiency, impaired coagulation |
Parasites can selectively suppress the growth of certain bacterial strains through secretion of specific molecules or alteration of intestinal pH. Restoration of normal bacterial composition after antiparasitic therapy does not always occur spontaneously and may require targeted microbiome modulation.
Clinical Manifestations and Symptoms: From Local to Systemic Effects
Parasitic infections present a spectrum from asymptomatic carriage to severe systemic disorders. Symptoms are often nonspecific and mimic gastroenterological, immunological, or psychiatric conditions, complicating diagnosis.
Symptoms alone are insufficient to confirm infection—laboratory verification is necessary.
Systemic Effects of Parasitic Infections
Chronic inflammation induced by parasites is a key mechanism of systemic manifestations: chronic fatigue, anemia, dermatological problems. Parasitic toxins and metabolites penetrate through the damaged intestinal wall into systemic circulation, affecting distant organs and systems.
The link between parasitic infections and depression is mentioned in popular sources, but a direct causal relationship has not been established. Depression is a multifactorial disorder; chronic infection may be only one of many contributing factors.
Allergic reactions and skin manifestations arise from immune hyperreactivity to parasitic antigens, but parasites are not the sole cause of dermatological conditions. Anemia develops due to blood loss from hematophagous invasion or impaired absorption of iron and vitamin B12.
Immunomodulatory effects of parasites can both suppress and excessively activate the immune system, leading to autoimmune phenomena or increased susceptibility to secondary infections.
Digestive and Immune Disorders
Malabsorption of nutrients is a direct consequence of intestinal epithelial damage and parasite competition for nutrients. Deficiencies of vitamins, minerals, and proteins develop.
- Impairment of intestinal barrier function facilitates translocation of bacterial components and parasitic antigens into systemic circulation, though clinical significance remains subject to scientific debate.
- Dyspeptic symptoms—diarrhea, constipation, bloating, abdominal pain—arise from mechanical irritation, inflammation, and disrupted intestinal motility.
- Immune dysregulation manifests as a shift toward Th2 response with increased IgE production and eosinophilia, exacerbating allergic conditions.
Chronic stimulation of the immune system by parasitic antigens leads to depletion of immune reserves and paradoxical reduction in anti-infectious defense.
Diagnosis requires comprehensive laboratory examination: stool microscopy, serological tests, molecular genetic methods for accurate pathogen identification.
Diagnosing Parasitic Infections: From Symptoms to Laboratory Confirmation
Laboratory Testing Methods
Microscopic stool examination is the gold standard for diagnosing intestinal parasites. Three samples collected at 3–5 day intervals are required for 85–90% sensitivity.
The Kato-Katz concentration method quantitatively assesses helminth infection intensity—critical for treatment selection and epidemiological monitoring.
| Method | Specificity | What It Detects | Limitation |
|---|---|---|---|
| Stool microscopy | 85–90% | Eggs, larvae, trophozoites | Requires repeat samples |
| PCR | 95–99% | Species identification, cryptosporidia, microsporidia | More expensive, not universally available |
| ELISA (serology) | Variable | IgM/IgG antibodies | Cannot distinguish active from past infection |
| Coprology | — | pH, undigested fibers, fatty acids | Supplementary method |
Serological tests (ELISA) detect specific antibodies to parasitic antigens, but a positive result may indicate either active or past infection—requires clinical interpretation.
Molecular genetic methods (PCR) provide high specificity and identify parasites at the species level, including cryptosporidia and microsporidia, which are difficult to detect microscopically.
Peripheral blood eosinophilia (>5% or >500 cells/μL) is an indirect marker of helminth infections, especially during the migratory phase, but is nonspecific and requires differential diagnosis with allergic conditions.
Differential Diagnosis
Symptoms of parasitic infections are often nonspecific and overlap with inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), and celiac disease.
Chronic diarrhea with blood may indicate either amebiasis or ulcerative colitis. Endoscopic examination with biopsy reveals characteristic ulcers and Entamoeba histolytica trophozoites in tissues.
Eosinophilic gastroenteritis caused by tissue helminths is distinguished from allergic reactions to food and medications through elimination diets and provocation tests.
In immunocompromised patients (cancer patients, HIV-infected individuals), parasitic infections present atypically and often coexist with opportunistic infections.
Cryptosporidiosis and isosporiasis in HIV manifest as profuse diarrhea mimicking cholera. Special staining methods (Ziehl-Neelsen) are required to detect oocysts.
Laboratory inflammatory markers (CRP, fecal calprotectin) are elevated in both parasitic infections and IBD. Values >250 μg/g are more characteristic of Crohn's disease and ulcerative colitis.
Evidence-Based Approaches to Treating Parasitic Infections
Antiparasitic Therapy
The choice of anthelmintic medication depends on the parasite species, infection intensity, and patient condition. Self-treatment without laboratory confirmation is unacceptable: risk of toxic effects and development of resistance.
| Medication | Spectrum of Action | Dosage | Mechanism |
|---|---|---|---|
| Albendazole | Nematodes, some cestodes | 400 mg single dose or 3 days | Inhibition of tubulin polymerization |
| Praziquantel | Trematodes, cestodes | 10–25 mg/kg (species-dependent) | High efficacy (85–95%), low toxicity |
| Metronidazole | Amebiasis, giardiasis | 750 mg × 3 times, 7–10 days | Specific therapy for protozoal infections |
| Nitazoxanide | Cryptosporidiosis | Per protocol (immunocompetent patients) | Alternative for resistance cases |
Efficacy monitoring is conducted at 2–4 weeks with repeat parasitological stool examination. Parasite persistence indicates resistance or reinfection.
In oncology patients, dosages require adjustment: myelosuppression and hepatotoxicity from chemotherapy alter the pharmacokinetics of antiparasitic agents.
Microbiome Restoration After Treatment
Antiparasitic therapy, especially metronidazole and broad-spectrum antibiotics, causes dysbiosis: reduced microbiota diversity and decreased populations of short-chain fatty acid-producing bacteria.
The restoration protocol includes three components:
- Probiotics (4–8 weeks post-treatment): Lactobacillus rhamnosus GG, Saccharomyces boulardii, Bifidobacterium longum — reduce the frequency of post-infectious IBS.
- Prebiotics (5–10 g/day): inulin, fructooligosaccharides stimulate growth of beneficial native microflora.
- Dietary correction: fermented foods (kefir, sauerkraut), dietary fiber (25–30 g/day) support restoration and intestinal barrier function.
Metagenomic analysis shows: complete restoration of microbial diversity takes 3–6 months. Some patients retain long-term alterations in microbiota composition.
Monitoring functional indicators (stool frequency, abdominal symptoms) and repeat microbiome analysis when necessary allow assessment of restoration therapy efficacy.
Prevention of Parasitic Infections and Risk Management
Sanitary Practices and Food Safety
Handwashing with soap after using the toilet, contact with soil, and before eating reduces the risk of fecal-oral transmission by 40–50%. This is the most effective and accessible preventive measure.
Thermal processing of meat to 145°F for pork and 160°F for beef destroys Trichinella larvae and cysticerci. Raw vegetables and fruits are washed under running water, especially when organic fertilizers are used.
Drinking water quality is critical: boiling for 1 minute or filtration through pores <1 μm removes Giardia cysts and Cryptosporidium oocysts.
In endemic regions, avoid swimming in freshwater bodies (schistosomiasis prevention) and wear shoes on soil (protection against hookworm and strongyloidiasis). Deworming pets every 3–6 months minimizes the risk of zoonotic parasitoses.
High-Risk Groups
Immunocompromised patients—with cancer, HIV infection, or on immunosuppressive therapy—have an increased risk of severe parasitic infections. Among cancer patients, the prevalence of intestinal parasitic infections reaches 15–30% depending on the region, with infections presenting atypically and diagnosed with delay.
| Risk Group | Primary Risk | Preventive Measure |
|---|---|---|
| Preschool children in group settings | Pinworms, Giardia (close contacts) | Regular preventive screenings |
| Travelers to endemic regions | Multiple parasitoses | Strict food safety, screening after return |
| Agricultural workers, veterinarians | Soil-transmitted parasites | Annual screening, personal protective equipment |
| Pregnant women | Treatment limitations | Prevention planning considering trimester |
Some anthelmintic drugs are contraindicated in the first trimester of pregnancy, so prevention and treatment are coordinated with an obstetrician considering potential risks to the fetus.

Knowledge Access Protocol
FAQ
Frequently Asked Questions
Intestinal parasites are divided into two main groups: helminths (worms) and protozoa (single-celled organisms). Helminths include roundworms, pinworms, tapeworms, and flukes, while protozoa include giardia and amoebas. According to research, these parasites affect the composition of the gut microbiome in different ways (S1).
Parasites significantly alter the diversity and composition of the intestinal microbiota. Studies show a correlation between the presence of helminths and changes in the bacterial composition of the gut (S1). These changes can affect digestion, immunity, and overall health.
Typical symptoms include chronic fatigue, digestive disturbances, anemia, and skin problems. Allergic reactions, reduced immunity, and nutrient deficiencies due to impaired absorption may also occur. It's important to understand that these symptoms are nonspecific and require laboratory confirmation of diagnosis.
No, parasites are not a direct cause of depression. Chronic parasitic infection can contribute to inflammation and affect mood, but depression is a multifactorial condition. Claims about parasites as the primary cause of mental disorders are not supported by scientific evidence.
No, preventive treatment without diagnosis is not recommended in regions with low parasite prevalence. Antiparasitic medications have side effects and should only be prescribed for confirmed infections. Regular cleanses without medical indication can disrupt microbiome balance and harm health.
The primary method is stool analysis for helminth eggs and protozoan cysts, often requiring three separate tests. Additional tests may include blood tests for antibodies, pinworm tape test, and serological tests. The choice of methods depends on clinical presentation and suspected parasite type (S1, S2).
Treatment should be conducted under medical supervision using specific antiparasitic medications. Drug choice depends on parasite type: albendazole or mebendazole for helminths, metronidazole for protozoa. After treatment, it's important to restore the microbiome with probiotics and proper nutrition.
The greatest risk is among people with weakened immunity, including cancer patients, children, and the elderly. Also at risk are those who travel to endemic regions or work with soil or animals. Studies show increased susceptibility in patients with immunosuppression (S2).
Yes, some parasites are transmitted from animals to humans (zoonoses). Toxocariasis from dogs and cats, and echinococcosis from dogs are examples of such infections. Regular deworming of pets, maintaining hygiene after contact with animals, and handwashing reduce infection risk.
After antiparasitic therapy, a course of probiotics with lacto- and bifidobacteria is recommended. It's important to include fermented foods, fiber, and prebiotics in the diet to nourish beneficial microflora. Recovery can take from several weeks to months depending on the degree of disruption (S1).
No, this is a myth. Parasites can contribute to skin manifestations through chronic inflammation and allergic reactions, but they are not the sole cause of dermatological diseases. Most skin problems have other causes: genetics, allergies, autoimmune processes, or infections.
Key measures include thorough handwashing, thermal processing of meat and fish, and washing vegetables and fruits. It's important to drink only purified water, especially when traveling, and to follow sanitary standards. These simple practices significantly reduce the risk of parasitic infection.
Yes, parasites compete for nutrients and can disrupt intestinal absorption. This leads to deficiencies in iron, vitamin B12, folic acid, and other nutrients. Chronic parasitic infection is often accompanied by anemia and vitamin deficiencies requiring correction.
Some parasites increase the risk of certain types of cancer with prolonged infection. For example, opisthorchiasis is linked to cholangiocarcinoma, and schistosomiasis to bladder cancer. Cancer patients are also more vulnerable to parasitic infections due to weakened immunity (S2).
In regions with inadequate water treatment, this is possible, especially for protozoa (Giardia, Cryptosporidium). In U.S. cities with modern water treatment systems, the risk is minimal, but it persists in rural areas. When water quality is uncertain, boiling or using filters is recommended.
Parasites modulate the immune response, often suppressing it for their own survival. This can lead to chronic inflammation, altered Th1/Th2 immune balance, and increased susceptibility to other infections. Research shows complex interactions between parasites, the microbiome, and the immune system (S1, S2).
