What is cervical spine manipulation and why has it become widespread practice without medical oversight
Chiropractic cervical spine manipulation is a high-velocity, low-amplitude mechanical force applied to the cervical vertebrae, often accompanied by a characteristic crack. The procedure is common worldwide (S003), but remains controversial: evidence of its effectiveness is weak, and potential risks are underestimated.
Manipulation is used by chiropractors, osteopaths, physical therapists, and physicians, but chiropractors have made it their signature practice (S003). The problem is that in most countries, a patient can see a chiropractor directly, without medical examination that would identify contraindications.
A person with neck pain bypasses a physician and undergoes manipulation, unaware of their risk factors for arterial dissection.
🧩 Institutional status: license without accountability
In the US, Canada, Australia, and several European countries, chiropractors are licensed and authorized to see patients independently. This creates a paradox: a procedure capable of causing stroke is performed without mandatory medical screening. More details in the section Anti-vaccination Movement.
Most patients undergo only verbal questioning before manipulation. There is no universal international standard requiring neck vessel imaging or functional tests. A patient with undiagnosed vascular anomaly, connective tissue disorder, or other risk factors undergoes the procedure unaware of the danger.
| Type of procedure | Pre-screening | Informed consent |
|---|---|---|
| Chiropractic neck manipulation | Minimal questioning | Often without risk description |
| Invasive medical procedure | Mandatory examination | Detailed risk description |
⚠️ Scale without control
Precise global data is unavailable, but tens of millions of manipulations are performed annually in developed countries. In the US, approximately 10% of adults see chiropractors at least once a year, and a significant portion of these visits include neck manipulation.
- Paradox of rarity
- Even if complications occur in 1 out of 100,000 procedures, with 10 million manipulations annually, this means hundreds of catastrophes per year. A rare event becomes a mass phenomenon.
The absence of mandatory screening and standardized protocol means that people at high risk for arterial dissection undergo manipulations unaware of the danger. This creates conditions for preventable catastrophes.
Review the analysis of how to recognize dangerous medical recommendations to understand the mechanisms that allow risky practices to remain popular.
Five Arguments Used by Proponents of Chiropractic Neck Manipulation — Steelman Analysis of the Position
Before examining the risks, it's necessary to honestly present the strongest arguments of chiropractic proponents. This is not a straw man, but a steelman — the most convincing version of the opposing position. More details in the section Candida and Leaky Gut.
🧩 Argument One: The Vast Majority of Manipulations Occur Without Complications
Chiropractic proponents correctly point out that millions of neck manipulations are performed annually, and the overwhelming majority of patients experience no serious complications. If the procedure were truly dangerous, the number of incidents would be orders of magnitude higher.
Statistically, the probability of a serious complication is estimated in the range of 1 in 100,000 to 1 in 2,000,000 manipulations, which is comparable to the risks of many routine medical procedures.
🧩 Argument Two: Correlation Does Not Imply Causation
Many cases of vertebral artery dissection following chiropractic manipulation may be coincidental. Patients often seek chiropractic care precisely because of neck pain, which itself may be an early symptom of spontaneous arterial dissection.
The manipulation may occur against the backdrop of an already initiated but not yet diagnosed dissection, creating a false causal relationship.
🧩 Argument Three: Spontaneous Arterial Dissections Occur Without Manipulation
Dissection of vertebral and carotid arteries can occur spontaneously or after minimal everyday activities — sudden head turning, sneezing, yoga practice, visiting a hair salon. If an artery can dissect from such trivial actions, singling out chiropractic manipulation as a special risk factor may be unwarranted.
🧩 Argument Four: Absence of Quality Prospective Studies
Most data on the connection between manipulation and arterial dissection is based on case reports and retrospective reviews (S001). Prospective randomized controlled trials that could establish causation with a high degree of certainty are virtually nonexistent.
- Case reports — low level of evidence
- Retrospective reviews — subject to selection bias
- Prospective RCTs — require ethical approvals and funding
- Methodological uncertainty — complicates assessment of true risk
🧩 Argument Five: Subjective Benefit and Patient Satisfaction
Many patients report significant pain relief and improved quality of life after chiropractic manipulation. Even if the mechanism of action is not fully understood, the subjective experience of millions of people cannot be ignored.
For many patients with chronic neck pain, chiropractic care remains one of the few accessible methods that provide relief. This creates a powerful incentive to continue the practice, despite rare but catastrophic complications.
Documented Cases of Catastrophic Complications: From Arterial Dissection to Patient Death
Medical literature contains numerous detailed cases of severe complications following chiropractic neck manipulations. These cases are important not as anecdotal evidence, but as sources for understanding injury mechanisms and risk factors. More details in the section Fake Diagnostics.
📊 Case of a 32-Year-Old Woman: From Routine Manipulation to Massive Brain Infarction
A 32-year-old woman consulted a chiropractor for neck pain. Immediately after manipulation, her condition deteriorated sharply. MRI revealed extensive areas of restricted diffusion in bilateral cerebellar hemispheres, right medulla oblongata, pons, midbrain, thalami, and left occipital lobe—acute infarction in the posterior circulation territory (S003).
The next day, CT showed increased intracranial pressure, hydrocephalus, diffuse cerebral edema, hemorrhagic transformation of the occipital lobe, and cerebellar tonsillar herniation (S003). Endovascular intervention failed—the left posterior cerebral artery territory completed infarction.
Catastrophe develops within hours. Mechanical arterial damage triggers a cascade that cannot be stopped by standard resuscitation methods.
🧾 Vertebral Artery Dissection: Early Stage of Injury
A 40-year-old woman presented with worsening right-sided neck pain and headache 10 days after chiropractic manipulation. Imaging revealed an intimal flap in the terminal portion of the right vertebral artery immediately after dural penetration, causing luminal narrowing (S004).
The artery remained patent, with no infarction on diffusion-weighted imaging. This case demonstrates an early stage of injury when catastrophic outcome can still be prevented.
🧾 Internal Carotid Artery Dissection with Horner's Syndrome
Internal carotid artery dissection following neck manipulation presented with Horner's syndrome (S007). The diameter of the right internal carotid artery increased due to methemoglobin in the vessel wall.
The residual patent true lumen of the artery is visible up to the skull base—the so-called "string sign." Contrast angiography (CT, catheter, or MR angiography) detects such injuries more sensitively than noninvasive time-of-flight angiography (S007).
| Type of Injury | Clinical Sign | Time Interval |
|---|---|---|
| Intimal flap | Neck pain, headache | Hours–days |
| Luminal narrowing | Neurological symptoms | Days–weeks |
| Complete occlusion | Stroke, death | Minutes–hours |
🔬 Posterior Circulation Stroke After Steroid Injection into C1-C2 Facet Joint
Although not a chiropractic manipulation, posterior circulation stroke following steroid injection into the intra-articular C1-C2 facet joint reveals the mechanism of vascular injury in the cervical region (S006). Cervical pain is increasingly treated with invasive procedures, most patients experience temporary improvement, but catastrophic complications can occur—stroke and spinal cord infarction.
Diffusion-weighted MRI showed multiple hyperintensities in the thalami, pons, occipital lobes, hippocampi, splenium of the corpus callosum, and cerebellum (S006). This is the first reported case of posterior circulation stroke associated with intra-articular steroid injection into a cervical facet joint.
🧪 Microvascular Embolization as Mechanism
The pattern of tissue damage on serial MRI and postmortem microscopy indicates microvascular embolization of macromolecular particles as the cause of stroke (S006). Multiple infarct foci in different vascular territories—a sign that damage is not localized but spreads throughout the brain's circulatory system.
- Intimal Flap
- Detachment of the artery's inner layer, creating turbulent flow and a zone of thrombus formation.
- Microembolism
- Particles of thrombus or tissue circulating in the bloodstream and occluding small vessels in the brain.
- Hemorrhagic Transformation
- Bleeding into the infarct zone, occurring when blood flow is restored to damaged tissue.
The connection between neck manipulation and posterior circulation stroke is documented in analysis of the thromboembolic stroke mechanism, which is often ignored by both sides of the debate.
Biomechanics of Catastrophe: How Rotational Movement Tears the Inner Lining of the Artery
Understanding the mechanism of injury is critically important for risk assessment and development of safety protocols. More details in the section Cognitive Biases.
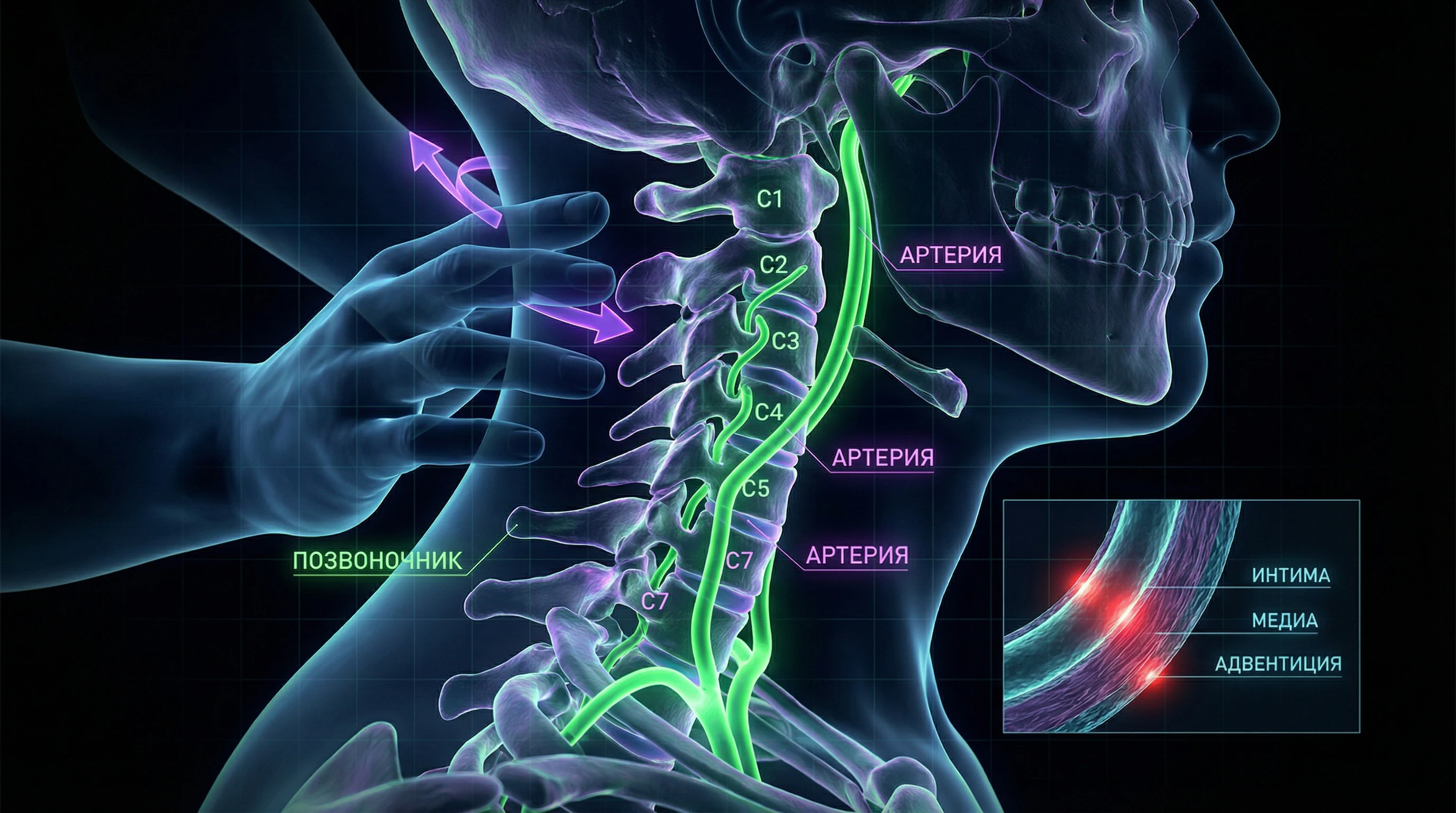
🔁 Anatomical Vulnerability of Vertebral Arteries in the Cervical Spine
The vertebral arteries pass through bony channels (transverse foramina) of cervical vertebrae C6–C1, then make a sharp bend, piercing the dura mater at the level of the atlas (C1), before entering the cranial cavity. This anatomical trajectory makes the arteries particularly vulnerable to mechanical stress during rotational head movements.
During chiropractic manipulation, the patient's head is rapidly rotated and extended, creating significant tension and twisting of the arteries. The vessel, fixed within the bony channel, cannot move freely—all the stress falls on its wall.
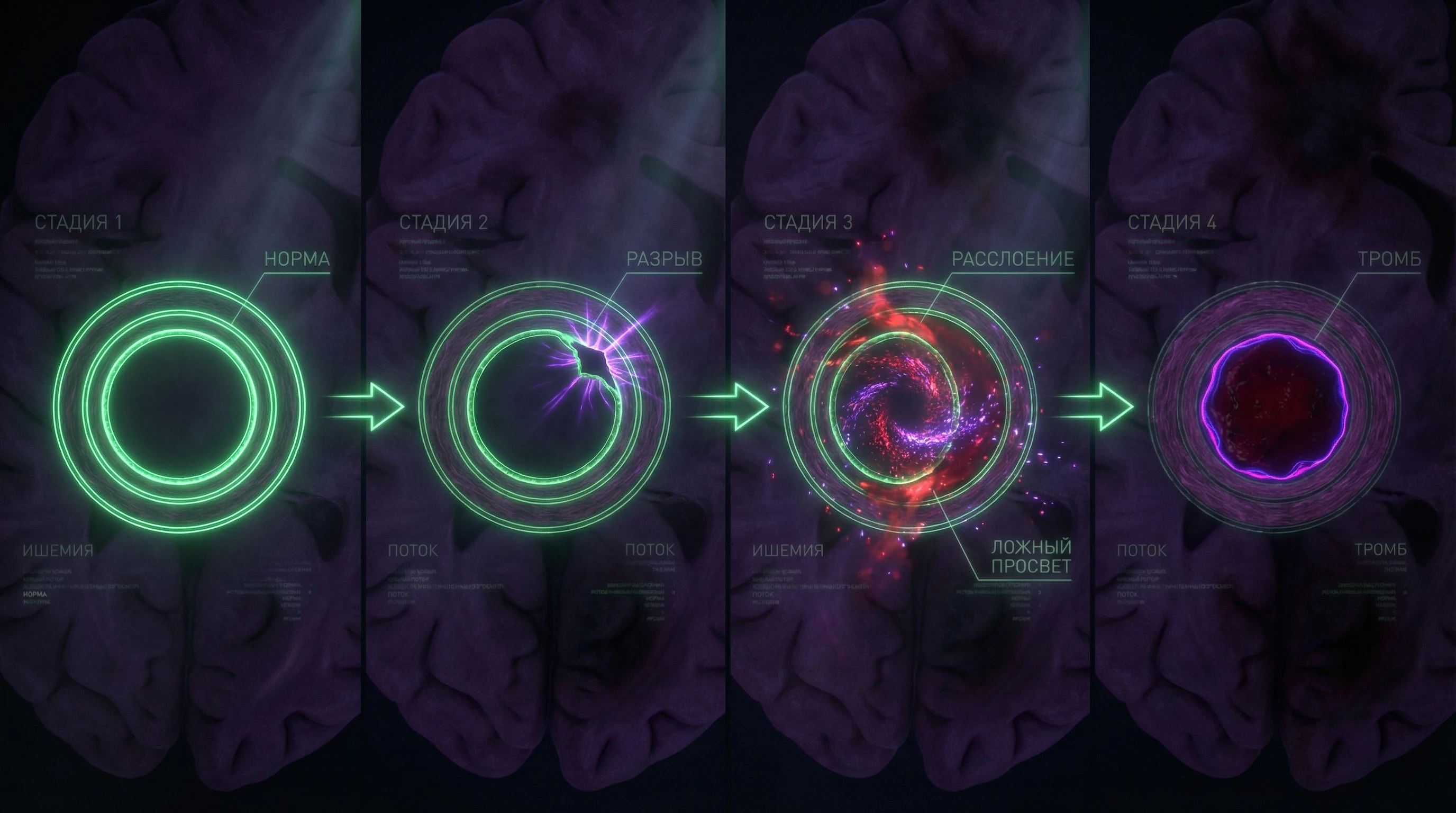
🧠 Mechanism of Intimal Tear: From Mechanical Stress to Dissection
The inner lining of the artery (intima) is a thin layer of endothelial cells that can be damaged by excessive stretching or twisting of the vessel. When the intima tears, blood under pressure penetrates between the layers of the arterial wall, creating a false lumen (S001).
Dissection can develop in two directions: the false lumen expands, compressing the true lumen and causing brain ischemia, or a thrombus forms in the false lumen, breaks off, and causes embolic stroke.
🧷 Factors That Increase Dissection Risk
| Risk Category | Examples | Why It Matters |
|---|---|---|
| Genetic | Ehlers-Danlos syndrome, Marfan syndrome, fibromuscular dysplasia | Weakened arterial connective tissue; often undiagnosed until an event occurs |
| Vascular | Arterial hypertension, smoking | Increased pressure in the vessel + wall fragility |
| Infectious | Recent upper respiratory infections | Inflammation can weaken the arterial wall |
| Pharmacological | Oral contraceptives | Increase risk of thrombus formation in the false lumen |
| Traumatic | Recent neck injuries | Intimal microtrauma may precede manipulation |
The problem is that many of these factors are not diagnosed until the first vascular event, and the patient may be unaware of their vulnerability.
⚙️ Temporal Dynamics: From Moment of Manipulation to Clinical Manifestations
Clinical manifestations of arterial dissection can occur immediately after manipulation or with a delay ranging from several hours to several days (S001). Early symptoms are often nonspecific: increased neck pain, headache, dizziness.
- First 0–6 hours: neck pain, headache, possible autonomic symptoms (sweating, tachycardia)
- 6–24 hours: escalating neurological symptoms (visual disturbances, ataxia, dysarthria)
- 24–72 hours: full stroke presentation (paresis, speech impairment, loss of consciousness)
- After 72 hours: stabilization or progression depending on degree of dissection and thrombus formation
This time delay creates a diagnostic trap: the patient may not connect the deterioration in their condition with a manipulation performed the day before, and seek medical attention too late, when stroke has already developed.
Zone of Uncertainty: Where Evidence Conflicts and Why It Matters
Honest analysis requires acknowledging areas where scientific data is incomplete or contradictory. Learn more in the Logical Fallacies section.
🧩 The Problem of Establishing Causation in Individual Cases
Spinal manipulation—practiced by chiropractors, physical therapists, osteopaths, and physicians—remains controversial without convincing safety evidence (S001). The core methodological problem: most data is based on individual case reports, where alternative explanations cannot be ruled out.
A patient may have had a pre-existing but asymptomatic dissection that became symptomatic independently of manipulation. This doesn't mean manipulation is safe—it means that in an individual case, causality remains uncertain.
Absence of proof of causation in one case ≠ absence of risk in the population. These are two different logical problems.
🔎 Discrepancies in Complication Rate Estimates: From 1:100,000 to 1:2,000,000
Different studies provide different estimates of serious complication rates following chiropractic neck manipulation. Discrepancies stem from methodology: voluntary reporting underestimates, insurance database analysis may include cases without causal connection.
| Data Source | Bias | Impact on Estimate |
|---|---|---|
| Voluntary reporting | Underreporting | Frequency underestimated |
| Insurance databases | False associations | Frequency may be overestimated |
| Physician surveys | Recall, selection | Depends on coverage |
A survey of American Pain Society physicians identified 78 ischemic neurological events, including 13 fatalities (S006). The true frequency remains uncertain, but a pattern exists.
🧾 Stroke Mechanism After Cervical Injections: The Microvascular Hypothesis
The mechanism of stroke following steroid injection into the cervical spine remains unclear. Diffuse posterior circulation involvement is incompatible with classic thromboembolism or vasospasm (S002).
- Classic hypothesis (thromboembolism)
- Thrombus occludes vessel locally. Predicts focal lesion. Doesn't explain diffuse damage.
- Microvascular embolization
- Particles (air, crystals, cellular debris) distribute through capillary network. Explains diffuse posterior circulation damage. Also relevant for manipulations.
This suggests an alternative mechanism that may be common to both injections and manipulations—microvascular injury rather than macroscopic arterial rupture.
Unclear mechanism doesn't mean absence of risk. It means we don't fully understand exactly how the catastrophe occurs.
For practice, this is critical: if the mechanism is microvascular, risk may be higher with repeated manipulations or injections than with a single procedure. Cumulative effect remains unstudied.
Cognitive Anatomy of the Safety Myth: Which Psychological Mechanisms Make Us Ignore Rare Catastrophes
People continue to consider chiropractic manipulations safe despite documented cases of severe complications. This isn't a logical error—it's the result of predictable cognitive biases. Learn more in the Mini-Courses section.
⚠️ Availability Heuristic: Personal Experience Overshadows Statistics
Most people who have undergone manipulations haven't experienced serious complications. This personal experience creates a powerful subjective sense of safety that overshadows abstract statistics about rare catastrophes.
The availability heuristic causes us to assess the probability of an event by how easily examples come to mind. Since arterial dissections are rare and don't receive widespread publicity, they don't form an accessible mental representation of risk (S001).
🕳️ Base Rate Neglect: Focus on Benefits Without Accounting for Costs
When someone experiences pain relief after manipulation, they attribute it specifically to the procedure, ignoring spontaneous improvement, placebo effect, or regression to the mean.
Rare catastrophic complications are perceived as statistical noise. This is classic base rate neglect: focus on the individual case without considering population statistics.
⚖️ Asymmetry in Risk Perception
| Perception | Medical Intervention | Alternative Intervention |
|---|---|---|
| Risk of rare complication | Perceived as inevitable cost of progress | Perceived as proof of method's danger |
| Lack of efficacy evidence | Requires additional research | Interpreted as confirmation of effectiveness |
| Mechanism of action | Must be explained by science | Can remain unclear ("energy," "balance") |
People apply different standards of evidence depending on whether information aligns with their preexisting beliefs. If you already believe in chiropractic safety, a report of a rare stroke is perceived as an exception. If you're skeptical, the same report becomes confirmation of danger.
🔄 Cognitive Dissonance and Investment Defense
Someone who has spent money and time on chiropractic care experiences psychological pressure to justify that investment. Acknowledging that the procedure might be dangerous creates cognitive dissonance between action (I underwent manipulation) and belief (this is dangerous).
Resolution of this conflict often occurs not through risk reassessment, but through benefit reassessment. This is called investment defense: the more invested, the stronger the motivation to believe in a positive outcome.
📊 Social Proof and Normalization
- Social Proof
- If many people visit chiropractors and talk about benefits, this creates the impression that risk is minimal. The absence of visible victims in one's personal circle is interpreted as absence of risk altogether.
- Normalization Through Repetition
- Chiropractic has existed for decades, holds licenses in some countries, is advertised in media. This normalization creates the illusion that risk has already been accounted for and controlled by the system. In reality, licensing doesn't mean proven safety (S003).
- The Trap: Authority Without Accountability
- A chiropractor may be licensed, but this doesn't mean they bear responsibility for rare but catastrophic complications. Patients perceive licensing as a safety guarantee, when in reality it's only professional regulation.
These mechanisms work not because people are foolish. They work because the brain evolved to make decisions under uncertainty with limited information. When information is rare and abstract, while personal experience is concrete and accessible, the brain chooses personal experience.
The chiropractic safety myth isn't the result of conspiracy or ignorance. It's the result of a predictable collision between event rarity and the architecture of human cognition.
Protection from these mechanisms requires not more information, but a change in how it's processed. This means: learning to distinguish personal experience from population statistics, understanding when a rare event remains rare but remains catastrophic, and acknowledging that absence of visible harm doesn't mean absence of risk.
For physicians and patients, this means one thing: demand transparency about rare but serious complications, even if they don't fall within the patient's personal experience. Event rarity doesn't cancel its catastrophic nature.
