What is cervical spine chiropractic manipulation and why has the safety debate persisted for half a century
Cervical spine manipulation (CSM) is a manual technique in which a practitioner applies a sudden, controlled impulse to the neck joints, often accompanied by a characteristic cracking sound. The goal is to restore mobility, relieve muscle tension, and reduce pain. For more details, see the section on Alkaline Diet.
The procedure is popular in the United States, Canada, Australia, and several European countries, where chiropractic is recognized as a legal medical practice. But over the half-century of its existence, the scientific debate about the safety of neck manipulations has not subsided.
⚠️ Anatomical vulnerability: why the neck is not the lower back
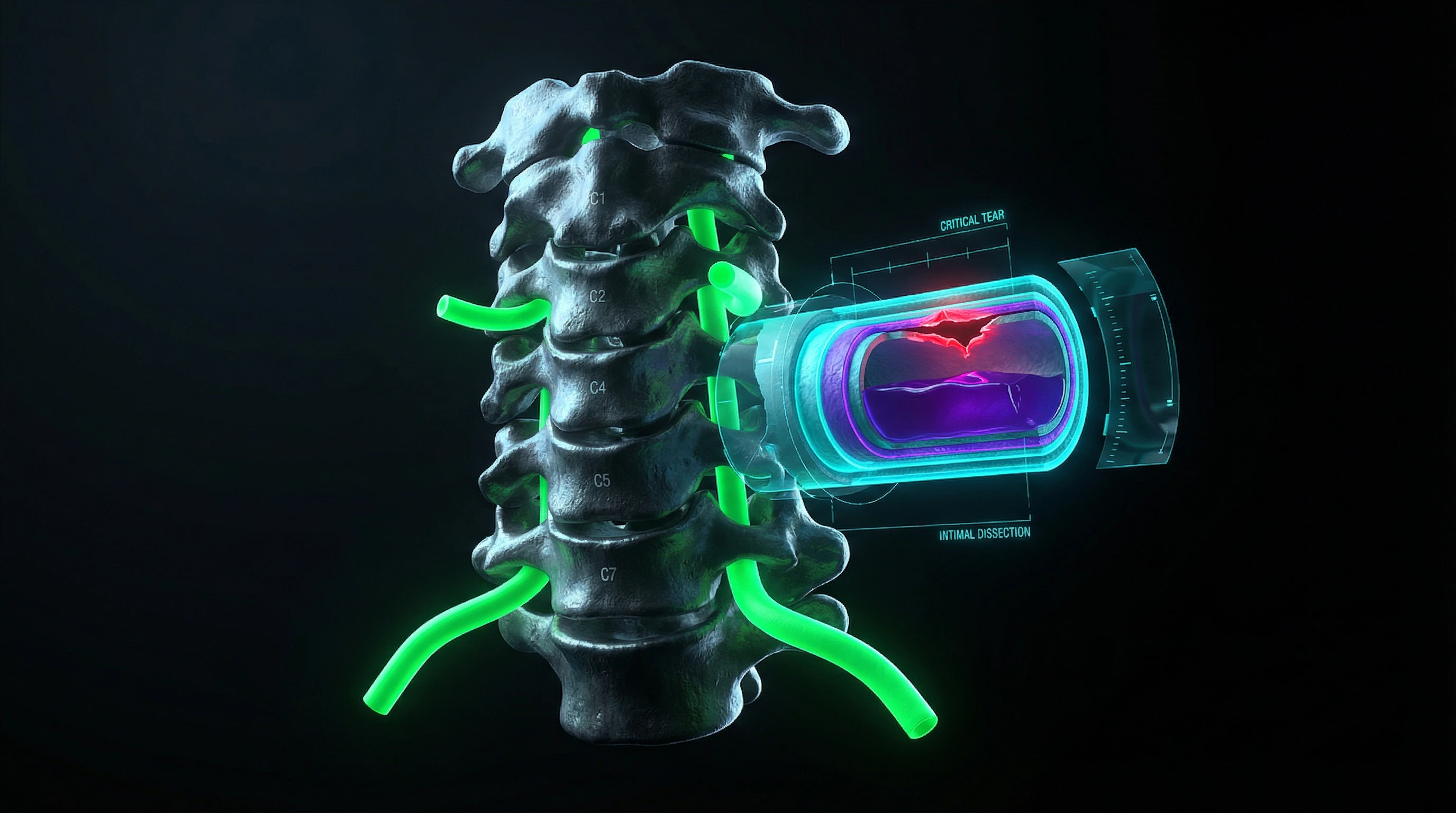
The cervical spine is unique: the vertebral arteries pass through the transverse processes of the cervical vertebrae, supplying blood to the posterior part of the brain, including the brainstem and cerebellum.
Sudden rotation or hyperextension of the neck can theoretically cause mechanical damage to the arterial wall—a dissection, in which blood penetrates between the layers of the vascular wall, forming a hematoma (S005). This hematoma can block the arterial lumen or become a source of thrombus, leading to ischemic stroke (S001).
- Vertebral artery dissection (VAD)
- Rupture of the inner layer of the arterial wall with formation of a hematoma inside the vessel. Can develop spontaneously or after trauma, including manual neck manipulations.
- Vertebral arteries
- Paired vessels passing through openings in the transverse processes of the cervical vertebrae. They supply blood to the cerebellum, brainstem, and occipital lobes.
🧩 Why the debate persists: the methodological trap of rare events
Vertebral artery dissection after chiropractic manipulation is a rare event. Estimates range from 1 case per 100,000 manipulations to 1 per several million (S002).
It is precisely this rarity that makes studying the problem nearly impossible: a statistically significant study would require samples of hundreds of thousands of patients, prospective observation, and control groups. Such studies do not exist.
Instead, we have case series, retrospective reviews, and indirect data—a mosaic from which it is impossible to construct an accurate picture of risk. This creates an ideal environment for opposing interpretations of the same facts.
| Type of evidence | Availability | Limitation |
|---|---|---|
| Prospective randomized trials | Absent | Ethically and practically impossible |
| Retrospective cohort studies | Rare | Selection bias, underreporting of cases |
| Clinical case series | Many | Do not prove causation, only association |
| Systematic reviews | Several | Based on low-quality data |
🔎 Scope of the topic: what we are discussing and what we are not
This article focuses on the link between cervical spine manipulations and stroke risk through the mechanism of vertebral artery dissection.
- We do not discuss the effectiveness of chiropractic in treating pain
- We do not compare it with other treatment methods
- We do not examine manipulations on other parts of the spine
- We focus on the invisible risk, its scale, reasons for ignoring it, and ways to protect the patient
If you are interested in the broader context of manual medicine, see the article on chiropractic and scoliosis.
Seven Arguments from Chiropractic Defenders: Why They Consider Stroke Risk a Myth or Statistical Noise
Professional chiropractic associations, industry-affiliated researchers, and practicing specialists claim that the link between neck manipulations and stroke either doesn't exist or is too weak to warrant attention. Here are their key arguments. More details in the section Folk Medicine vs. Evidence-Based Medicine.
🧩 Argument 1: Correlation Does Not Equal Causation
Vertebral artery dissection occurs spontaneously—from congenital connective tissue weakness, sudden head turns, sneezing, sports. Early symptoms (neck pain, headache) prompt the patient to visit a chiropractor. Stroke occurs hours or days later, creating a false causal relationship.
The chiropractor doesn't cause the dissection—they simply become the last link in a chain of events that has already begun.
🧩 Argument 2: Absolute Risk Is Negligibly Small
Even at the upper bound of estimates (1 stroke per 100,000 manipulations), 99,999 procedures occur without incident. The risk of serious complications from nonsteroidal anti-inflammatory drugs—gastrointestinal bleeding, heart attacks—is significantly higher, yet these medications are sold over the counter.
Why does chiropractic face such criticism when its risk is orders of magnitude lower?
🧩 Argument 3: Absence of Prospective Studies
All data on the link between manipulations and stroke are based on retrospective reviews, case series, and insurance database analyses. Not a single large prospective randomized controlled trial has confirmed a causal relationship.
In evidence-based science, the absence of quality data is interpreted as absence of effect, not its presence.
🧩 Argument 4: Systematic Reviews Find No Convincing Evidence
Several systematic reviews and meta-analyses from the 2000s–2010s concluded that the quality of evidence is extremely low (S002). Methodological limitations (small samples, lack of confounder control, selection bias) make definitive conclusions impossible.
🧩 Argument 5: Spontaneous Dissection Is More Common Than Thought
Population studies show that spontaneous vertebral artery dissection occurs at a rate of approximately 1–1.5 cases per 100,000 people per year (S005). This is comparable to estimates of stroke frequency following chiropractic treatment.
Perhaps the observed cases are simply the background rate of spontaneous dissections, not the result of manipulations.
🧩 Argument 6: Publication Bias
Dramatic stroke cases are actively published in medical journals and media, creating a distorted perception of event frequency. Millions of successful, safe procedures go unnoticed.
This is classic publication bias, which exaggerates the risk of rare catastrophic events.
🧩 Argument 7: Professional Standards Minimize Risk
Modern protocols include preliminary screening for risk factors: young age, connective tissue dysplasia, recent trauma, vascular symptoms. Qualified specialists avoid aggressive manipulations in at-risk patients.
- Collection of trauma history and congenital pathologies
- Assessment of symptoms indicating vascular pathology
- Selection of gentle techniques for high-risk patients
- Informed consent specifying rare but serious complications
Thus, the risk, if it exists, can be minimized through proper clinical practice.
Evidence Base: What Systematic Reviews and Meta-Analyses Actually Tell Us About the Link Between Neck Manipulation and Stroke
Now let's turn to the facts. Over the past three decades, a substantial body of data has accumulated that allows us to assess the scale of the problem. More details in the Pseudomedicine section.
📊 Systematic Reviews: Heterogeneity and Data Quality
Systematic reviews and meta-analyses are the gold standard for synthesizing evidence. But researchers face a fundamental problem: enormous variability in study design and data quality. Standardized definitions are lacking, data collection methods differ, and reporting of confounders is incomplete.
This same problem characterizes research on manipulation and stroke: details of study conduct and dataset composition are often missing, making it difficult to synthesize results and assess the reliability of conclusions.
📊 Risk Estimates: From 1 in 100,000 to 1 in Several Million
The most frequently cited estimate of stroke risk following neck manipulation is 1 to 3 cases per 100,000 procedures. However, this figure is based on retrospective data and may be either overestimated (selection bias) or underestimated (insufficient case reporting). Some studies suggest the true risk may be an order of magnitude lower—1 in a million or rarer.
The problem is that we cannot accurately measure the frequency of an event that occurs so rarely. This doesn't mean the event doesn't exist—it means standard epidemiological methods are inadequate here.
🧪 Biological Plausibility: Mechanism of Injury
Biomechanical studies on cadaveric material and computer modeling show that sudden rotational movements of the neck, especially combined with hyperextension, create significant mechanical loads on the vertebral arteries. The artery stretches, compresses between bony structures, and undergoes shearing forces.
In people with predisposition (congenital connective tissue weakness, fibromuscular dysplasia, recent infection), these loads can exceed the strength of the vascular wall, causing dissection (S005). The mechanism is biologically plausible.
🧾 Case Series: Patterns and Temporal Association
The medical literature contains hundreds of descriptions of stroke occurring within hours or days after neck manipulation (S001, S007). The typical pattern: a young patient (20–40 years) without cardiovascular risk factors visits a chiropractor for neck pain, undergoes a procedure, and within hours develops stroke symptoms (dizziness, coordination problems, double vision).
Imaging confirms vertebral artery dissection and ischemic stroke in the vertebrobasilar territory. The temporal association, absence of alternative explanations, and reproducibility of the pattern all point to a causal relationship.
- Young age (other causes of stroke are rare)
- Absence of pre-existing risk factors
- Neck manipulation immediately preceding symptoms
- Specificity of location (vertebrobasilar territory)
- Imaging confirmation of arterial dissection
🔬 The Problem of Reverse Causation: When Pain Is Already a Symptom
Critics rightly point out: perhaps the patient sought chiropractic care precisely because the arterial dissection process had already begun, manifesting as neck pain. This is a serious objection, but it doesn't explain all cases.
When a patient presents with chronic, stable pain (without acute symptoms), undergoes manipulation, and immediately (within minutes or hours) develops a stroke, reverse causation is unlikely. Moreover, if all cases resulted from spontaneous dissection, we would observe the same frequency of strokes after visits to massage therapists, physical therapists, or general practitioners. But this doesn't happen—the association is specific to cervical chiropractic manipulation.
📊 Insurance Company Data: Statistical Signal
Analysis of insurance databases in Canada and the United States showed a statistically significant increased risk of vertebrobasilar stroke among patients who visited a chiropractor in the preceding week compared to controls (S003, S004). Relative risk ranged from 1.5 to 5 depending on age group and study methodology.
| Data Source | Relative Risk | Age Group | Interpretation |
|---|---|---|---|
| Canadian insurance data | 1.5–2.0 | 45–64 years | Statistically significant, but absolute risk is low |
| Medicare (USA) | 2.0–5.0 | 66+ years | Higher in older age groups |
| Commercial insurers (USA) | 1.5–3.0 | 18–64 years | Association persists across all ages |
These data confirm the existence of an association but don't definitively prove causation. However, the totality of evidence—biological plausibility, case series with clear temporal association, statistical signal in large databases, specificity of association—indicates the link is real, not an artifact.
The question isn't whether the risk exists. The question is how large it is and who is at increased risk. We'll address these questions next.

Mechanism or Coincidence: How to Distinguish Causation from Statistical Artifact in Rare Events
The central question: is the observed association between CSM and stroke a causal relationship or a statistical artifact generated by systematic errors and confounders?
To answer this, we must apply causality criteria — a set of logical filters that separate real mechanisms from coincidences. For more details, see the Scientific Method section.
🧬 Hill's Criteria: Nine Questions for Assessing Causality
Bradford Hill's criteria are a classic epidemiological tool for testing causal relationships (S001). Let's apply them to the CSM–VAD–stroke connection:
- Strength of association — moderate (relative risk 1.5–5). Not extreme, but notable.
- Consistency — the association is reproduced across different studies, countries, and populations (S002, S003).
- Specificity — the association is specific to cervical spine manipulations, not observed with other interventions.
- Temporality — manipulation precedes stroke. This is critical.
- Biological gradient — insufficient data (see below).
- Biological plausibility — the mechanism is understood: rotation and hyperextension of the neck can cause arterial dissection (S005).
- Coherence — consistent with biomechanical and anatomical knowledge.
- Experimental evidence — absent (for ethical reasons).
- Analogy — similar mechanisms of arterial damage are known from other neck injuries (S008).
Most criteria are satisfied. This supports the causality hypothesis but doesn't prove it definitively — especially in rare events, where chance and systematic errors carry greater weight.
🔁 Confounders: What Else Could Explain the Association?
The main confounder is reverse causation: the patient seeks a chiropractor not because manipulation will cause a stroke, but because they're already experiencing symptoms of an incipient dissection (neck pain, dizziness, asymmetric pressure).
Other potential confounders: age (younger people more frequently visit chiropractors and have higher risk of spontaneous dissection), lifestyle (sports activities, injuries), genetic predisposition to connective tissue defects.
- Why these confounders don't explain the entire association:
- None of them explain the specificity of the association to CSM specifically and the temporal proximity of the event (stroke within days after manipulation). If confounders were the main cause, we would expect to see the same association in patients who didn't visit chiropractors.
🧷 Dose-Response: Does More Aggressive Manipulation Mean Higher Risk?
If the relationship is causal, we would expect to see a dose-response effect: more aggressive manipulations (greater amplitude, higher velocity, repeated procedures) should be associated with higher risk (S006, S007).
There is insufficient data to test this hypothesis — most studies don't record details of manipulation technique. This is a critical knowledge gap that leaves room for skepticism.
The absence of dose-response doesn't disprove causality, but it weakens the evidence. In rare events, even weak exposure can be sufficient if it targets vulnerable anatomy.
Conflicts of Interest and Uncertainties: Why the Scientific Community Cannot Reach Consensus and Who Benefits from Maintaining the Status Quo
The debates surrounding cervical chiropractic safety are not purely scientific. They are permeated by conflicts of interest, professional politics, and economic incentives that distort the interpretation of evidence. More details in the section Statistics and Probability Theory.
💰 Economic Interests: The Chiropractic Industry as a Stakeholder
Chiropractic is a multi-billion dollar industry. Over 70,000 chiropractors practice in the United States, performing tens of millions of procedures annually. Recognition of significant stroke risk threatens the profession's reputation, could lead to stricter regulation, rising insurance premiums, and lawsuits.
Professional chiropractic associations actively fund research aimed at refuting the link between manipulations and stroke, and lobby industry interests in regulatory bodies. This creates systematic pressure on the scientific narrative.
🧾 Funding Bias: Who Pays for the Research?
A significant portion of chiropractic safety research is funded by the industry itself or conducted by researchers affiliated with chiropractic colleges. As meta-analyses in other areas of medicine show, funding source systematically influences results: industry-sponsored studies more often reach conclusions favorable to the sponsor (S001).
This doesn't mean data falsification, but can manifest in methodology choices, interpretation of results, selective publication—mechanisms that remain invisible in the final report.
🕳️ Data Gaps: What We Don't Know and Why It's Profitable
The absence of large prospective studies is not coincidental, but the result of systemic factors. Such studies are expensive, require years of observation of enormous cohorts, and their results may be unfavorable to the industry.
Maintaining uncertainty is profitable: in the absence of definitive evidence, one can continue to claim that risk is unproven. As noted in the context of living systematic reviews, "science is rightly admired as a cumulative process, but scientific knowledge is usually built on a patchwork of research contributions without much coordination" (S003). In the case of chiropractic, this patchwork is deliberately not sewn into a complete picture.
- Large prospective studies require funding that has no interest in unfavorable results.
- The absence of mandatory complication registration conceals the true frequency of events.
- A fragmented database allows each side to select convenient studies for their narrative.
⚠️ Regulatory Vacuum: Why the Healthcare System Doesn't Require Mandatory Complication Registration
In most countries, there is no mandatory system for registering complications after chiropractic procedures. Chiropractors are not required to report stroke cases occurring after manipulations. This means the true frequency of events remains unknown.
For comparison: in the pharmaceutical industry, strict pharmacovigilance systems exist requiring reporting of adverse effects. Why isn't the same standard applied to invasive manual procedures? The answer lies in the political economy of regulation: chiropractic has historically positioned itself as an alternative to medicine, not part of it, and has avoided the same degree of oversight.
- Oversight Asymmetry
- Pharmaceutical drugs require registration of every adverse effect; manual procedures do not. This creates an illusion of safety through absence of data.
- Political History of Regulation
- Chiropractic historically fought for professional recognition and avoided integration into the mandatory oversight system that exists for other invasive interventions.
- Economic Interest in Status Quo
- Introducing mandatory complication registration would require infrastructure and could reveal problems that currently remain hidden.
The conflict of interest here is not personal, but structural. No one needs to be blamed—the system simply works to preserve uncertainty. This benefits everyone invested in the status quo: the chiropractic industry, researchers funded by that industry, and regulators who prefer to avoid conflicts.
The patient remains alone in this vacuum. They're told the risk is unproven, but not told that absence of evidence is not evidence of absence, especially when the system actively prevents collection of that evidence. This is a cognitive trap built into the very structure of the scientific and regulatory landscape.
Cognitive Anatomy of the Myth: Which Psychological Mechanisms Cause Patients and Doctors to Underestimate the Risk of Rare Catastrophic Events
Even if the evidence of risk were crystal clear, psychological factors would prevent its adequate perception. The human brain is poorly adapted to assess rare but catastrophic risks. Learn more in the Mini-Courses section.
🧩 Availability Heuristic: "I've Never Heard of Such Cases"
People assess the probability of an event by the ease with which they can recall examples. If a person doesn't know anyone who suffered a stroke after chiropractic treatment, they intuitively consider this risk zero or negligibly small.
This is the classic availability heuristic, which systematically distorts the perception of rare events. Millions of safe procedures create an illusion of absolute safety.
- Rare event = hard to recall = seems improbable
- Frequent favorable outcomes = easy to recall = seem like a guarantee
- Absence of personal experience = absence of risk (logical fallacy)
- Media silence about rare complications = additional reinforcement of the illusion
Doctors fall into the same trap. If a neurologist has seen one patient with stroke after neck manipulation in 20 years of practice, while a chiropractor has seen thousands of successful procedures, the cognitive weight of the first event is lost in the noise of the second.
Rarity of an event does not mean its impossibility. Rarity means statistics are needed, not memory.
🎯 Confirmation Bias and Evidence Filtering
Defenders of chiropractic seek out and remember studies confirming safety, and ignore or reinterpret those indicating risk (S002). Patients who have chosen chiropractic are motivated to believe in its safety—cognitive dissonance is too costly.
Doctors recommending manipulations face the same bias: acknowledging risk requires reevaluation of their own recommendations and possible admission of harm.
- Confirmation Bias
- Active search for information confirming existing beliefs, and ignoring contradictory information. In the context of chiropractic: a doctor remembers successful cases, forgets complications, reinterprets statistics in favor of the method.
- Cognitive Dissonance
- Psychological discomfort from contradiction between action (choosing chiropractic) and information (stroke risk). Resolved by denying the risk rather than refusing the procedure.
📊 Numerical Blindness and Inability to Work with Small Probabilities
The risk of stroke after neck manipulation is estimated at 1 in 5 million or 1 in 100,000 procedures (S003, S004). For a person, this number has no intuitive meaning.
The brain works well with probabilities of 10%, 50%, 90%. But 0.00002%? This is perceived as "practically zero." At the same time, people overestimate the risk of rare but dramatic events (plane crashes, terrorist attacks) if they are frequently covered in media.
| Risk | Intuitive Perception | Actual Behavior |
|---|---|---|
| 1 in 5 million (stroke after chiropractic) | "Zero, not concerned" | Ignored, even if known |
| 1 in 100 (drug side effect) | "Maybe, but unlikely" | Weighed against benefit |
| 1 in 10,000 (plane crash) | "Scary, won't fly" | Overestimated if in the news |
🔄 Social Proof and Authority
If a neighbor, friend, or celebrity recommends chiropractic and speaks of its benefits, this creates social proof. If a doctor (authority figure) recommends manipulations, this strengthens trust.
The absence of visible victims in one's personal circle is interpreted as proof of safety. Rare strokes remain invisible because they are rare and often attributed to other causes (S001).
Social proof works best when there is no objective way to verify information. The rarity of the event makes verification impossible.
⏱️ Future Discounting and Illusion of Control
The patient gets relief from neck pain today. The risk of stroke is in an uncertain future and seems avoidable ("it won't happen to me"). This is the illusion of control: a person believes that a rare event won't happen specifically to them.
Doctors performing manipulations for years without complications develop a false sense of mastery: "I know how to avoid the risk." Statistics of rare events cannot refute personal experience.
The connection to the myth of vertebral realignment reinforces the belief in the controllability of the process. If a vertebra can be "realigned," then complications can also be avoided.
🎭 Narrative and Meaning-Making
Chiropractic is embedded in a narrative about "natural medicine," "restoring balance," "activating the body's own forces." This narrative is psychologically attractive and creates meaning.
Stroke is an accident, a technical error, an exception. The narrative remains intact. A patient who suffered a stroke often reinterprets the event: "It's a coincidence," "I was at risk," "The doctor made a mistake," but not "The method is dangerous."
Narrative is stronger than statistics. A person believes the story that explains their experience, even if that story is untrue.
These mechanisms work not because people are stupid, but because the brain evolved to make decisions under conditions of frequent, visible risks, not rare, hidden catastrophes. Cervical chiropractic is a perfect storm for cognitive errors: rare risk, visible benefit, social approval, attractive narrative.
