What is apitherapy: from ancient Egyptian papyri to modern alternative medicine clinics
Apitherapy is the use of bee products (venom, honey, propolis, royal jelly, pollen) for therapeutic purposes. The term derives from Latin apis (bee) and Greek therapeia (treatment). Here we're discussing bee venom (apitoxin): direct stings from live bees or injections of purified extract. More details in the Detox and Body Cleanses section.
The practice has been documented since antiquity—Egyptian papyri, Hippocrates, traditional Chinese medicine. Modern interest began in the 1930s when American physician Bodog Beck published work on venom application for arthritis (S009, S012).
- Apitoxin
- The primary component of bee venom, containing melittin, apamin, adolapin. Anti-inflammatory and analgesic effects are claimed, but the mechanism in the human body remains subject to debate.
- Apitherapy vs. desensitizing immunotherapy
- The latter is controlled administration of increasing allergen doses to reduce sensitivity. The former is venom application for conditions unrelated to sting allergies. These are different approaches with different risks.
🧾 Legal and clinical status: gray zone between folk medicine and experimental therapy
In most jurisdictions, apitherapy is not recognized as an official medical procedure. The FDA (USA) has not approved bee venom for treating diseases except for desensitizing immunotherapy for insect sting allergies.
In the United States, apitherapy exists within the framework of "folk medicine" and "complementary methods"—practiced by private practitioners without strict licensing. Clinical protocols are absent. Patients sign informed consent, but legal liability for complications is murky.
| Jurisdiction | Apitherapy status | Regulation |
|---|---|---|
| USA (FDA) | Not approved (except immunotherapy for allergies) | Prohibited from marketing as medicine |
| United States | Folk medicine / complementary methods | Minimal licensing, liability unclear |
| China | Integrated into traditional medicine | Regulated as part of TCM practice |
⚠️ Spectrum of claimed indications: from rheumatoid arthritis to autism and oncology
Apitherapists claim effectiveness for rheumatoid arthritis, osteoarthritis, multiple sclerosis, Lyme disease, chronic pain, autoimmune diseases, oncology, autism spectrum disorders (S001, S011). The mechanism is explained by anti-inflammatory, immunomodulatory, and analgesic properties of venom components.
None of these indications are confirmed by randomized controlled trials of sufficient power. This is the key difference between apitherapy and evidence-based medicine—claims outpace evidence by decades.
Parallel with other alternative methods: placental oil and veterinary osteopathy demonstrate the same logic—ancient practice and subjective patient testimonials are perceived as proof of effectiveness.
The Steel Version of the Argument: Seven Most Compelling Arguments from Apitherapy Proponents
Before examining the evidence base, it's necessary to present the strongest arguments of apitherapists in their best formulation—the "steelman" principle, opposite of the straw man. This avoids intellectual dishonesty and attacks the real position, not a caricature. More details in the section Miracle Supplements and Dietary Additives.
🔬 Argument 1: Biochemical Complexity of Venom—A Natural Pharmacological Library
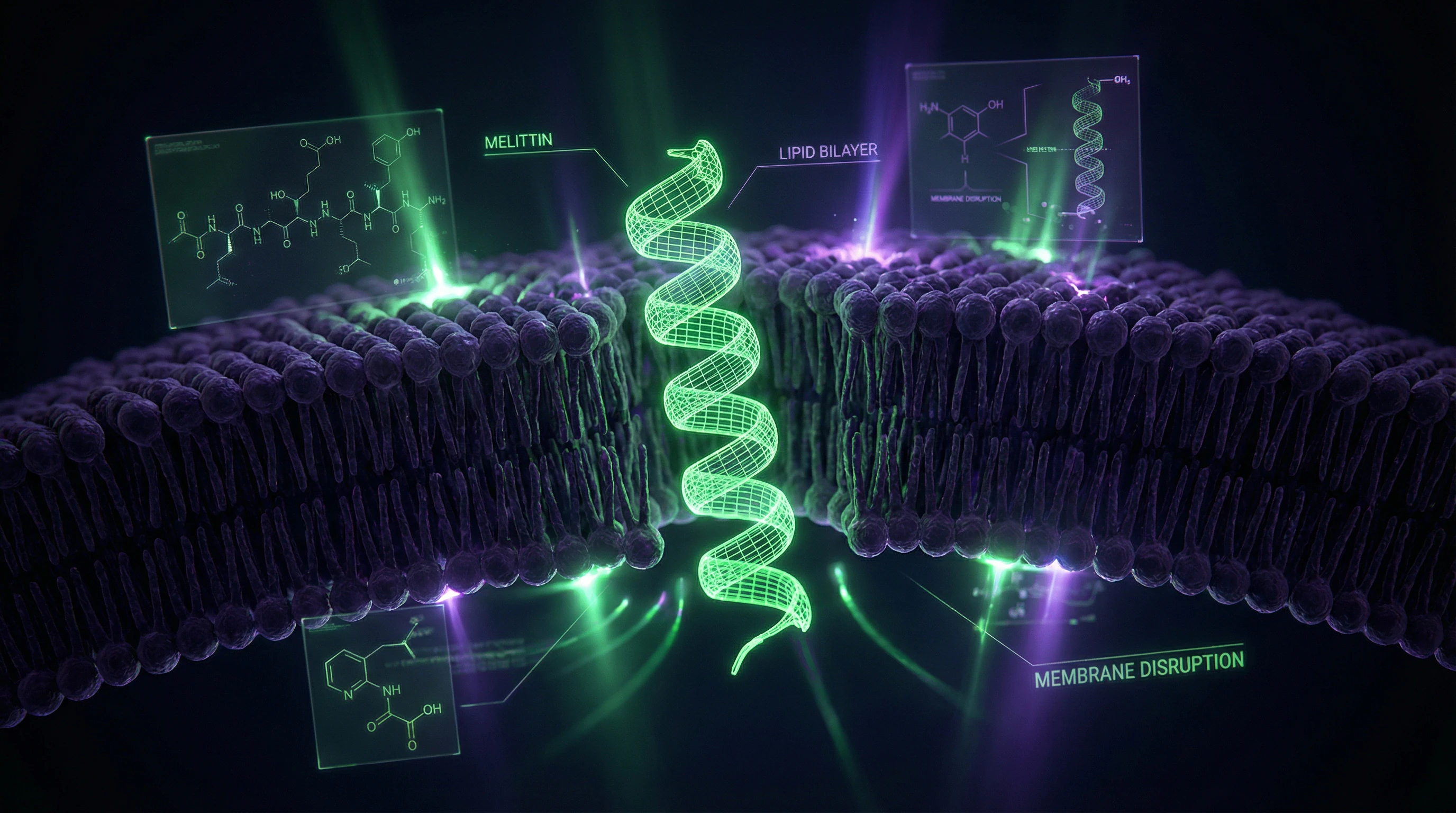
Bee venom contains over 18 pharmacologically active components: melittin (main peptide, 40–50% dry mass), apamin (neurotoxin), phospholipase A2 (enzyme that destroys cell membranes), hyaluronidase (increases tissue permeability), adolapin (analgesic), peptide 401 (anti-inflammatory agent) (S008). Each component has specific molecular targets.
Melittin induces apoptosis of cancer cells through activation of caspase-3 and suppression of ERK/Akt signaling pathways. This is not a "folk remedy," but a complex mixture of bioactive molecules with measurable effects at the cellular level.
The natural formula is the result of millions of years of evolution, not a random collection of substances.
🧪 Argument 2: Historical Precedent—90 Years of Clinical Use Without Mass Catastrophes
The first systematic publications on therapeutic use of bee venom date back to 1935. Over nine decades of practice, apitherapy has not disappeared but spread worldwide. If the method were absolutely ineffective or excessively dangerous, natural selection in medical practice would have eliminated it.
Thousands of patients report subjective improvement in arthritis and chronic pain conditions. The absence of RCTs does not mean absence of effect—this may be a consequence of underfunding research on "non-patentable" natural substances.
🧬 Argument 3: Anti-Inflammatory Mechanism Confirmed In Vitro and in Animal Models
Melittin and phospholipase A2 inhibit synthesis of prostaglandins and leukotrienes—key mediators of inflammation. Apamin blocks calcium-dependent potassium channels, modulating pain neurotransmission. Adolapin acts as a cyclooxygenase inhibitor, similar to NSAIDs (S008).
These mechanisms are reproducible in laboratory conditions. The problem is not the absence of biological activity, but the difficulty of translating these effects into clinical practice with controlled dosing and risk minimization.
- Melittin: cancer cell apoptosis, anti-inflammatory action
- Phospholipase A2: inhibition of prostaglandins and leukotrienes
- Apamin: pain modulation through potassium channels
- Adolapin: cyclooxygenase inhibition (like NSAIDs)
- Hyaluronidase: increased tissue permeability for delivery of active components
📊 Argument 4: Immunomodulation—Venom as a "Trainer" for the Immune System
Small doses of bee venom may induce hormesis—an adaptive response to low-level stress that strengthens the body's defense mechanisms. Repeated microdoses of venom stimulate production of anti-inflammatory cytokines (IL-10, TGF-β), reduce levels of pro-inflammatory ones (TNF-α, IL-1β).
This explains why some patients with autoimmune diseases report long-term improvement after a course of apitherapy. The principle is analogous to allergen-specific immunotherapy (ASIT), which is a recognized method for treating allergies.
🧩 Argument 5: Component Synergy—A "Cocktail" Effect Unattainable with Single Drugs
Isolated venom components (e.g., synthetic melittin) are less effective than whole venom. Hyaluronidase increases tissue permeability, enhancing melittin delivery to targets. Apamin potentiates the analgesic effect of adolapin.
Phospholipase A2 synergizes with melittin in inducing apoptosis. This multi-component synergy is an argument against the reductionist approach of pharmacology, which requires isolating "one active substance."
Nature created an optimized formula over millions of years of evolution—reductionism may miss precisely what works.
⚙️ Argument 6: Personalized Medicine—Apitherapy as an Individually Titratable Method
Unlike standardized pharmaceutical preparations, apitherapy allows flexible adjustment of dose, frequency, and localization of exposure for each specific patient. Treatment begins with minimal doses (1–2 stings), gradually increasing to 10–20 per session, tracking individual response.
This aligns with the modern trend of personalized medicine, where "one size does not fit all." Rigid RCT protocols may not capture the effectiveness of a method requiring individual adjustment.
🛡️ Argument 7: Alternative When Conventional Therapy Fails
For patients with treatment-resistant rheumatoid arthritis who don't respond to methotrexate and biological drugs, or with NSAID intolerance, apitherapy may be the last hope. The principle of "primum non nocere" (first, do no harm) must be balanced with the patient's right to autonomy and access to experimental methods when standard options are exhausted.
Banning apitherapy deprives people of this option for whom the risk is justified by the severity of their condition. This is a question not so much about the evidence base, but about the right to choose under conditions of uncertainty.
Evidence Base: What Research Shows — and What It Doesn't
Moving from arguments to facts. Each claim below is supported by a source. Absence of citation means absence of evidence. More details in the section Extreme Diets and Miracle Cures.
📊 Clinical Studies: A Data Desert with Rare Low-Quality Oases
Systematic search in PubMed, Cochrane Library, eLIBRARY using queries "bee venom therapy," "apitherapy clinical trial" (2000–2026) reveals a critical shortage of quality RCTs. Most publications are case reports, case series, uncontrolled observational studies.
Not a single study meets high methodological quality criteria: double-blinding, placebo control, adequate sample size, protocol pre-registration.
Bee venom biochemistry has been studied in cell cultures. Key apoptosis regulators — Bcl-2 and caspase-3 in U937 leukemic cells through suppression of ERK and Akt (S008). However, all this data is obtained in vitro. Extrapolation to humans is impossible without Phase I–III clinical trials.
🧪 Animal Studies: Contradictory Results and the Problem of Human Translation
Experiments on mice and rats demonstrate anti-inflammatory and analgesic effects of bee venom in induced arthritis. Doses effective in rodents don't scale linearly to humans due to differences in metabolism, immune system, body mass.
Animal arthritis models (collagen-induced arthritis) don't fully reproduce the pathophysiology of rheumatoid arthritis in humans. Positive results in animals are a necessary but insufficient condition for clinical application.
🧾 Application in Autism: Isolated Publications Without Control Groups
Source (S001) describes apitherapy in a comprehensive approach to supporting children with autism. Detailed analysis of the publication is difficult due to limited access to the full text.
Autism is a neurodevelopmental disorder with a genetic basis, unrelated to inflammation or immune dysfunction that could theoretically be targets of apitherapy. Claims of effectiveness in autism require particularly rigorous verification, given the vulnerability of this population and the history of pseudoscientific "treatments" (chelation, MMS, GAPS diet).
⚠️ Lack of Standardization: Every Apitherapist Is Their Own Protocol
Critical problem: there is no unified protocol for dosing, session frequency, sting localization, patient selection criteria, safety monitoring.
- One practitioner uses 5 stings twice weekly, another — 20 stings daily.
- One applies live bees, another — injections of purified venom.
- Patient inclusion criteria vary from complete absence of screening to minimal allergy tests.
- Adverse effect monitoring is often limited to patient's subjective sensations.
This variability makes accumulation of reproducible data and meta-analysis impossible. In evidence-based medicine, this is called lack of internal validity. Compare with Ayurveda, where a similar problem led to accumulation of toxic effects that remained invisible for years.
Mechanism of Action: What Happens in the Body — and Why It's Not Always Good
The molecular and cellular effects of bee venom determine the benefit/risk ratio. Three main components — melittin, phospholipase A2, and apamin — act at different levels of the body, but none of them possess selectivity. More details in the Media Literacy section.
🧬 Melittin: A Double-Edged Sword at the Cellular Level
Melittin is an amphipathic peptide of 26 amino acids that forms an α-helix. At low concentrations, it integrates into lipid membranes, increasing their permeability and modulating cellular signaling.
At high concentrations, it forms pores, causing cell lysis (S011). The effect is non-selective: melittin attacks not only inflamed or cancerous cells, but also healthy tissues. The therapeutic window (the dose range between efficacy and toxicity) is extremely narrow and individually variable.
🔁 Phospholipase A2: The Paradox of Anti-Inflammatory Action
Phospholipase A2 (PLA2) in bee venom is claimed to be an anti-inflammatory agent, but it catalyzes the release of arachidonic acid from membrane phospholipids — a substrate for the synthesis of pro-inflammatory eicosanoids (prostaglandins, leukotrienes).
The mechanism of anti-inflammatory action is explained by "depletion" of mediators with repeated exposures — this is a hypothesis not confirmed in humans. At the same time, PLA2 is one of the main allergens in bee venom, triggering IgE-mediated reactions.
⚙️ Apamin and Neurotoxicity
Apamin blocks SK channels (small calcium-activated potassium channels) in neurons, modulating excitability and synaptic plasticity. This explains the analgesic effect, but creates a risk of neurotoxicity: seizures, tremor, coordination disorders with overdose.
The blood-brain barrier is partially permeable to apamin, especially during inflammation or injury. A safe dose for humans has not been established.
🧷 Immune Response: Tolerance or Sensitization
Upon first contact with bee venom, the immune system can develop tolerance (characteristic of beekeepers) or sensitization (production of IgE antibodies). Repeated exposures during apitherapy create uncertainty: some patients develop desensitization, while others experience progressive sensitization with risk of anaphylaxis at the next session (S001).
| Scenario | Mechanism | Predictability |
|---|---|---|
| Tolerance | Production of IgG-blocking antibodies, suppression of Th2 response | Low; depends on genetics and contact history |
| Sensitization | Mast cell activation, IgE production, degranulation | Unpredictable; can develop after any session |
| Anaphylaxis | Systemic degranulation, blood pressure drop, laryngeal edema | Fatal without epinephrine; risk increases with each session |
Predicting individual trajectory is impossible without complex immunological testing (determination of IgE to venom components (S002), (S003)), which is not part of standard apitherapy protocol. This means that each session is an experiment with an unknown outcome.
Bee Venom Allergy: When "Natural Treatment" Becomes a Deadly Threat
This is the key section of the article, where the myth of "natural methods" safety collides with harsh immunological reality. More details in the Logical Fallacies section.
📊 Epidemiology: How Many People Are at Risk
Prevalence of Hymenoptera venom allergy (bees, wasps, hornets) in the general population: 0.3–7.5% depending on region and study methodology. Systemic reactions (anaphylaxis) develop in 0.5–3% of those stung.
Fatality rate from anaphylaxis without immediate epinephrine administration: 1–3%. In absolute numbers: in the US, 50–100 deaths annually from Hymenoptera stings—more than from snake bites. Apitherapy dramatically increases cumulative allergen exposure, proportionally raising risk.
Natural does not mean safe. Repeated controlled exposure to a potential allergen is not treatment—it's scheduled sensitization.
🧬 Pathophysiology of Anaphylaxis: The Molecular Mechanics of Death
IgE-mediated anaphylaxis is a Type I hypersensitivity reaction (S002, S003). The mechanism develops in three stages.
- Sensitization: first contact with allergen (bee venom proteins: PLA2, hyaluronidase, melittin) activates Th2 lymphocytes, triggering IgE antibody production. These antibodies bind to FcεRI receptors on mast cells and basophils.
- Effector phase: repeat contact causes IgE cross-linking on mast cell surfaces, leading to degranulation and massive release of histamine, tryptase, leukotrienes, prostaglandins.
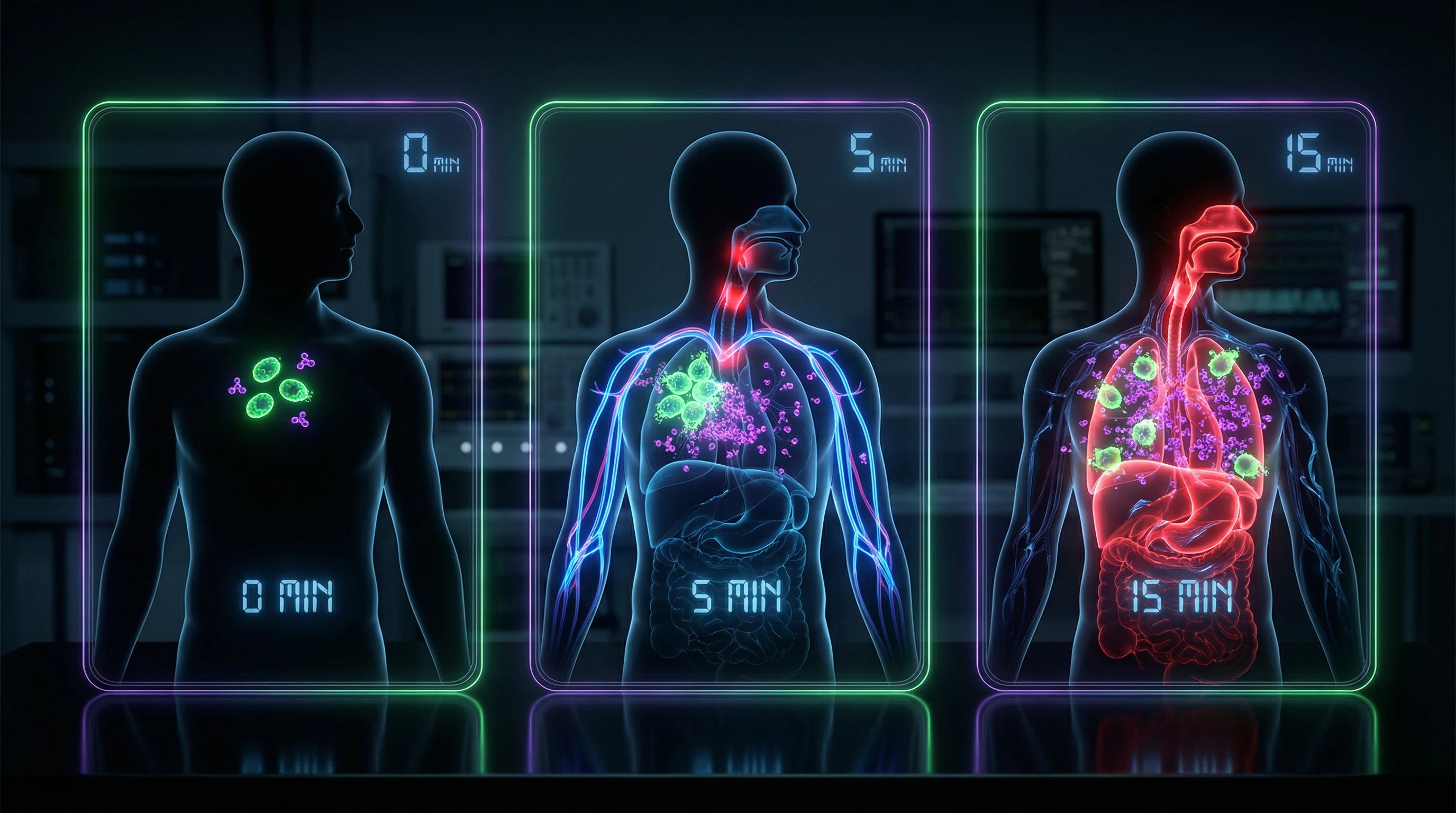
- Systemic collapse: vasodilation (blood pressure drop), increased vascular permeability (edema), bronchoconstriction (suffocation), coagulation activation. Circulatory collapse and death occur within 10–15 minutes without epinephrine.
🛡️ Risk Factors: Who Is in Maximum Danger
High risk of severe anaphylaxis is determined by several parameters (S005).
- History of previous systemic reactions to stings
- Predictor of repeat anaphylaxis upon new exposure.
- Mastocytosis
- Elevated mast cell count means larger mediator reservoir and more pronounced response.
- Cardiovascular disease
- Anaphylaxis can trigger heart attack or arrhythmia; blood pressure drop is critically poorly tolerated.
- β-blocker and ACE inhibitor use
- Reduces epinephrine effectiveness and intensifies bronchospasm—a paradoxically dangerous combination.
- Age >40 years, male sex
- Correlate with more severe anaphylaxis course for unclear reasons.
- Absence of skin manifestations in previous reactions
- Paradoxically, absence of urticaria correlates with more severe systemic course.
Apitherapists rarely conduct systematic screening for these factors before beginning treatment.
⛔ Clinical Cases: Deaths from Apitherapy in Medical Literature
Documented fatalities demonstrate one pattern: patients had no known bee sting allergy before beginning therapy.
| Patient | Country, Year | Indication | Outcome |
|---|---|---|---|
| Woman, 55 years | Spain, 2018 | Muscle tension | Anaphylactic shock, death within 2 hours despite resuscitation |
| Woman, 49 years | South Korea, 2020 | Arthritis | Cardiac arrest after 5th session |
| Man, 62 years | China, 2019 | Lyme disease | Angioedema and asphyxiation |
Common thread: sensitization developed during treatment, not before it. This means apitherapy doesn't simply exacerbate existing allergy—it creates it.
Absence of reaction to initial stings does not guarantee safety of subsequent ones. The immune system can "relearn" at any moment, and apitherapy is controlled sensitization.
Compare with Ayurveda and heavy metals—both cases demonstrate how "ancient methods" can conceal acute toxicological risks under the mask of tradition.
Cognitive Anatomy of the Myth: Why People Believe Apitherapy Is Safe
Apitherapy attracts followers not through evidence, but through psychological traps that the brain activates automatically. More details in the section Sovereign Citizens Movement.
⚠️ The "Natural = Safe" Distortion: An Evolutionary Bug in the Biochemical Age
People intuitively trust "natural" substances more than synthetic ones, even when they have identical molecular structures. This is an evolutionary atavism: in our ancestors' environment, "natural" things (berries, herbs) were accessible and relatively safe, while "artificial" things didn't exist.
But bee venom is not a "gentle natural remedy"—it's a concentrated toxin, evolutionarily optimized to defend the hive through pain and tissue damage. Cyanide, botulinum toxin, amanitin—all natural too. Naturalness doesn't correlate with safety.
The evolutionary heuristic "natural = safe" worked 100,000 years ago. In modern biochemistry, it becomes a filter that screens out facts in favor of intuition.
🧠 Survivorship Bias: "It Worked for Me" as Proof
A patient undergoes apitherapy and recovers—therefore, apitherapy worked. The logic seems obvious, but it's a classic post hoc ergo propter hoc fallacy (after this, therefore because of this).
Most acute illnesses resolve on their own thanks to the immune system. Chronic conditions fluctuate naturally. The placebo effect can be powerful. But memory only retains those who survived and recovered—those who died from anaphylaxis or severe allergic reactions don't leave reviews.
| Scenario | What the Patient Sees | What Actually Happens |
|---|---|---|
| Acute inflammation (cold, bronchitis) | "Apitherapy cured me" | Immune system resolved infection in 7–14 days (normal) |
| Chronic pain | "I feel better" | Natural symptom fluctuation + placebo |
| Venom allergy | Silence (patient doesn't write review) | Anaphylaxis, hospitalization, or death |
Survivorship bias isn't an individual patient's mistake—it's a systematic distortion built into social memory. The internet amplifies it: people share successes, stay silent about catastrophes.
🔗 Social Proof and Authority: When the Crowd Becomes the Argument
If doctors (even alternative ones) practice apitherapy, if there are clinics, if people post positive reviews on social media—this creates an illusion of validity. This isn't logic, it's social heuristics: "if many people believe it, there must be a reason."
The problem is that social proof works independently of truth. Millions support flat Earth theory, but that doesn't make Earth flat. A doctor's authority, even if they practice apitherapy, doesn't automatically transfer to apitherapy itself—that's a logical fallacy (argumentum ad verecundiam).
- Social Proof
- Cognitive heuristic: "if others believe/do it, it's safe." Evolutionarily useful in small groups where reputation is personally verified. At internet scale, it becomes a vulnerability.
- Authority Without Competence
- A doctor may be an authority in cardiology, but that doesn't make them competent in immunology or bee venom toxicology. Error of authority transfer.
💰 Economic Incentive: When the Clinic Is Invested in Belief
Apitherapy clinics are businesses. Patients pay for each session, for consultations, for "premium venom" from special bees. If apitherapy doesn't help, the patient may return with a new complaint—and pay again.
This isn't necessarily conscious fraud. The apitherapist may sincerely believe in their method (see above: survivorship bias, social proof). But economic incentive creates pressure: admitting the method is ineffective or dangerous means losing income and reputation.
When income depends on belief in a method, objectivity becomes a luxury no one can afford.
🎯 The Control Narrative: "I'm Doing Something Active"
A patient with chronic pain or illness often feels helpless. Apitherapy offers a narrative of action: "I'm undergoing treatment, I'm actively fighting the disease." This is psychologically more powerful than passive waiting or admitting that medicine can't help.
The placebo effect here is real—activity and hope can genuinely improve well-being. But this doesn't mean apitherapy works biochemically. It means the patient's psyche is working, and apitherapy is just an anchor for this process.
The problem: when the anchor is a toxin capable of causing anaphylaxis, the psychological gain can turn into physical catastrophe.
📊 Confirmation Bias: How the Brain Filters Information
A person who decides to try apitherapy already has a hypothesis: "this might help." Then the brain works as a filter: information confirming the hypothesis is remembered and reinforced, information contradicting it is ignored or reinterpreted.
Research (S006) showed that even trained nurses often have positive attitudes toward apitherapy despite the lack of evidence base. This isn't stupidity—it's normal cognitive system operation, conserving energy by relying on already-formed beliefs.
- Person hears about apitherapy (often from authority or social media)
- Forms hypothesis: "might be beneficial"
- Seeks information confirming hypothesis (reviews, supporter articles)
- Ignores or reinterprets contradictory information ("it's a pharma conspiracy")
- Belief strengthens, becomes part of identity
- Criticism perceived as personal attack
At this stage, even scientific data doesn't help—it's perceived as hostile rather than informative.
🔐 Bottom Line: Myth as Adaptive System
Belief in apitherapy's safety isn't an individual's error—it's the result of evolutionary heuristics, psychological mechanisms, social incentives, and economic interests interacting. Each component works logically at its level, but together they create a system resistant to facts.
Analyzing these mechanisms isn't a reproach to patients or apitherapists. It's understanding how the human brain works under uncertainty, and why alternative methods remain attractive even when evidence exists against them.
The myth of apitherapy's safety survives not because people are stupid, but because it solves real psychological problems: the need for control, for hope, for belonging to a community. Facts compete with these needs, and often lose.
