The ketogenic diet is not a trendy weight-loss fad, but a strict medical protocol with a 4:1 ratio of fats to proteins and carbohydrates, used to treat drug-resistant epilepsy in children. Research from Central Asia demonstrates the method's effectiveness for specific forms of epilepsy, including GRIN-associated syndromes. However, this is not a universal solution: it requires rigorous medical supervision, precise macronutrient calculation, and readiness for side effects—from growth delays to kidney stones.
📌 What Medical Ketogenic Diet Is and Why It Has Nothing to Do with Instagram Keto
When most people hear "ketogenic diet," they picture a trendy weight-loss approach with bacon for breakfast and avocado for lunch. The medical ketogenic diet for treating epilepsy is an entirely different universe. More details in the section Essential Oils as a Cure-All.
This is not a lifestyle or a choice—it's a strict therapeutic protocol developed nearly a century ago and applied under rigorous medical supervision (S001).
Definition and Key Parameters
The classic ketogenic diet for epilepsy uses a ratio of fats to combined proteins and carbohydrates of 4:1 or 3:1 by weight. For every 4 grams of fat, there is only 1 gram of protein and carbohydrates combined (S002).
| Parameter | Standard Diet | Medical Ketogenic |
|---|---|---|
| Carbohydrates | 50–60% | 4% |
| Proteins | 15–20% | 6% |
| Fats | 25–35% | 90% |
Every meal is calculated down to the gram. Parents weigh food on digital scales, use specialized calculators to determine ketogenic ratios.
A 5-gram error in carbohydrates can pull a child out of ketosis and eliminate the therapeutic effect (S001). This is not a diet you can "try out"—it's a medical intervention requiring the discipline of a surgical procedure.
Metabolic Switch
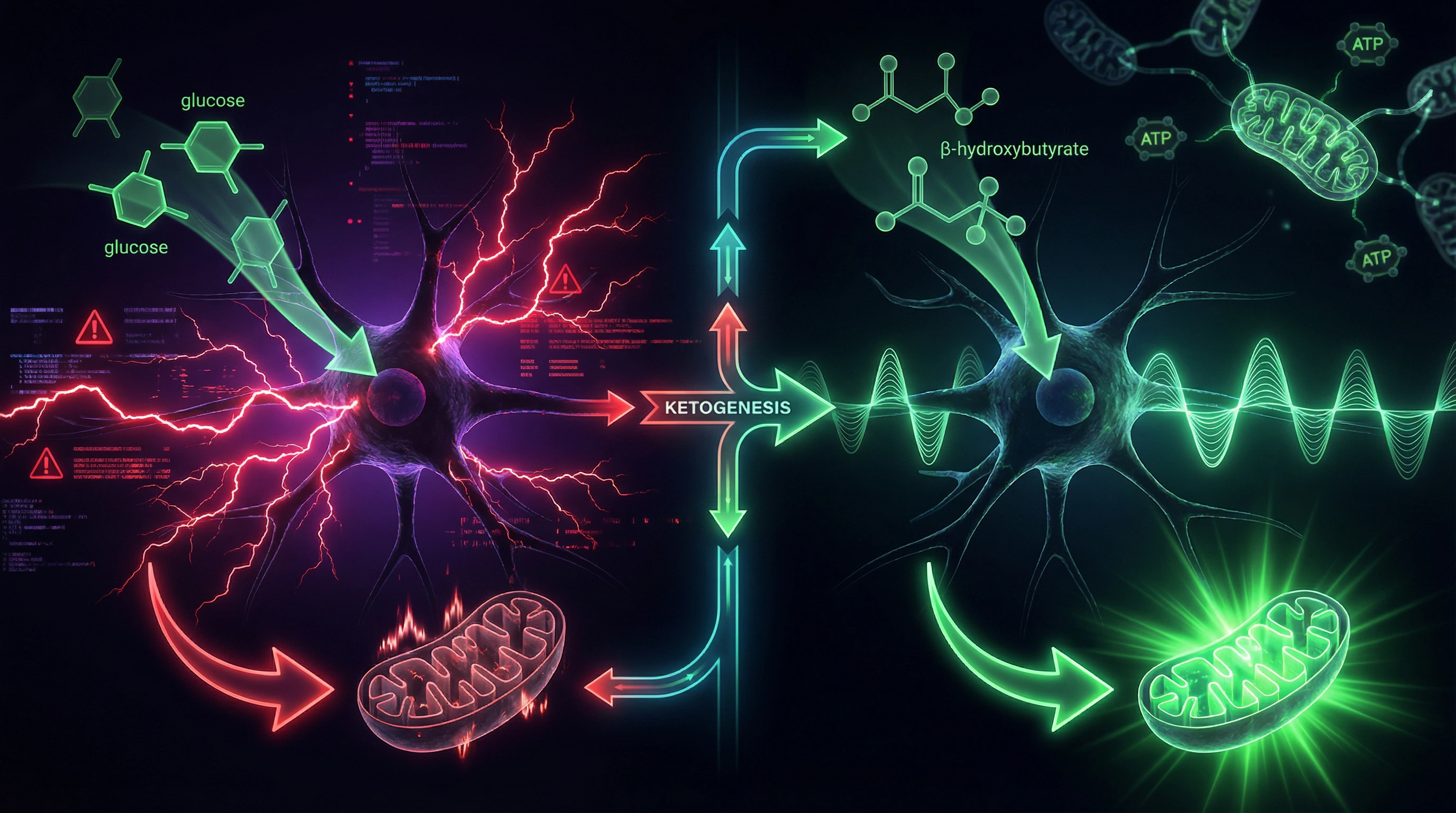
The goal of the ketogenic diet is to shift brain metabolism from glucose to ketone bodies. Under normal conditions, the brain uses glucose as its primary fuel.
With severe carbohydrate restriction, the liver begins breaking down fats and producing ketone bodies—beta-hydroxybutyrate, acetoacetate, and acetone. These molecules cross the blood-brain barrier and become an alternative energy source for neurons (S004).
- Ketosis
- Not a pathology, but an ancient metabolic survival mechanism activated during fasting. The ketogenic diet mimics the biochemistry of starvation, but without actual caloric deficit—the child receives sufficient energy for growth and development, but from fat rather than carbohydrates.
Drug-Resistant Epilepsy
The ketogenic diet is not a first-line therapy. It's prescribed for children with drug-resistant epilepsy—a condition where seizures continue despite adequate doses of two or more antiepileptic medications (S002).
Between 20% and 40% of children with epilepsy do not achieve seizure control with medications. For these children, the ketogenic diet becomes one of the few remaining options, aside from surgical intervention or vagus nerve stimulator implantation.
- In 50–60% of children on the ketogenic diet, seizure frequency decreases by more than 50% (S001)
- In 10–15%, seizures stop completely
- For families living in constant fear of the next seizure, this can mean the difference between a normal life and disability
Five Most Compelling Arguments for the Ketogenic Diet in Childhood Epilepsy
Before examining mechanisms and limitations, it's essential to honestly present the strongest arguments from proponents of this method. This is not a straw man for easy refutation, but serious clinical observations backed by decades of research. More details in the section Detox Myths.
🔬 First Argument: Clinical Efficacy in Specific Syndromes Surpasses Pharmacotherapy
For certain forms of epilepsy, the ketogenic diet demonstrates efficacy comparable to or exceeding medication treatment. Particularly impressive results are observed in Dravet syndrome, Lennox-Gastaut syndrome, infantile spasms, and glucose transporter type 1 deficiency (GLUT1) (S001).
In GLUT1 deficiency, a rare genetic disorder where glucose cannot cross the blood-brain barrier, the ketogenic diet is not merely effective but the only pathogenic treatment. Ketone bodies use different transporters and provide the brain with energy it cannot obtain from glucose. In this case, the diet is not an alternative to medication—it replaces a missing biochemical function.
For rare genetic forms of epilepsy, the ketogenic diet is not a choice between methods, but restoration of a disrupted metabolic pathway.
📊 Second Argument: Long-Term Safety Confirmed by Nearly a Century of Clinical Use
The ketogenic diet has been used to treat epilepsy since the 1920s, when physicians noticed that fasting reduced seizure frequency. Over nearly a century, enormous clinical experience has accumulated, allowing prediction and management of side effects (S002).
Unlike new antiepileptic drugs whose long-term effects may be unknown, the ketogenic diet has stood the test of time. Studies show that most side effects are reversible and manageable with proper medical supervision (S001).
- Long-Term Safety
- Children who maintained the diet for several years, in most cases, return to normal eating without long-term consequences.
- Manageable Side Effects
- A century of experience allows physicians to anticipate and control adverse reactions, unlike new drugs with unstudied profiles.
🧬 Third Argument: Efficacy in GRIN-Associated Epilepsy, Where Pharmacology Often Fails
GRIN-associated epilepsy is a group of severe epileptic encephalopathies caused by mutations in genes encoding NMDA receptor subunits. These forms of epilepsy are often resistant to standard antiepileptic drugs and accompanied by severe cognitive impairments.
Systematic review shows that the ketogenic diet can be effective where medication therapy fails. The mechanism is linked to modulation of NMDA receptor activity by ketone bodies, which reduces excitotoxicity and stabilizes neuronal membranes (S004). For families of children with these rare and severe forms of epilepsy, the ketogenic diet may be the only hope for improved quality of life.
🛡️ Fourth Argument: Absence of Cognitive Side Effects Characteristic of Many Anticonvulsants
Many antiepileptic drugs cause cognitive side effects—slowed thinking, memory problems, drowsiness, attention deficits. For the developing child's brain, these effects can be particularly devastating, affecting learning and social development (S002).
The ketogenic diet, by contrast, is often associated with improved cognitive function. Parents report increased attention, improved behavior, and accelerated development after starting the diet. It's hypothesized that stable brain energy supply from ketone bodies and reduced oxidative stress contribute to neuroprotection (S004).
Paradox: a restrictive diet often improves cognitive function where expanding the pharmacological arsenal impairs it.
⚙️ Fifth Argument: Possibility of Gradual Discontinuation with Sustained Effect in Some Patients
Unlike antiepileptic drugs, which often require lifelong use, the ketogenic diet can be gradually discontinued after 2–3 years of adherence. In a significant proportion of children (ranging from 20% to 40% by various estimates), seizure control persists even after returning to normal eating (S001).
This suggests that the ketogenic diet doesn't merely suppress symptoms but may modify disease progression, possibly through epigenetic mechanisms or long-term reorganization of neural networks (S002). For families, this means hope not for lifelong disease management, but for potential cure or at least prolonged remission.
| Characteristic | Antiepileptic Drugs | Ketogenic Diet |
|---|---|---|
| Duration of Use | Often lifelong | 2–3 years with possible discontinuation |
| Effect Persistence After Discontinuation | Rare | 20–40% of patients |
| Cognitive Side Effects | Frequent and significant | Absent or improvement |
| Clinical Experience | Variable by drug | Century of clinical experience |
Evidence Base: What Research from Central Asia and Global Literature Shows
From arguments to facts. Every claim about the ketogenic diet must be verified through the lens of available research—data quality, sample sizes, methodological limitations. More details in the Homeopathy section.
📊 Efficacy by the Numbers: What Clinical Studies Show
A study in the Bulletin of Kazakh National Medical University analyzes the use of the ketogenic diet in children with epilepsy in Central Asian settings. Results: 52% of children experienced a reduction in seizure frequency of more than 50%, 27% saw a reduction of more than 90%, and 13% achieved complete seizure freedom (S001).
These figures align with global data. Meta-analyses show a median seizure frequency reduction of 50–60% among responders, with approximately 10–15% of children achieving complete seizure freedom. Efficacy varies by epilepsy type: response rates are lower in focal forms compared to generalized epileptic encephalopathies (S002).
Most studies are retrospective observational or small prospective cohorts. Randomized controlled trials (RCTs) are relatively scarce: it's difficult to create placebo controls for dietary interventions, and parents of children with severe epilepsy are reluctant to agree to randomization.
🧪 Mechanisms of Action: From Lipid Membranes to Neurotransmitters
The precise mechanisms of antiepileptic action remain the subject of active research. Several competing and complementary hypotheses exist.
- Neuronal Membrane Stabilization
- Ketone bodies, particularly beta-hydroxybutyrate, integrate into membrane structures, altering their fluidity and ion channel function. This raises the threshold for seizure activity (S004).
- Neurotransmitter Modulation
- The ketogenic diet increases synthesis of GABA (the primary inhibitory neurotransmitter) and reduces glutamate levels (the primary excitatory neurotransmitter). The balance shifts toward inhibition, counteracting hyperexcitability (S001).
- Energy Metabolism
- Ketone bodies are more efficient fuel for mitochondria than glucose: they produce more ATP with less generation of reactive oxygen species. This improves neuronal energy status and reduces oxidative stress, which plays a role in epileptogenesis (S004).
- Epigenetic Regulation
- Beta-hydroxybutyrate inhibits histone deacetylases (HDACs), altering histone acetylation patterns and modulating transcription of genes associated with neuroprotection and inflammation.
🧬 GRIN-Associated Epilepsy: Molecular Mechanism
GRIN genes encode subunits of NMDA receptors—ionotropic glutamate receptors critical for synaptic plasticity. Mutations lead to both gain-of-function and loss-of-function effects, but in both cases the result is epileptic encephalopathy (S001).
Ketone bodies modulate NMDA receptor activity, reducing excessive activation in gain-of-function mutations. The mechanism may involve direct interaction with the receptor or mediated influence through changes in membrane potential.
| Parameter | Observation |
|---|---|
| Seizure Frequency | Reduction in most patients |
| Cognitive Function | Improvement in behavior and learning |
| Level of Impact | On symptoms and underlying pathophysiology |
🧾 Side Effects and Complications: The Cost of Therapy
The ketogenic diet is not a safe intervention in the conventional sense. It carries a range of side effects, some of which are serious and require medical intervention (S001).
- Gastrointestinal Disorders: constipation (30–50% of children), diarrhea, nausea, vomiting, gastroesophageal reflux. Usually occur at diet initiation, manageable through fat adjustment, fiber addition, and laxatives.
- Nephrolithiasis (Kidney Stones): develops in 3–7% of children. Associated with increased calcium and uric acid excretion, changes in urine pH. Prevention: adequate hydration and citrate supplementation.
- Dyslipidemia: elevated cholesterol and triglycerides in 10–30% of children. Requires lipid profile monitoring and modification of fat types.
- Growth Retardation and Micronutrient Deficiency: children require careful growth monitoring and mandatory vitamin-mineral supplementation. Deficiencies in selenium, carnitine, vitamin D, and calcium are particularly common.
- Rare Complications: pancreatitis, cardiomyopathy (selenium or carnitine deficiency), hepatopathy, osteoporosis. Require regular monitoring: biochemical tests, ECG, bone densitometry, kidney ultrasound.
These complications underscore the necessity of regular medical supervision. The ketogenic diet is not a home experiment, but a medical intervention requiring protocol-based monitoring and adjustment.
Causal Relationships and Mechanistic Understanding: Correlation Does Not Equal Causation
Improvement after starting a diet does not mean the diet is the cause. This is a basic logical fallacy that permeates all of popular medicine. More details in the section Debunking and Prebunking.
Epilepsy follows a wave-like pattern: periods of exacerbation alternate with remissions. Parents typically start the diet at the peak of seizures—when the situation is critical. Then natural improvement occurs, which is attributed to the diet (S002).
This is regression to the mean—a statistical artifact, not proof of effect. Without a control group, it's impossible to distinguish it from the diet's actual action.
🔁 Natural Course and Randomization
Most ketogenic diet studies are open cohort studies. All participants receive the intervention, there is no control group. This makes it impossible to separate the diet's effect from the natural course of the disease (S002).
Randomized controlled trials require an ethically complex decision: giving one group of children the diet and another group none. Therefore, there are few of them, and most evidence remains low quality.
🧷 Confounders: What Else Changes Simultaneously
When a child starts the ketogenic diet, many other changes occur simultaneously:
- Changes in antiepileptic therapy—adding medications, changing doses, discontinuing ineffective ones (S001)
- Intensive medical monitoring—regular visits, laboratory tests, monitoring
- Increased family attention to the child's health and lifestyle
- Psychological effect—hope for recovery, improved treatment adherence
Separating the diet's effect from the effect of medications and monitoring in observational studies is practically impossible (S001).
The "observation effect" itself can improve outcomes through better treatment adherence, early problem detection, and psychological support for the family.
🧬 Genetic Heterogeneity: Why One Diet Doesn't Work for Everyone
Epilepsy is not a single disease, but a group of hundreds of different syndromes. Each has its own genetic, structural, or metabolic causes.
| Type of Epilepsy | Mechanism | Expected Response to Keto |
|---|---|---|
| Genetic (ion channel mutation) | Protein-level defect | Unpredictable |
| Structural (scar, tumor) | Physical brain damage | Low, unless surgical treatment |
| Metabolic (metabolic defect) | Cellular energy disruption | High, if diet addresses defect |
| Idiopathic (unknown cause) | Unclear | Variable |
Assuming that one dietary intervention will be equally effective for all forms is biologically implausible. It's like giving one antibiotic for all infections.
The ketogenic diet may work for certain metabolic forms of epilepsy (S004), but for other syndromes the effect is minimal or absent. Studies often mix these groups, creating an illusion of universal effectiveness.
- Selection bias
- Published studies mainly include cases with good response to the diet. Cases without effect are often not published or remain in clinic archives. This distorts the perception of true effectiveness.
Mechanistic understanding requires not just correlation, but proof that the diet acts through a known biological pathway, and that this pathway is disrupted specifically in that patient. Without this—only a statistical artifact.
Counter-Position Analysis
⚖️ Critical Counterpoint
The ketogenic diet for epilepsy is one of the few non-pharmacological methods with an evidence base, but its effectiveness and safety have limitations. Here's where the article may underestimate risks or overestimate the universality of the approach.
Geographic Limitation of Data
The primary sources are from Central Asia (Kazakhstan, Russia). This creates a risk of regional bias: protocols, effectiveness, and side effects may vary depending on population, access to medical supervision, and cultural factors. Western meta-analyses (Cochrane, for example) may show different effectiveness figures.
Insufficient Long-Term Outcome Data
The article relies on clinical protocols and reviews, but there are few large prospective studies with 10–20 years of follow-up for children on the ketogenic diet. It's unknown how strict carbohydrate restriction during critical developmental periods affects cognitive function, metabolic health, and quality of life in adulthood.
Theoretical Mechanisms vs. Clinical Practice
The membrane contamination hypothesis is presented as one of the models, but the mechanisms of action of the ketogenic diet are not fully understood. The effect may be related not to ketosis per se, but to other factors: calorie restriction, microbiome changes, anti-inflammatory effects. If the mechanism is misunderstood, this calls into question the optimality of the protocol.
Risk of Overestimating Effectiveness
Systematic reviews on specific genetic forms of epilepsy may show high effectiveness in narrow subgroups, but this doesn't mean universal applicability. Publication bias (positive results are published more often) may inflate the effect estimate.
Alternative Explanations for Improvement
Part of the effect may be related not to the diet, but to intensive medical monitoring, placebo effect in parents (subjective assessment of seizure frequency), natural variability in the course of epilepsy. Controlled blinded studies are difficult in dietetics, which reduces confidence in the causal relationship.
FAQ
Frequently Asked Questions
