 🥬 Extreme Diets and Miracle Cures
🥬 Extreme Diets and Miracle CuresExtreme Diets: Scientific Evidence on Effectiveness and Risksλ
Systematic analysis of extreme weight loss diets: from low-carb to intermittent fasting, their metabolic consequences and long-term safety
Overview
Extreme diets promise rapid weight loss through radical restrictions of macronutrients or calories, but scientific evidence reveals serious problems with their long-term effectiveness and safety. Systematic reviews and meta-analyses from 2005–2024 identify: very low-carbohydrate and very low-fat diets often lead to rebound effects — weight regain exceeding baseline — due to metabolic adaptation. Epidemiological data demonstrate a U-shaped mortality curve — both very high and very low carbohydrate intake are associated with increased risk, indicating the optimality of a moderate approach.
🛡️
Laplace Protocol: Extreme restrictions trigger physiological defense mechanisms that undermine long-term weight maintenance. Moderate, balanced dietary changes outperform radical approaches in safety and sustainability of results.
Reference Protocol
Scientific Foundation
Evidence-based framework for critical analysis
Navigation Matrix
Subsections
[extreme-diets-cures]
Extreme Diets and Miracle Cures
Scientific evidence on the risks of crash diets, mono-diets, and fasting: from muscle loss to serious metabolic disorders
Explore
[fasting-panacea]
Fasting as a Panacea
Scientific analysis of evidence on intermittent fasting effectiveness for health, metabolism, and longevity compared to traditional calorie restriction
Explore
Protocol: Evaluation
Test Yourself
Quizzes on this topic coming soon
Sector L1
Articles
Research materials, essays, and deep dives into critical thinking mechanisms.
 🥬 Extreme Diets and Miracle Cures
🥬 Extreme Diets and Miracle Cures 🥬 Extreme Diets and Miracle Cures
🥬 Extreme Diets and Miracle Cures 🥬 Extreme Diets and Miracle Cures
🥬 Extreme Diets and Miracle Cures ⏰ Fasting as a Panacea
⏰ Fasting as a Panacea⚡
Deep Dive
What Lies Behind Extreme Diet Promises: A Typology of Radical Approaches
Extreme diets are eating regimens with radical restrictions of macronutrients or calories, promising rapid weight loss while ignoring long-term consequences. They're characterized by deviations of 40% or more from recommended protein, fat, and carbohydrate ratios, creating metabolic stress.
The scientific community defines them as eating patterns that are difficult to maintain long-term and carry risks of nutritional imbalance. Their appeal mechanism is simple: radical restriction = quick results in the first weeks, creating an illusion of effectiveness.
- Metabolic Stress
- A state where the body experiences extreme deviation from normal nutritional conditions, triggering protective mechanisms and adaptation. This isn't just calorie deficit—it's a danger signal to your physiology.
- Nutritional Imbalance
- Deficiency or excess of specific macro- and micronutrients, disrupting hormonal regulation, immunity, and long-term health. Often hidden behind short-term results.
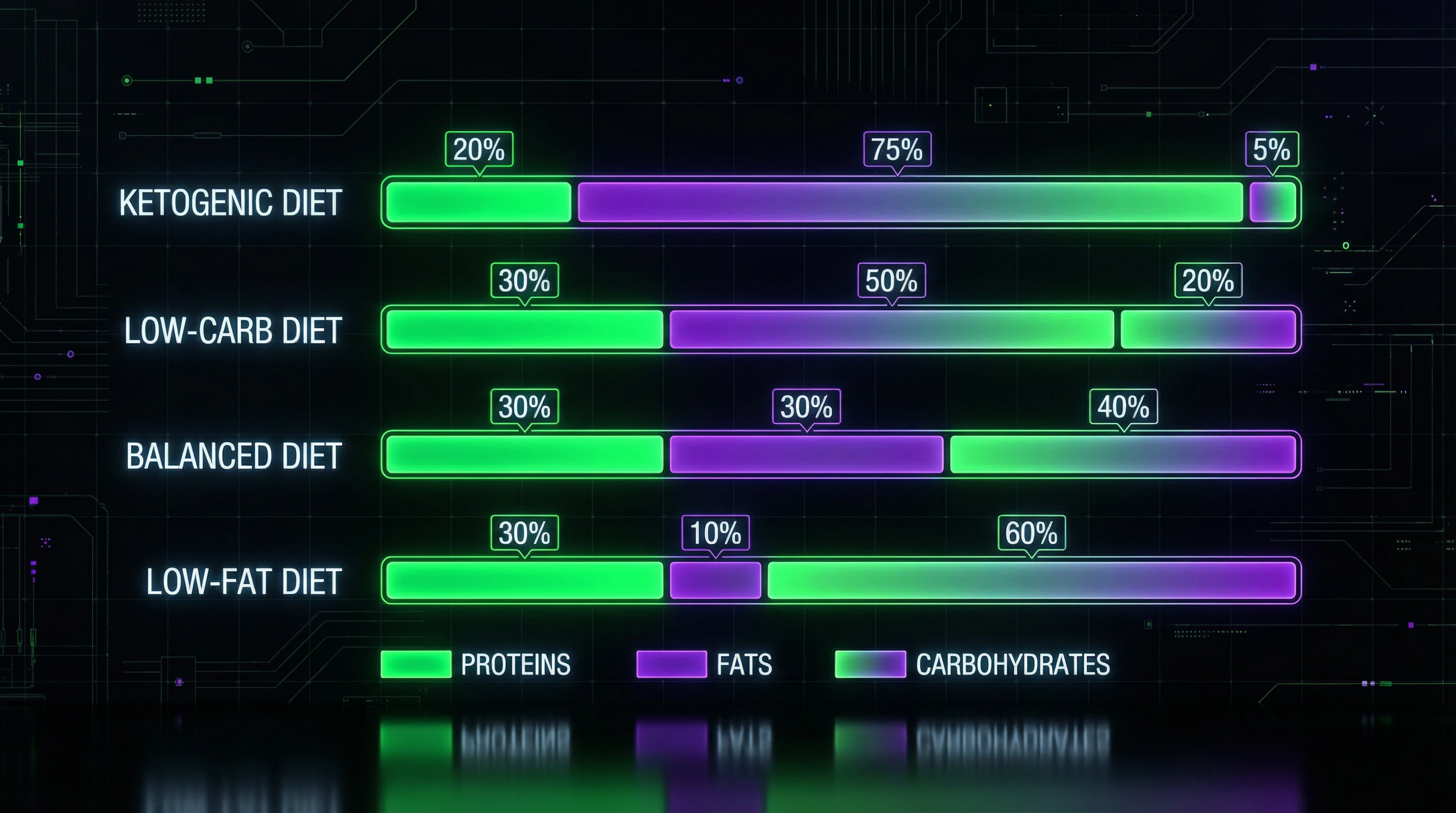
Very Low-Carbohydrate Diets: The Ketogenic Approach and Its Variations
The ketogenic diet and Atkins diet restrict carbohydrates to 20–50 grams per day, forcing the body to switch to fat metabolism and ketone body production. The metabolic shift occurs within 2–4 days, when glycogen stores are depleted and the liver actively breaks down fats.
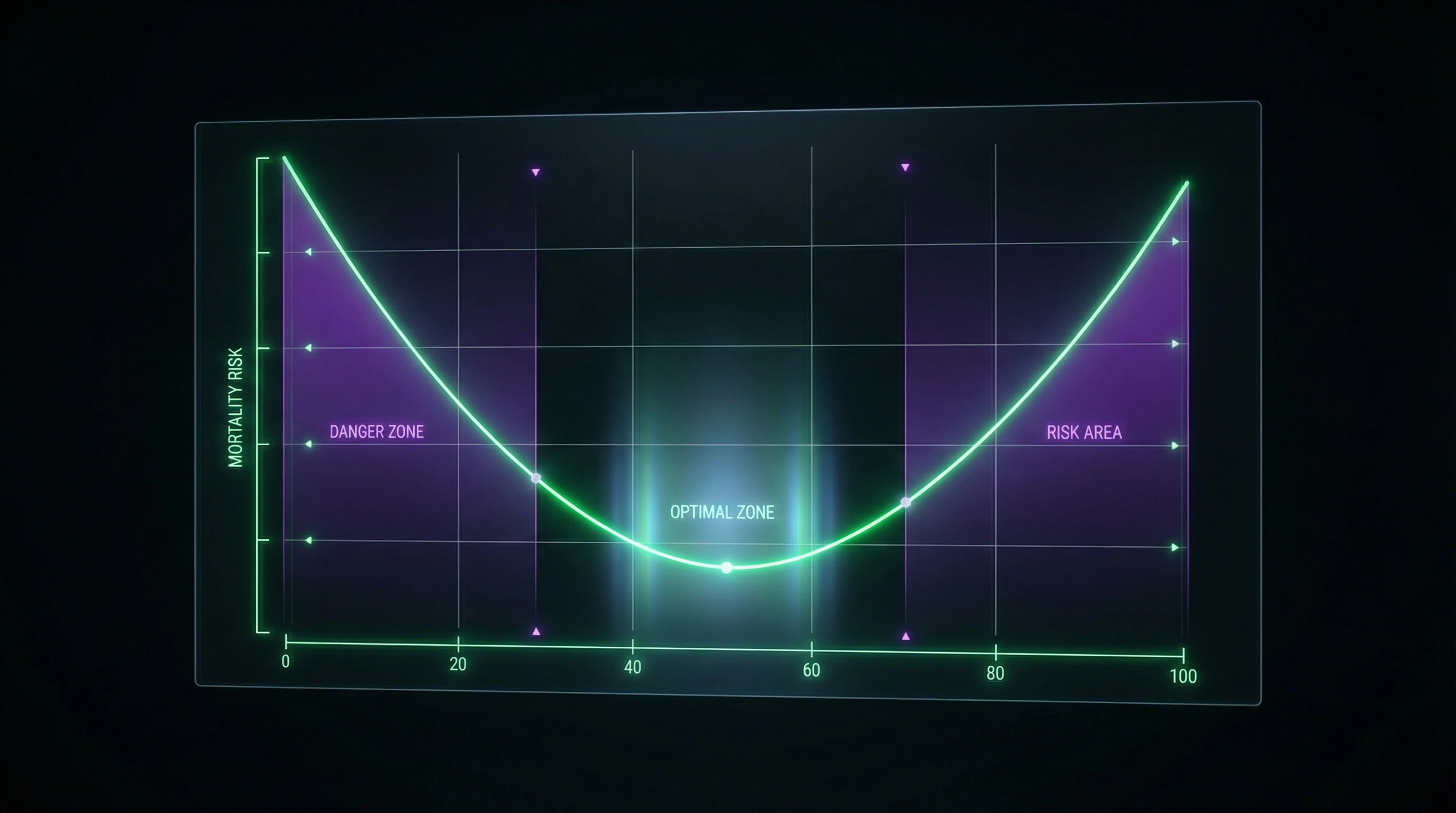
Long-term epidemiological data shows a U-shaped mortality curve: both very low and very high carbohydrate intake are associated with increased risk of premature death.
The ARIC study with over 15,000 participants found that optimal carbohydrate intake is 50–55% of total calories, while reducing below 40% increases long-term mortality by 20%.
Very Low-Fat Diets: The Opposite Pole of Restriction
Diets with fat content below 10–15% of calories (Ornish diet, some vegan protocols) restrict all fat sources, including plant oils and nuts. Such regimens lead to deficiency of fat-soluble vitamins A, D, E, K and essential fatty acids, affecting hormonal balance and nutrient absorption.
| Parameter | Very Low-Carb | Very Low-Fat |
|---|---|---|
| Adherence at 12 months | ~35–40% | ~30% |
| Micronutrient deficiency risk | B vitamins, minerals | Fat-soluble vitamins, omega-3 |
| Paradoxical effect | May increase triglycerides | May lower HDL, increase triglycerides |
Clinical trials show adherence drops to 30% at 12 months due to the restrictive nature and social difficulties.
Intermittent Fasting and Extreme Caloric Restriction
Intermittent fasting ranges from 16-hour fasting windows to protocols with 500–600 calories on "fasting" days. Extreme variants with calorie intake below 800 kcal/day (VLCD) are used in clinical practice under medical supervision, but their independent application carries risks.
- 15–20% reduction in basal metabolic rate—the body conserves energy
- Increased ghrelin (hunger hormone) and decreased leptin (satiety hormone)—amplified appetite
- Prolonged fasting beyond 24 hours activates muscle tissue catabolism—slowed metabolism and worsened body composition
These protective mechanisms aren't weakness of will, but physiological reality. The body perceives extreme restriction as a survival threat and activates conservation mode.
The Illusion of Quick Results: What Happens in the First Weeks of Restriction
The dramatic weight loss in the first 1–2 weeks of an extreme diet creates a powerful psychological effect, but most of this loss is not fat tissue. Understanding the mechanisms of the initial phase is critical for realistic expectations and preventing disappointment when progress slows.
Initial Water Loss and Glycogen Depletion
Each gram of glycogen in muscles and liver is bound to 3–4 grams of water, so depleting 400–500 grams of glycogen leads to a loss of 1.5–2 kg of weight in the first 48–72 hours.
On low-carb diets, this effect is amplified: reduced insulin regulates sodium retention in the kidneys, resulting in an additional loss of 1–2 liters of fluid. Studies show that up to 70% of weight lost in the first week of a ketogenic diet is water and glycogen, not fat tissue.
Returning to normal eating immediately restores 2–3 kg of "lost" weight — this is simply replenishment of physiological stores, not failure of results.
Metabolic Changes in the First Weeks: Adaptation or Stress
Within 7–14 days of strict calorie restriction, the body shifts into "energy conservation" mode, reducing thermogenesis (heat production) by 10–15%.
- The thyroid gland decreases production of active T3 hormone, slowing metabolism at the cellular level — a protective response to perceived starvation.
- Cortisol rises, a catabolic hormone that promotes muscle loss and water retention, masking actual fat loss on the scale.
- Insulin sensitivity temporarily improves and inflammation decreases, creating a subjective feeling of "lightness" and energy that doesn't persist long-term.
The paradox of the first weeks: the body simultaneously loses water and muscle, conserves energy, and elevates stress hormones — this isn't success, it's mobilization of defenses.
Why Weight Returns: The Physiology of Rebound and the Metabolic Trap
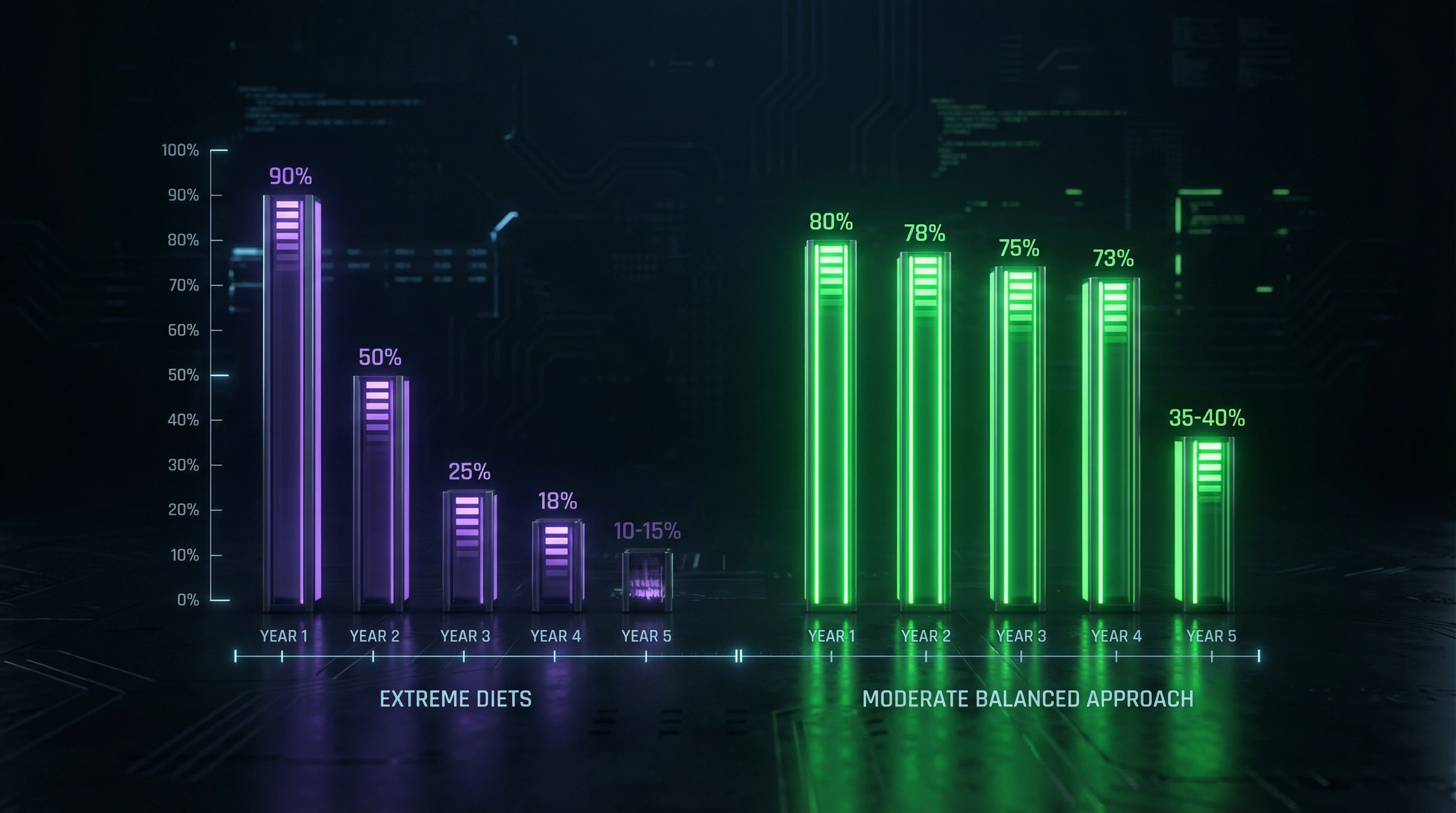
The phenomenon of weight regain after extreme diets is not a result of "weak willpower," but a predictable physiological response to prolonged restriction. Studies show that 80–95% of people who lost significant weight on extreme diets regain it within 1–5 years, with 30–40% gaining more than they lost.
Physiological Defense Mechanisms: The Body Against the Diet
Evolutionarily hardwired mechanisms protecting against starvation include a reduction in basal metabolism of 20–25% below what's predicted for the new weight — a phenomenon known as metabolic adaptation.
A study of participants from "The Biggest Loser" showed that 6 years after extreme weight loss, their metabolism remained 500 kcal/day below expected, requiring constant undereating to maintain results.
The body increases the efficiency of calorie absorption from food, activates lipoprotein lipase (a fat-storing enzyme), and reduces spontaneous physical activity by 15–30%. These changes persist for years after stopping the diet, creating a biological predisposition to weight regain.
Hormonal Changes: Hunger Defeats Willpower
Ghrelin, the "hunger hormone," increases 20–30% above baseline after significant weight loss and remains elevated for at least a year. Simultaneously, leptin, which signals the brain about adequate energy stores, drops 40–50%, creating a constant sensation of hunger even with adequate nutrition.
- Peptide YY and cholecystokinin (satiety hormones) decrease, shortening the period of fullness after meals.
- Neuroimaging shows enhanced brain response to food images, especially high-calorie foods.
- Reward centers activate while prefrontal control is suppressed.
Statistics of Failure: Numbers They Don't Advertise
A meta-analysis of 29 long-term diet studies showed that after 4–5 years, the average participant maintains only 3–4 kg of the initially lost 10–15 kg. Extreme diets demonstrate the worst weight maintenance outcomes: adherence drops to 10–20% after 2 years.
| Indicator | Value | Consequence |
|---|---|---|
| Yo-yo effect | Cycles of weight loss and gain | Cardiovascular disease risk +40%, mortality +60% |
| Cumulative adaptation | Each diet cycle | Subsequent weight loss becomes more difficult |
| Muscle mass loss | With extreme restrictions | Reduced metabolism, accelerated fat gain |
A study of 14,000 people following various popular diets found that the yo-yo effect is associated with a 40% increased risk of cardiovascular disease and 60% increased mortality compared to stable weight.
U-Shaped Mortality Curve and Long-Term Risks of Extreme Diets
The ARIC (Atherosclerosis Risk in Communities) study of 15,428 participants over 25 years revealed a U-shaped relationship: lowest mortality risk at 50–55% of calories from carbohydrates, with a 20–30% increase at both very low (<40%) and very high (>70%) intake levels. A meta-analysis of eight cohort studies (432,179 people) confirmed: extreme restriction of any macronutrient increases long-term risks.
Epidemiological Data: What Large Samples Show
Participants with carbohydrate intake below 40% had an 18% higher risk of all-cause mortality. Replacing carbohydrates with animal proteins and fats increased mortality risk by 23%, while plant-based sources showed no negative effect.
The European EPIC study (521,448 people) found: extremely low-fat diets (<15% of calories) are associated with a 34% increased risk of hemorrhagic stroke in women. A Japanese cohort study showed that weight fluctuations exceeding 5 kg over 5 years increase cardiovascular event risk by 40%—a typical pattern of cyclical extreme dieting.
It's not weight loss itself that's dangerous, but its volatility. The body experiences extreme restriction as stress, and each cycle amplifies metabolic maladaptation.
Optimal Ranges: Where the Line Between Effectiveness and Risk Lies
A 2023 systematic review identified optimal ranges for long-term health: carbohydrates 45–65%, fats 20–35%, proteins 10–35% of caloric intake. The study showed that macronutrient ratios affect metabolic health independently of weight loss.
| Parameter | Optimal Range | Risk with >10% Deviation |
|---|---|---|
| Carbohydrates | 45–65% | Increased inflammation, impaired glycemic control |
| Fats | 20–35% | Dyslipidemia, impaired absorption of fat-soluble vitamins |
| Proteins | 10–35% | Impaired protein synthesis, muscle loss or kidney overload |
Moderately low-carbohydrate diets (40–45% carbohydrates) improved insulin sensitivity by 28% without extreme restrictions. Clinical trials showed: deviation from these ranges correlates with worsening biomarkers—elevated inflammatory markers, dyslipidemia, and impaired glycemic control.
Individual variability in metabolic response requires personalization within these ranges, but exceeding their boundaries is rarely justified from a risk–benefit perspective.
Compliance Issues and Psychological Aspects of Extreme Diets
Only 15% of participants adhered to an extremely low-fat diet (<10% fat) for 12 months, compared to 58% on a moderately low-fat diet. Compliance with extreme diets drops exponentially: 60% at 3 months, 30% at 6 months, less than 10% at 2 years.
Primary reasons for discontinuation: social isolation (73%), constant hunger (68%), psychological exhaustion from rigid restrictions (61%).
Extreme approaches have a dropout rate of 45–60% within the first year—2–3 times higher than balanced diets. Diet quality and adherence are more important than the degree of macronutrient restriction.
The DIETFITS study (609 participants) showed: participants with high compliance to moderate diets lost more weight than those who periodically followed extreme protocols. Every 10% decrease in adherence to an extreme diet is associated with regaining 2.3 kg of lost weight within 6 months.
Psychological Dynamics and Neurobiology
Extreme diets trigger a cycle of psychological dependence: initial euphoria from rapid results gives way to anxiety at the slightest deviation, leading to even more rigid restrictions. Among 87 individuals practicing extreme diets, 64% developed signs of orthorexia—an obsessive preoccupation with "correct" eating that negatively impacts quality of life.
Neuroimaging studies demonstrate: prolonged extreme restrictions alter prefrontal cortex and limbic system activity, amplifying responses to food stimuli and reducing cognitive control. This creates a neurobiological foundation for lapses.
Eating Disorders as an Outcome
- Risk of Developing Eating Disorders
- People practicing extreme diets have a 5-fold higher risk of developing clinically significant eating disorders within 3 years compared to those following moderate approaches.
- Vulnerable Groups
- Adolescents and young adults are particularly susceptible. Among 2,516 participants aged 15–23 who practiced extreme restrictions, 18% developed bulimia or binge eating disorder within 5 years.
- Mechanism of Disruption
- Extreme diets disrupt natural hunger and satiety signals, creating dichotomous "all-or-nothing" thinking—a key risk factor for eating disorders.
Evidence-Based Alternatives: Moderate Approaches to Weight Loss
A systematic review of 121 randomized controlled trials showed that moderate balanced diets with a 500–750 calorie/day deficit provide sustainable weight loss of 0.5–1 kg per week with results maintained by 35–40% of participants after 5 years.
The Mediterranean diet with moderate calorie restriction demonstrated not only effectiveness (average 8.4 kg over one year), but also improvement in cardiometabolic markers and a 25% reduction in overall mortality in long-term observations.
Diet quality — emphasis on whole foods, vegetables, fruits, and minimally processed foods — is more important than specific macronutrient ratios for long-term success.
Comparative Effectiveness of Balanced Diets
The PREDIMED-Plus study with 6,874 participants showed that an energy-restricted Mediterranean diet combined with physical activity led to a loss of 3.2 kg after one year and 2.1 kg after 3 years with a simultaneous 30% reduction in cardiovascular events.
A meta-analysis of 53 studies found that moderately-low-carbohydrate diets (40–45% carbohydrates) and moderately-low-fat diets (25–30% fat) show comparable effectiveness with significantly better adherence than their extreme variants.
| Approach | Weight Loss (Year 1) | Maintenance (5 Years) | Adherence |
|---|---|---|---|
| Moderate deficit 500–750 calories | 0.5–1 kg/week | 35–40% | High |
| Mediterranean (moderate) | 8.4 kg | Stable | High |
| Moderately-low-carbohydrate | Comparable | Comparable | Higher than extreme |
Individualization of Macronutrient Ratios
The Angelidi et al. (2026) study demonstrated significant individual variability in metabolic response to different macronutrient ratios.
Genetic factors, such as polymorphisms in the FTO and TCF7L2 genes, can modulate response to carbohydrates, but even in genetically predisposed individuals, extreme restrictions showed no advantages over moderate approaches.
- Start with baseline ratios: 50% carbohydrates, 30% fat, 20% protein
- Adjust within ±10% based on individual response
- Consider preferences and metabolic markers
- Avoid extreme restrictions even with genetic predisposition
Clinical Recommendations for Sustainable Weight Loss
A consensus statement from the American Association of Clinical Endocrinologists (2024) recommends gradual weight loss of 0.5–1 kg per week through moderate caloric deficit and balanced nutrition within recommended macronutrient ranges.
The combination of a moderate dietary approach with behavioral therapy and regular physical activity provides the best long-term results: average weight loss of 7–10% from baseline with maintenance by 40% of participants after 5 years.
- Gradual Changes
- Weight loss of 0.5–1 kg per week, without drastic restrictions that trigger relapses and metabolic adaptation.
- Focus on Diet Quality
- Whole foods, vegetables, fruits, minimally processed foods — the foundation, not calorie counting as an end in itself.
- Regular Monitoring Without Obsession
- Tracking progress without obsessive control, which increases anxiety and disrupts eating behavior.
- Stress Management and Emotional Eating
- Developing coping skills without resorting to extreme restrictions as a means of control.
Knowledge Access Protocol
FAQ
Frequently Asked Questions
Extreme diets are eating patterns with severe restrictions on macronutrients or calories, such as keto, Atkins, or very low-fat diets. They promise rapid results but are difficult to maintain long-term and create risks of nutrient deficiencies. Regular diets involve moderate changes and a balanced approach (Joshi et al., 2018).
The body activates protective mechanisms: it slows metabolism, alters hunger and satiety hormone levels, which triggers overeating. Many people regain more weight than they lost—this is called the rebound phenomenon. Metabolic adaptation makes maintaining results extremely difficult (Ubie Health, 2025).
Moderate carbohydrate reduction can be safe, but extreme variants (less than 50g/day) are associated with increased mortality according to cohort studies. A U-shaped curve shows that both very low and very high carbohydrate intake levels are dangerous. The optimal range is 50-55% of calories from carbohydrates (ARIC, 2018).
No, this is a myth. Extreme diets provide a quick start through water and glycogen loss, but long-term they don't outperform balanced approaches. Low compliance and weight rebound negate initial results. Moderate changes produce sustainable effects without risks (Joshi et al., 2018).
Severe calorie restriction slows basal metabolic rate—the body shifts into energy conservation mode. Secretion of leptin, ghrelin, and other hormones changes, intensifying hunger. These adaptations persist for months after the diet ends, making weight maintenance difficult (Elsevier, 2024).
Clinical data show extremely low long-term compliance—most people break within 6-12 months. Strict restrictions cause psychological discomfort, social isolation, and nutrient deficiencies. Sustainability is the main problem with extreme approaches (Schaefer, 2005).
This is the relationship between mortality risk and the proportion of carbohydrates in the diet: both very low (less than 40%) and very high (more than 70%) intake increase mortality. Minimum risk occurs with moderate intake of 50-55% of calories from carbohydrates. Data obtained from 15 years of observation of 15,000 people (ARIC, 2018).
Fat deficiency impairs absorption of fat-soluble vitamins (A, D, E, K), disrupts hormonal balance, and worsens skin condition. Extremely low fat intake (less than 10% of calories) is associated with increased mortality. The optimum is 25-35% of calories from fats (Joshi et al., 2018).
Create a moderate deficit of 300-500 calories/day while maintaining balance of proteins, fats, and carbohydrates. Include all food groups, increase vegetables and whole grains, add regular physical activity. Gradual loss of 1-2 lbs/week is sustainable and safe (Fang et al., 2023).
It depends on the protocol. Moderate variants (16/8) are relatively safe for healthy individuals, but prolonged fasting (more than 24 hours) or very low calories can trigger the same protective mechanisms as extreme diets. Individual tolerance and medical supervision are important (Elsevier, 2024).
It's mostly water and glycogen, not fat. With a sharp reduction in carbohydrates, the body uses up glycogen stores (1 g binds 3-4 g of water), which produces rapid weight loss on the scale. Fat mass loss begins later and proceeds more slowly (Angelidi et al., 2026).
Yes, strict restrictions increase the risk of developing orthorexia, binge eating disorder, and other eating disorders. The "restriction-binge" cycle creates an unhealthy relationship with food and feelings of guilt. Psychological support is important with any significant dietary changes (Schaefer, 2005).
This is a dangerous myth. Epidemiological and clinical data show that extreme approaches produce worse long-term outcomes due to weight rebound and health risks. Moderate changes are more effective, safer, and more sustainable. "More" doesn't mean "better" in nutrition (ARIC, 2018).
Essential: complete blood count and comprehensive metabolic panel, lipid profile, glucose, thyroid hormones, vitamins D and B12. Consultation with an endocrinologist and dietitian is advisable to assess risks. Regular monitoring is necessary if continuing strict restrictions (Joshi et al., 2018).
Yes: pregnant and breastfeeding women, children and adolescents, elderly people, patients with diabetes, kidney disease, liver disease, or heart conditions. For them, extreme restrictions can cause serious complications. Any significant dietary changes require medical approval (Ruden, 2007).
Check whether it: promises quick results, excludes entire food groups, requires purchasing special supplements, is based on actual research. Scientific approaches are moderate, individualized, and don't promise miracles. Look for recommendations from professional medical organizations (Fang et al., 2023).
