 📡 Bioresonance Therapy
📡 Bioresonance TherapyHealth Technology Assessment: Devices and Diagnosticsλ
Specialized methodologies for assessing clinical and economic value of medical devices and diagnostic technologies for regulatory decisions and reimbursement
Overview
Medical devices and diagnostics require different evaluation methods than pharmaceuticals: iterative innovations, operator learning curves, procedural dependencies, and small sample sizes create methodological challenges for systematic reviews and clinical validation. Regulatory requirements FDA 510(k)/PMA, NICE technology appraisals, and HTA jurisdictions shape the evidence landscape — 🧩 clinical effectiveness is complemented by health economic analysis and demonstration of real-world value for healthcare systems.
🛡️
Laplace Protocol: Specialized HTA frameworks for devices and diagnostics account for unique technology characteristics, ensuring adequate value assessment with smaller evidence volumes and dynamic technological evolution.
Reference Protocol
Scientific Foundation
Evidence-based framework for critical analysis
Navigation Matrix
Subsections
[bioresonance]
Bioresonance Therapy
Comprehensive evaluation of bioresonance therapy based on systematic reviews, clinical studies, and scientific consensus on methodological limitations
Explore
[fake-diagnostics]
Misdiagnosis
Fake diagnostics are deceptive medical practices that use unscientific methods, unnecessary procedures, and fraudulent equipment to exploit patients and extract profit.
Explore
Protocol: Evaluation
Test Yourself
Quizzes on this topic coming soon
Sector L1
Articles
Research materials, essays, and deep dives into critical thinking mechanisms.
 📡 Bioresonance Therapy
📡 Bioresonance Therapy 📡 Bioresonance Therapy
📡 Bioresonance Therapy 📡 Bioresonance Therapy
📡 Bioresonance Therapy 📡 Bioresonance Therapy
📡 Bioresonance Therapy 🔍 Misdiagnosis
🔍 Misdiagnosis 🔍 Misdiagnosis
🔍 Misdiagnosis⚡
Deep Dive
HTA Specificity for Medical Devices: Why Pharmaceutical Methods Don't Work Here
Health Technology Assessment (HTA) for devices and diagnostics requires fundamentally different approaches than pharmaceutical drugs. Medical devices are subject to iterative improvements, depend on operator skills, and demonstrate learning curve effects—factors absent in drug evaluation.
Regulatory bodies, including NICE committees, explicitly recognize the need for specialized evaluation criteria for devices that account for their unique characteristics.
Differences from Pharmaceutical Technology Assessment
Traditional HTA frameworks developed for pharmaceuticals do not account for the procedural dependence of devices. Outcomes are determined not only by the technology itself but also by the qualifications of medical personnel, creating significant variability in clinical outcomes.
| Parameter | Pharmaceutical Drugs | Medical Devices |
|---|---|---|
| Outcome Variability | Minimal (patient-dependent) | High (operator and technique-dependent) |
| Study Sample Sizes | Large, standardized | Often smaller, heterogeneous |
| Learning Curve | Absent | Critical for data interpretation |
| Iterative Improvements | Rare in lifecycle | Continuous, require reassessment |
Systematic literature reviews for devices face smaller sample sizes, intervention heterogeneity, and operator-dependent outcomes—problems uncharacteristic of pharmaceutical research.
- Economic Evaluation of Devices
- Requires specific approaches: budget impact analysis and cost-effectiveness evaluation become critical for reimbursement decisions, with requirements for economic evidence increasing across various jurisdictions.
Iterative Innovation and Operator Learning Curves
Medical devices undergo continuous iterative improvements throughout the product lifecycle. By the time an assessment is completed, the technology may have already changed, creating a unique challenge for HTA.
The learning curve effect means that clinical outcomes improve as medical personnel accumulate experience using the device, complicating the interpretation of early clinical data.
- Adaptive evaluation methodologies must account for the evolution of both technology and operator skills
- Healthcare innovations demonstrate value through clinical effectiveness, economic impact, and real-world effectiveness in practice
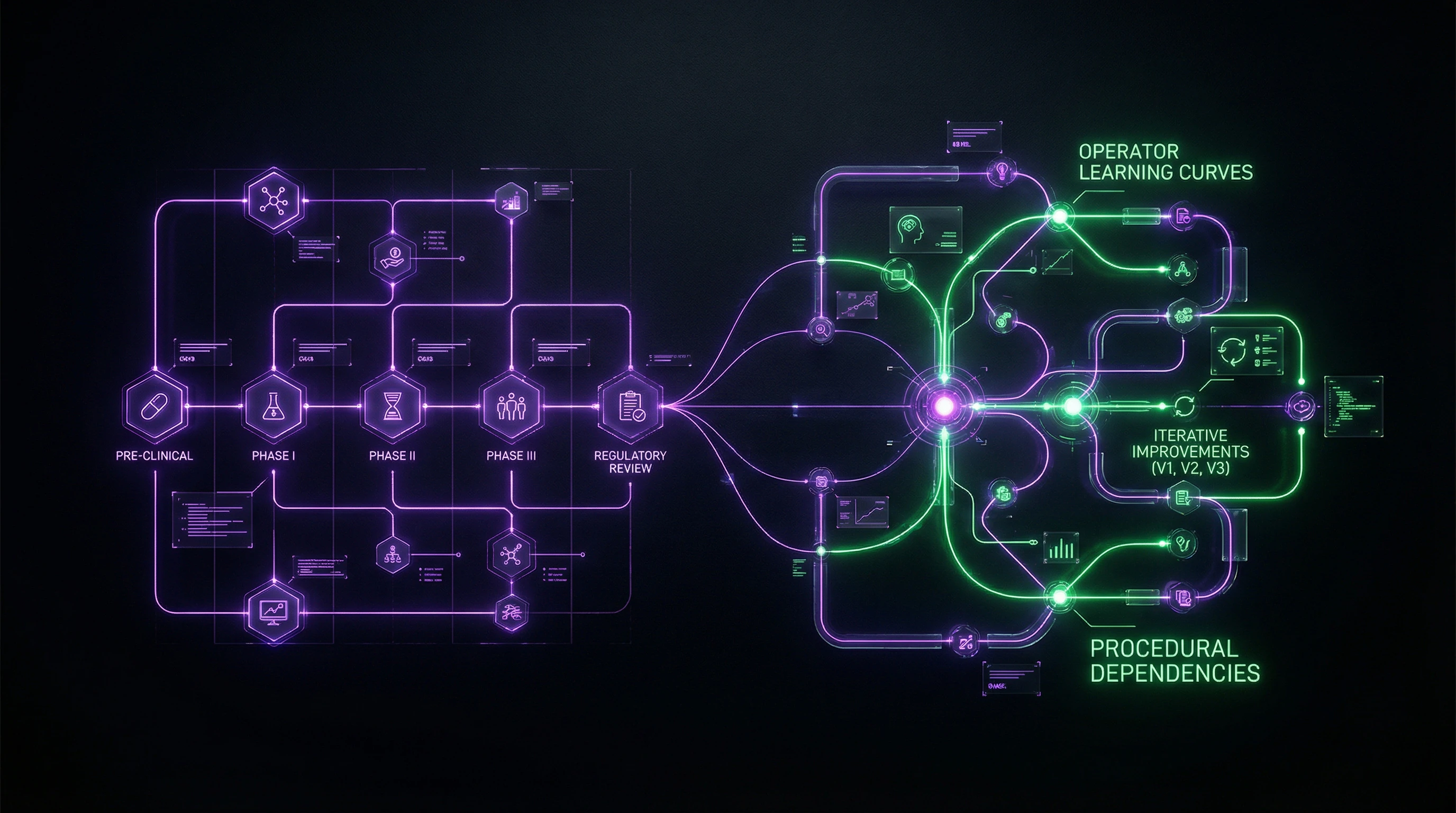
Systematic Literature Reviews for Devices: Adapting Methodology to Data Reality
Systematic reviews for medical devices and diagnostics require substantial adaptations from pharmaceutical methods. Key challenges: small sample sizes, high intervention heterogeneity, operator skill-dependent outcomes.
Methodological Adaptations for Devices and Diagnostics
Clinical validation of devices is a continuous process throughout the product lifecycle. Methodology must account for procedural dependencies and learning effects that influence data interpretation.
Economic impact assessment becomes mandatory for diagnostic modalities. Literature reviews must cover not only clinical effectiveness but also cost analysis, budget impact, and real-world applicability.
| Key Parameter | Pharmaceuticals | Devices and Diagnostics |
|---|---|---|
| Sample Size | Large RCTs (hundreds–thousands) | Often small (tens–hundreds) |
| Heterogeneity | Relatively controlled | High: models, techniques, operator experience |
| Learning Effect | Minimal | Critical for interpretation |
| Economic Synthesis | Supplementary analysis | Embedded in validation |
Working with Heterogeneous Data and Small Samples
Device studies often have smaller sample sizes than pharmaceutical trials. This creates statistical challenges for meta-analysis and evidence synthesis.
Operator-dependent outcomes add an additional layer of variability. Qualitative evidence synthesis becomes critical when quantitative meta-analysis is impossible due to high heterogeneity.
Data heterogeneity in device studies is not an obstacle but the norm. Methodology must anticipate this, not ignore it.
- Apply Bayesian approaches to handle small samples
- Use network meta-analysis methods to integrate indirect comparisons
- Conduct qualitative synthesis when quantitative analysis is limited
- Document learning effects and procedural dependencies
- Stratify results by operator experience and device model
Clinical Validation and Regulatory Requirements: From EU MDR to Post-Market Surveillance
EU MDR and IVDR rewrote the rules for medical devices and diagnostics. The regulations established strict safety reporting requirements to Notified Bodies and created a comprehensive vigilance system.
Market authorization is not the finish line—it's the starting line. NICE guidance and HTA assessments significantly influence the practical application of devices in clinical settings.
EU MDR and IVDR Evidence Requirements
The regulations require systematic reporting of adverse events and safety incidents. Clinical validation is no longer a one-time event, but a continuous process of ensuring quality, safety, and effectiveness throughout the product lifecycle.
| Requirement | EU MDR | IVDR |
|---|---|---|
| Clinical Evidence | Corresponds to risk class; clinical trials for high-risk devices | Rigorous assessment of analytical and clinical validity, especially for critical decisions |
| Risk Classification | Four classes (I–IV) | Four categories with enhanced requirements for diagnostics |
| Post-Market Surveillance | Mandatory for all classes | Mandatory; real-world registries encouraged |
Post-Market Surveillance and Implementation Variability
After market authorization, significant variability in technology adoption is observed. This phenomenon underscores the critical role of post-market surveillance and real-world data collection.
- Organizational barriers: incompatibility with existing infrastructure, staff retraining requirements.
- Clinical integration: adapting the device to routine clinical pathways and workflows.
- Economic factors: reimbursement, budget constraints, cost-effectiveness analysis in real-world settings.
- Evidence generation: collecting data on long-term safety and effectiveness outside controlled trials.
Early adoption of medical innovations faces barriers related to evidence generation, reimbursement, and clinical integration. Post-market studies and real-world registries become critically important for demonstrating long-term safety, effectiveness, and economic value of devices in diverse clinical settings.
Evidence for routine practice implementation requires consideration of practical factors beyond clinical trials: organizational barriers, staff training, integration into existing clinical pathways.
Pharmacoeconomic Evaluation of Diagnostic Technologies: From Clinical Effectiveness to Budget Impact
Economic Impact Models for Diagnostic Devices
Health technology assessment requires demonstrating value beyond clinical effectiveness. Pharmacoeconomic models for diagnostic devices must account for cascade effects: how test results influence therapeutic decisions, alter treatment trajectories, and prevent costly complications.
Economic impact analysis includes three components: direct testing costs, indirect costs of subsequent patient management, and potential savings from early diagnosis or prevention of ineffective treatment.
| Methodological Approach | Effectiveness Unit | Application |
|---|---|---|
| Cost-effectiveness | Correctly established diagnoses, prevented outcomes | Comparison of diagnostic technologies |
| Cost-utility | QALY (quality-adjusted life years) | Assessment of impact on patient quality of life |
Systematic literature reviews establish clinical and economic evidence for in vitro diagnostic devices. Health technology assessment requirements vary by jurisdiction, with growing recognition of the need for specialized criteria for devices and diagnostics.
Budget Impact Analysis and Pricing
Budget impact analysis complements cost-effectiveness analysis with a financial affordability perspective for the healthcare system. It evaluates the aggregate financial consequences of implementing a new diagnostic technology in a defined population over a specific time horizon.
- Define technology utilization volumes in the target population
- Calculate direct costs per test unit and indirect costs for results management
- Assess displacement of existing diagnostic methods and resource liberation
- Model financial impact on healthcare system budget over 3–5 years
- Link results to clinical evidence to justify pricing position
Medical device pricing requires balancing development cost recovery, market competitiveness, and value demonstration for payers. Without this balance, technology is either inaccessible to patients or economically unsustainable.
Strategic pricing links the financial model to clinical evidence, creating a foundation for negotiations with regulators and healthcare systems.
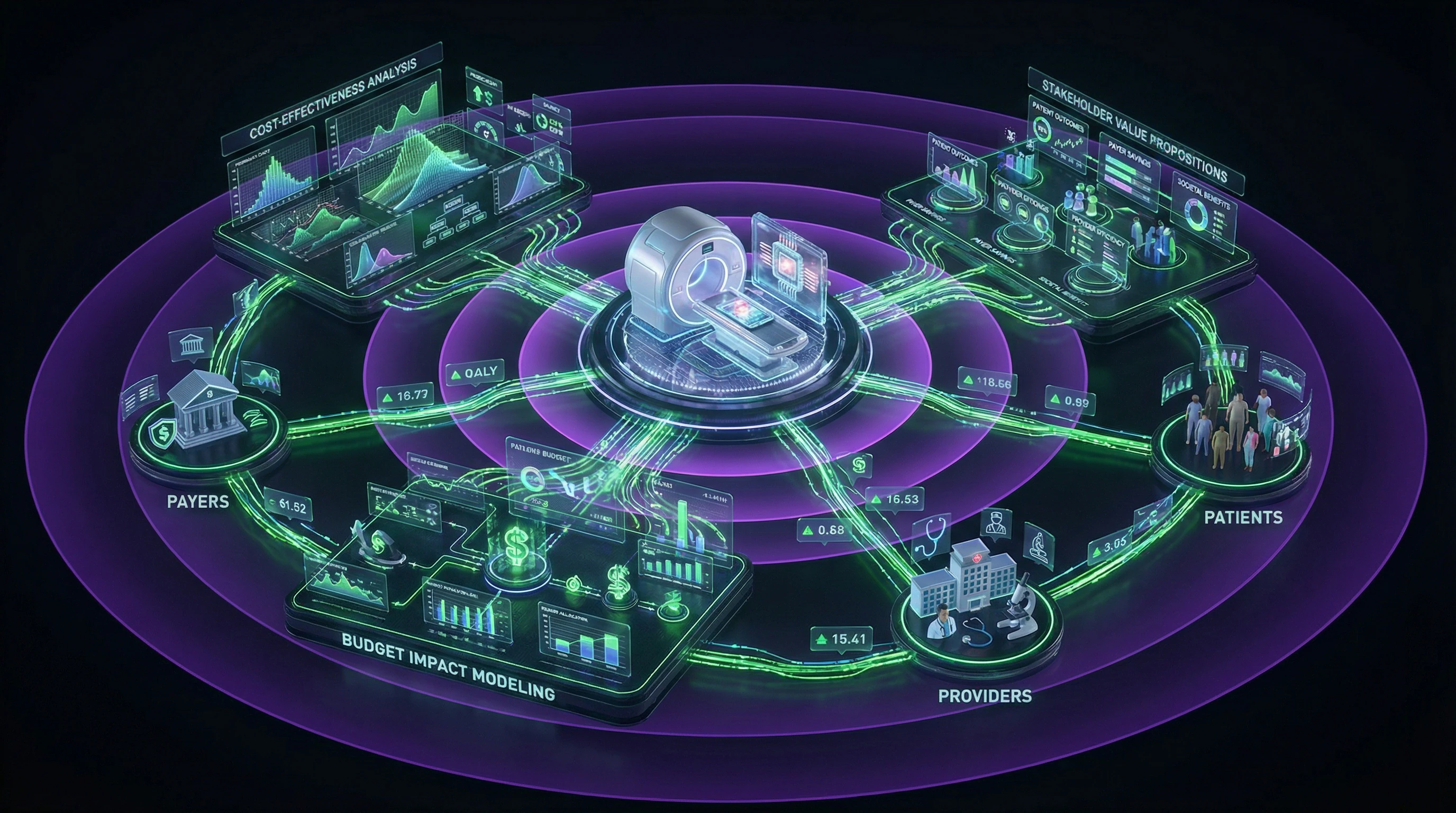
Market Access Pathways and Reimbursement: Navigating the Regulatory Landscape
NICE Medical Technologies Guidance and Specialized Evaluation Pathways
The Medical Technologies Advisory Committee (MTAC) within NICE determines appropriate evaluation pathways for devices and diagnostics. Marketing authorization alone does not guarantee adoption — NICE guidance and HTA assessments substantially influence practical implementation in the healthcare system.
The EU regulatory landscape (MDR and IVDR) has established safety reporting requirements to notified bodies. Innovators must demonstrate value beyond clinical efficacy: economic impact and real-world effectiveness.
- Begin evidence generation in early development stages
- Examine HTA requirements in target markets
- Clarify jurisdiction-specific evaluation criteria for devices and diagnostics
- Prepare economic justification parallel to clinical data
Implementation Variability Following Regulatory Approval
Following marketing authorization and positive NICE recommendations, significant variability in technology adoption is observed. The gap between regulatory approval and widespread clinical use arises from barriers in evidence generation, reimbursement, and clinical integration.
Organizational readiness, availability of staff training, compatibility with existing clinical pathways, and local budget constraints determine the speed and scale of innovation adoption, not just its regulatory status.
Successful implementation requires additional value demonstration and targeted support at the healthcare organization level. Strategy must include local training, adaptation to existing workflows, and transparent cost justification for decision-makers.
Generating Real-World Evidence: From Controlled Trials to Routine Use
Study Design for Medical Devices and Diagnostics
Clinical validation establishes that a device or diagnostic tool functions as intended in clinical settings. Study designs must account for iterative improvements, operator learning curves, and the dependence of outcomes on procedural factors.
Systematic reviews for devices adapt to smaller sample sizes, intervention heterogeneity, and operator-dependent outcomes. Complex diagnostic scenarios—coinfections, multi-organ involvement—require metagenomic and multiplex platforms.
- Evidence for routine practice must include organizational barriers and staff training
- Integration into existing clinical pathways is a mandatory validation criterion
- Advanced methodologies compensate for limitations of traditional RCTs
Monitoring Effectiveness in Routine Clinical Practice
Post-market studies and real-world registries demonstrate long-term safety, effectiveness, and economic value across diverse clinical settings. Monitoring systems collect data on clinical outcomes, usage patterns, adverse events, and economic indicators.
Regulatory requirements of MDR and IVDR create a structured framework for systematic collection of safety and effectiveness data in real-world conditions—this is not bureaucracy, but a feedback mechanism for iterative improvement.
Integration of real-world data with traditional clinical trials creates a complete picture of effectiveness and safety. Machine learning and artificial intelligence reveal patterns not evident in controlled settings.
| Evidence Source | Advantages | Limitations |
|---|---|---|
| Controlled RCTs | High internal validity, bias minimization | Narrow inclusion criteria, artificial conditions |
| Real-world registries | Representativeness, long-term data, patient diversity | Confounding, incomplete data, selection bias |
| Big data analysis + ML | Hidden pattern detection, scalability | Requires validation, overfitting risk |

Knowledge Access Protocol
FAQ
Frequently Asked Questions
Medical devices require specialized HTA approaches distinct from pharmaceuticals. Key differences include iterative design improvements, operator skill dependence, learning curves, and procedural factors not characteristic of drugs. Standard drug evaluation methods don't account for these device and diagnostic-specific features.
It's a methodical process of collecting, critically appraising, and synthesizing clinical and economic data on medical technologies. Reviews are essential for establishing the evidence base for IVD devices and other medical technologies. The methodology adapts to device specifics and the heterogeneity of available data.
The EU operates under MDR (for medical devices) and IVDR (for in vitro diagnostics) regulations. They establish requirements for safety reporting to notified bodies and clinical validation. These regulations ensure post-market surveillance throughout the product lifecycle.
No, regulatory approval doesn't guarantee market success. After obtaining clearance and NICE recommendations, significant variability in technology adoption and diffusion is observed. Additional demonstration of value, economic impact, and practical implementation support are required for real-world success.
Assessment includes analysis of economic impact on the healthcare system and budget impact. For diagnostic technologies, specialized models are built accounting for changes in clinical pathways, diagnostic accuracy, and subsequent therapeutic decisions. Cost analysis and pricing are critical for HTA evaluation.
It's the process of confirming that a device performs as intended in clinical settings. Validation ensures the technology's quality, safety, and effectiveness. It's a continuous process throughout the product lifecycle, especially important for iteratively evolving devices.
NICE evaluates the value proposition of medical technologies through the specialized MTAC committee and determines evaluation pathways. NICE recommendations influence technology adoption in the NHS and serve as a benchmark for procurement. Positive NICE guidance significantly increases chances of widespread device adoption.
Adoption variability relates to barriers in evidence generation, reimbursement, and clinical integration. Even after approval and positive recommendations, time is needed for staff training, process adaptation, and demonstration of real-world effectiveness. Local factors and resources also influence adoption speed.
Special study designs are required that account for practical factors beyond clinical trials. Monitoring effectiveness in routine practice is necessary, considering learning curves, operator variability, and application conditions. Post-market registries and observational studies complement RCT data.
This is a myth—economic evaluation is critically important for devices and diagnostics. Innovators must demonstrate value, not just clinical effectiveness, but economic impact as well. HTA requirements are growing across all jurisdictions, and without health economic justification, reimbursement is unlikely.
No, diagnostic technologies require specific evaluation methodologies. It's necessary to account for impact on clinical decisions, changes in therapeutic pathways, and cascading effects of diagnostic accuracy. Direct transfer of pharmaceutical evaluation methods ignores the unique characteristics of diagnostic technologies and leads to incomplete assessment.
IVD (in vitro diagnostic) devices are medical devices for analyzing biological samples (blood, tissue, urine) outside the body. They require systematic literature reviews to establish clinical evidence and fall under the IVDR regulation in the EU. Evaluation includes analytical and clinical validation, as well as economic analysis.
Continuous design improvements create challenges for traditional HTA methods designed for static technologies. Adaptive evaluation approaches are required that account for device evolution and data accumulation. Clinical validation becomes an ongoing process rather than a one-time event before market entry.
Major barriers include insufficient evidence base in early stages, reimbursement uncertainty, and clinical integration complexities. Early innovators face requirements to generate data under conditions of limited application experience. Regulatory and HTA processes are often not adapted for evaluating breakthrough technologies with limited data.
Metagenomics represents an advanced solution for identifying complex diagnostic scenarios with multiple pathogens. The technology enables simultaneous identification of different pathogens without prior hypotheses. Implementation of metagenomic diagnostics requires new clinical and economic evaluation methodologies that account for the complexity of result interpretation.
Post-market surveillance ensures continuous monitoring of safety and effectiveness in real-world conditions. MDR and IVDR regulations require systematic reporting of adverse events and quality issues. This enables identification of rare complications, evaluation of long-term outcomes, and adjustment of usage recommendations based on accumulated experience.
