What "detox" means in marketing versus detoxification in physiology—the gap between promises and biochemistry
The term "detox" in a commercial context has no clear medical definition. Analysis of popular online "liver cleanse" products showed that most contain no specific information about which substances they supposedly remove from the body (S003).
This isn't accidental—it's strategy: vagueness allows selling the same solution for any complaint. When a product doesn't name specific substances, it's impossible to test for effectiveness. More details in the Fake Diagnostics section.
In physiology, detoxification is a continuous biochemical process in which the liver transforms lipophilic (fat-soluble) compounds into water-soluble metabolites for elimination through the kidneys and bile.
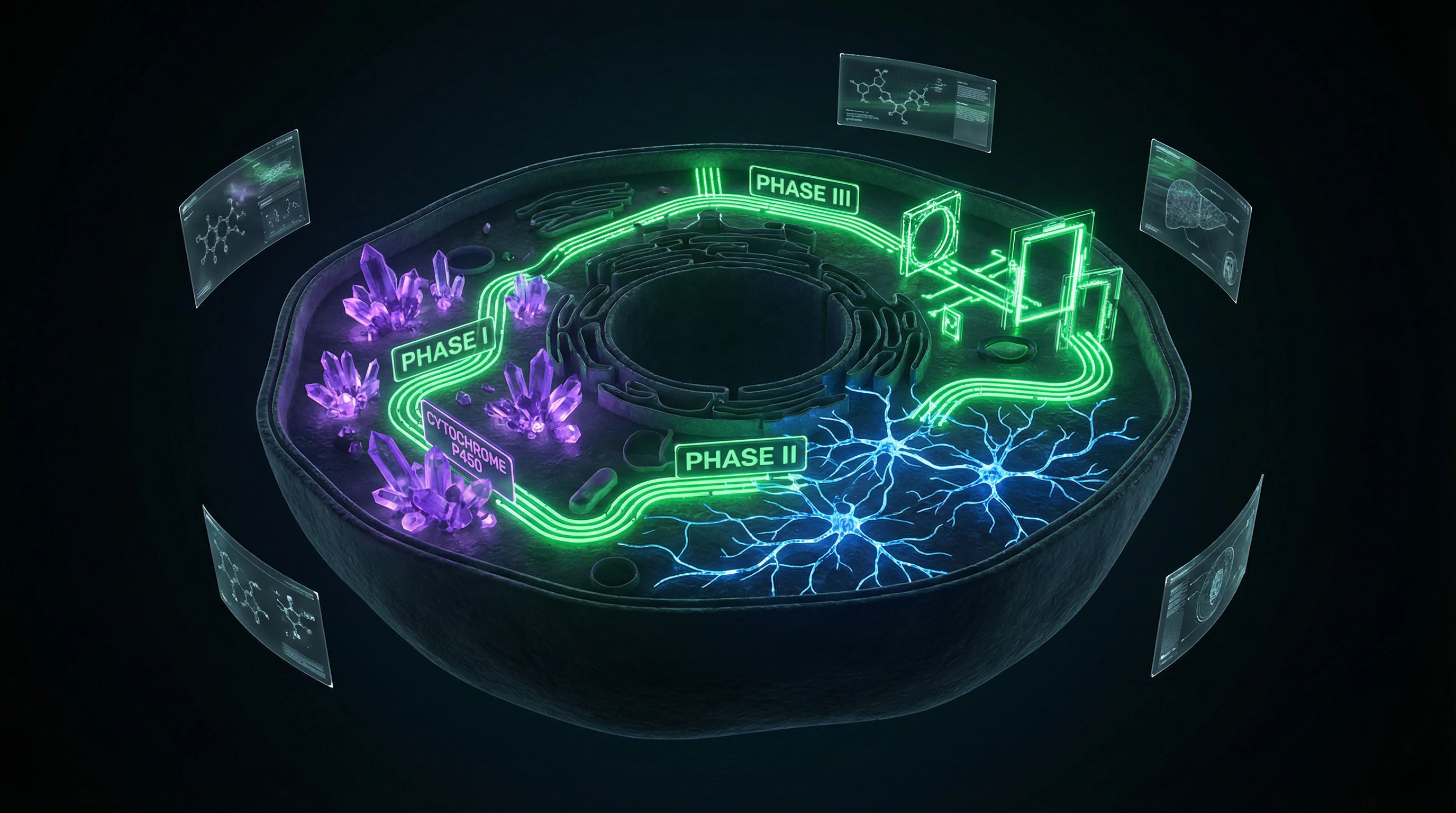
This process is divided into three phases: phase I (oxidation via cytochrome P450), phase II (conjugation with glutathione, sulfates, glucuronides), and phase III (transport of metabolites out of cells) (S001). The liver processes not only exogenous toxins (alcohol, drugs, pesticides) but also endogenous metabolites (ammonia, bilirubin, hormones).
Why "toxins" in detox marketing remain unnamed
The environment contains approximately 80,000 new chemical compounds registered by the U.S. Environmental Protection Agency, but many haven't undergone thorough human health risk assessment (S001). This uncertainty creates fertile ground for exploiting fear.
- Substances are toxic only depending on dose
- Even water can be toxic with excessive consumption (hyponatremia). The lack of specificity in detox products is protection against falsification.
- Marketing vagueness
- If you don't name specific substances, it's impossible to verify effectiveness or file claims.
The boundary between supporting metabolism and "cleansing"
There's a difference between supporting normal detoxification function and claims about "eliminating accumulated toxins." The former has physiological basis: adequate antioxidant supply is necessary for maintaining metabolic homeostasis and reducing oxidative stress during detoxification (S001).
| Detoxification support | Marketing "cleanse" |
|---|---|
| Providing substrates for enzymes | Promise to eliminate "accumulated toxins" |
| Antioxidant protection | Assumption that toxins are "stored" in the liver |
| Maintaining homeostasis | Need for special "cleansing" |
The liver doesn't "store" toxins in the sense the detox industry implies. It continuously metabolizes and eliminates substances. Fat-soluble compounds can accumulate in adipose tissue (e.g., persistent organic pollutants), but detox programs don't directly affect these depots—mobilization of such substances occurs with reduction of adipose tissue mass.
When adipose tissue is lost, accumulated substances temporarily increase their concentration in the blood. This isn't "cleansing"—it's a side effect of fat metabolism that can be either beneficial or require caution depending on the substance and mobilization rate.
Five Strongest Arguments for Detox Programs — and Why They Require Critical Analysis
To avoid strawman arguments, let's examine the most compelling arguments from detox program proponents, based on real physiological processes and preliminary research. For more details, see Folk Medicine vs Evidence-Based Medicine.
🔬 Argument 1: Modern Toxic Burden Is Unprecedented and Requires Support
The environment does contain thousands of synthetic compounds that didn't exist 100 years ago. These substances enter food chains and agricultural production systems, and health risk assessment is limited due to lack of information about their long-term toxicity and exposure levels (S001).
However, the critical question is: does the presence of new chemicals in the environment prove that the liver and kidneys cannot process them without special programs? Evolutionarily, detoxification systems developed to process a wide spectrum of natural toxins (plant alkaloids, mycotoxins, bacterial metabolic products). Cytochrome P450 enzymes possess broad substrate specificity precisely because the body has always encountered diverse xenobiotics.
- New synthetic substances are real, but not proof of inadequate detoxification organs.
- Evolutionary adaptation of detoxification systems to natural toxins suggests the ability to handle unknown compounds.
- Lack of long-term toxicity data is an argument for regulation and monitoring, not for commercial programs.
📊 Argument 2: Studies Show Improvement in Detoxification Markers
A randomized controlled trial with 32 participants showed that a 28-day metabolic detoxification program with a multi-component supplement increased Phase II detoxification enzyme activity compared to a control group that received only an educational session about healthy eating (S001). Intervention group participants showed statistically significant increases in glutathione-S-transferase activity and other conjugating enzymes.
Increased enzyme activity ≠ clinically significant health improvement. This distinction is critical for evaluating any intervention.
Three questions remain unanswered: (1) Does increased enzyme activity mean clinically significant health improvement? (2) Were participants initially deficient in these nutrients? (3) Could the same effect be achieved simply by improving the basic diet without special supplements?
🧬 Argument 3: Dietary Fiber Affects the Gut-Liver-Kidney Axis
The molecular mechanisms by which dietary fiber alters gut, liver, and kidney physiology are likely related to gut-localized events (bacterial nitrogen metabolism, microbe-microbe and microbe-host cell interactions), combined with specific factors originating from the gut in response to fiber (S008).
Dietary fiber does affect the microbiome, short-chain fatty acid production, intestinal barrier function, and systemic inflammation. However, this isn't "detox" in the commercial sense — it's normal physiological function that works with adequate fiber intake (25–30 g/day).
- Adequate Fiber Intake
- 25–30 g per day from vegetables, fruits, whole grains, and legumes. Most of the population doesn't reach this level.
- Why This Isn't Detox
- This is basic physiology, not special "cleansing." The solution is permanent dietary change, not a short-term program.
🧪 Argument 4: Phytonutrients Stimulate Detoxification Enzymes
Certain classes of phytonutrients may help support the detoxification process by stimulating the liver to produce detoxification enzymes or acting as antioxidants (S001). For example, sulforaphane from cruciferous vegetables induces Phase II enzymes through activation of the Nrf2 transcription factor (S006).
This is a mechanistically sound argument, but it supports not detox programs, but rather permanent inclusion of diverse plant foods in the diet. Cruciferous vegetables (broccoli, cabbage, kale), turmeric, green tea, and berries contain compounds that modulate detoxification enzyme expression — but these effects are achieved through regular consumption, not short-term "cleanses."
🛡️ Argument 5: Detox Programs Include Beneficial Lifestyle Changes
Many detox programs recommend eliminating alcohol, processed foods, added sugars, increasing water intake, vegetables and fruits, improving sleep, and reducing stress. These changes are indeed beneficial for liver health and overall metabolism.
Improved well-being after a detox program is the result of a healthy lifestyle, not "toxin elimination." This doesn't prove detox effectiveness, but demonstrates the effectiveness of healthy habits.
The critical question: are these improvements the result of "detoxification" or simply the result of temporary lifestyle improvement? If someone transitions from a diet high in processed foods, alcohol, and sugar to a diet rich in vegetables and whole foods, improved well-being is expected — but this doesn't prove that "toxin elimination" occurred.
It simply demonstrates that a healthy lifestyle improves health. The question is why these changes need to be packaged in a "detoxification" narrative instead of an honest conversation about how normal physiology works.
Evidence Base for Detox Programs: What Systematic Reviews and Randomized Studies Show
A systematic analysis of popular online "liver cleanse" products revealed a critical problem: most don't specify which toxins they target, mechanisms of action, or clinical evidence (S003). This isn't a lack of information—it's a structural problem with an industry selling solutions to nonexistent problems.
A product without a defined problem isn't treatment—it's marketing.
Controlled Studies: What They Actually Measure
A randomized study with 32 participants evaluated a 28-day metabolic detoxification program (S001). The intervention group received a multi-component whole-food supplement, while the control group received education and healthy eating guidance.
Result: statistically significant increase in Phase II detoxification enzyme activity in the intervention group. More details in the Folk Medicine vs. Evidence-Based Medicine section.
- Small sample size (power calculation required 15–20 participants)
- Short duration (4 weeks)
- No long-term follow-up
- Measured only enzyme activity, not health outcomes or disease incidence
Other trials showed high variability due to genetic differences (S001). Polymorphisms in CYP450, GSTM1, GSTT1 genes mean that even if an intervention modulates enzymes, the effect varies substantially between individuals.
Milk Thistle: The Most Studied Ingredient
Milk thistle (silymarin) has shown potential hepatoprotective effects and improvements in cholesterol, insulin resistance, and inflammatory markers (S004). These are real effects, but not what detox programs promise.
There's no evidence that milk thistle "detoxifies" the liver. Evidence is contradictory or based on poor study design (S010).
The same applies to artichoke, dandelion, and other herbs—no evidence they eliminate toxins or detoxify the liver (S010).
Detox Diets in the Context of Fad Diets
A systematic review of fad diets identified eight characteristics that distinguish them from healthy eating patterns (S011):
| Fad Diet Characteristic | Detox Diets |
|---|---|
| Promise rapid weight loss | "7-day cleanse" |
| No physical activity recommendations | Focus only on nutrition |
| Short-term changes, not sustainable goals | Program-based approaches |
| Exclude entire food groups | Often exclude carbs, fats |
| Not sustainable long-term | Impossible to maintain permanently |
| Questionable nutritional adequacy | Micronutrient deficiencies |
| No warnings for people with chronic conditions | Dangerous for diabetes, hypertension |
| Lack scientific evidence | Marketing instead of research |
Detox diets meet all eight criteria. They're not designed for long-term adherence and lack a reliable evidence base.
Dietary Fiber: A Mechanism with Real Evidence
Unlike commercial detox programs, the impact of dietary fiber on detoxification organs has a solid foundation. Fiber alters the intestinal environment, affecting gut, liver, and kidney function through local and systemic signaling networks (S008).
- Why This Matters
- Different fiber types produce different outcomes—enabling specific recommendations for reducing liver lipids in non-alcoholic fatty liver disease or lowering creatinine in chronic kidney disease (S008).
- Long-Term Effect
- Fiber consumption has declined since the Industrial Revolution. Mice on low-fiber diets showed reduced microbial diversity that didn't recover after fiber reintroduction (S008). Chronic low fiber intake may have irreversible effects on the microbiome.
This isn't marketing—it's a mechanism with evidence. Fiber works not because it "cleanses," but because it supports normal detoxification organ function.

Detoxification Mechanisms: What Actually Happens and Why Your Liver Doesn't Need "Cleansing"
The liver performs over 500 functions, including nutrient metabolism, protein synthesis, bile production, and detoxification. Detoxification is not a separate function that can be "turned on" or "enhanced" by a short-term program, but a continuous process integrated into all aspects of hepatic metabolism. Learn more in the Mental Bugs section.
⚙️ Three-Phase Detoxification System: Biochemistry Without Mysticism
Phase I detoxification involves cytochrome P450 enzymes (CYP450), which catalyze oxidation, reduction, and hydrolysis reactions. These reactions often make compounds more reactive, creating intermediate metabolites that can be more toxic than the original substance.
Adequate antioxidant supply is necessary to maintain metabolic homeostasis and reduce oxidative stress during detoxification (S001).
Phase II involves conjugation — attaching water-soluble molecules (glutathione, sulfates, glucuronides, acetyl groups) to Phase I metabolites. These reactions are catalyzed by enzymes such as glutathione-S-transferases (GST), UDP-glucuronosyltransferases (UGT), sulfotransferases (SULT), and N-acetyltransferases (NAT). Conjugation increases water solubility and typically reduces toxicity.
Phase III involves transport proteins that actively export conjugated metabolites from liver cells into bile or blood for elimination through the intestines or kidneys. These transporters include P-glycoprotein, multidrug resistance proteins (MRP), and organic anion transporters (OAT).
🧬 Genetic Polymorphism: Why Detoxification Is Individual
Clinical trials investigating strategies to enhance detoxification pathways have shown high variability due to genetic and gender differences (S001). Polymorphisms in CYP450 genes (e.g., CYP1A2, CYP2D6, CYP3A4) can alter the rate of drug and toxin metabolism by 10–100 times between individuals.
- Rapid Metabolizers
- Individuals with high detoxification enzyme activity; risk — insufficient accumulation of protective metabolites.
- Slow Metabolizers
- Individuals with low activity; risk — accumulation of toxic intermediate products.
- Phase II Polymorphisms (GSTM1, GSTT1)
- Approximately 50% of the European population has a GSTM1 gene deletion, which reduces the ability to conjugate certain toxins with glutathione and increases susceptibility to oxidative stress.
This genetic variability means that one-size-fits-all detox programs cannot be optimal for everyone. Claims that a particular program will "cleanse" everyone equally effectively ignore biological reality.
🔄 Enterohepatic Circulation: Why "Toxins" Can Return
Some conjugated metabolites excreted in bile can be deconjugated by intestinal bacteria and reabsorbed into the bloodstream — a process called enterohepatic circulation. This is a normal physiological mechanism for conserving bile acids, but it can also prolong the presence of some toxins in the body.
| Mechanism | Effect | Duration |
|---|---|---|
| Dietary fiber binds bile acids and toxins in the intestine | Interrupts enterohepatic circulation, promotes fecal elimination | Continuous effect with adequate fiber intake |
| Short-term detox programs | Temporary increase in fiber intake | Ceases after program ends |
Dietary fiber supports detoxification through the continuous effect of adequate intake, not through short-term "cleansing" (S008).
🧪 Kidneys: The Underappreciated Detoxification Organ
The kidneys filter approximately 180 liters of blood per day, removing water-soluble waste and toxins through urine. They also regulate electrolyte balance, acid-base balance, and blood pressure.
Chronic kidney disease (CKD) is associated with accumulation of uremic toxins, many of which are produced by intestinal bacteria from dietary proteins (indoxyl sulfate, p-cresyl sulfate). Dietary fiber can reduce production of these toxins by altering microbial metabolism and increasing their elimination through the intestines (S008).
- Intestinal bacteria metabolize dietary proteins, producing uremic toxins.
- Dietary fiber alters microbiota composition and reduces toxin production.
- Increased toxin elimination through the intestines reduces kidney burden.
- This effect requires continuous fiber intake, not short-term intervention.
Supporting kidney function is a matter of hydration, adequate electrolyte intake, and minimizing nephrotoxic substances (excess sodium, certain medications). Detox programs do not address these fundamental needs.
🔬 Why the Liver Doesn't Need "Cleansing"
The liver is a self-regenerating organ with built-in mechanisms to protect against overload. When detoxification pathways are overwhelmed, the liver activates stress-response pathways, including reality-checking its own recovery capabilities.
The liver does not accumulate "toxins" that need to be eliminated by a special program. It either successfully metabolizes substances, or they accumulate in adipose tissue or other organs — and no detox drink will change this biochemistry.
If the liver is damaged (cirrhosis, hepatitis, fatty liver disease), detox programs can be dangerous, as they often contain substances requiring hepatic metabolism. Supporting the liver during disease requires medical supervision, not marketing promises.
Real detoxification support means minimizing toxin exposure (quitting smoking, reducing alcohol, avoiding pollution), adequate nutrition (especially antioxidants and fiber), regular physical activity, and sufficient sleep. These factors support all three phases of detoxification without the need for special programs or supplements.
